Posted on Dec 4, 2018 in Original Article |
Patients’ Attitudes Towards Text Messages about HIV and Hepatitis C Screening
Julika Kaplan, MD1, Haley Marek, BS2, Monisha Arya, MD, MPH1,3
1 Department of Medicine, Baylor College of Medicine, Houston, TX, USA
2 School of Medicine, Baylor College of Medicine, Houston, TX, USA
3 Center for Innovations in Quality, Effectiveness and Safety, Michael E. DeBakey VA Medical Center, Houston, TX, USA
Corresponding author: julika.kaplan@bcm.edu
Journal MTM 7:2:51–54, 2018
doi:10.7309/jmtm.7.2.7
Background: Despite the prevalence of HIV and hepatitis C virus (HCV), many people in the United States have never been screened for these infections. Mobile phones could educate patients about screening recommendations and “nudge” them to request screening from their physicians. There is a need for studies to understand patients’ perspectives on this campaign strategy.
Aims: The purpose of this pilot study is to describe patients’ attitudes towards text messages that educated them about HIV and HCV and “nudged” them to discuss screening recommendations with their physicians.
Methods: In 2016 and 2017, patients in primary care clinics in Houston, Texas were recruited to participate in text message studies promoting HIV and HCV screening. Participants were sent either HIV, HCV, or control text messages prior to their individual primary care appointments. After the appointment, research staff called the participants and conducted evaluation surveys to determine whether they enjoyed receiving health-related text messages and to elicit their opinions about the specific content of the messages.
Results: The majority of our participants appreciated the text messages, specifically because they provided valuable health information that was unfamiliar to the patients and prompted them to discuss HIV and HCV screening with their physicians.
Conclusion: Our pilot study demonstrated that the majority of patients enjoyed receiving text message-based “nudges” because they helped them overcome barriers to healthy behavior and may have improved patient-physician communication. These findings are important because this strategy can improve screening rates in primary care for infections such as HIV and HCV.
Keywords: Text Messaging, Hepatitis C, HIV Infections, Mobile Health, Pilot Projects
Introduction
Despite the prevalence of HIV and hepatitis C virus (HCV), many people in the United States have never been screened for these infections.1,2 This is partially due to a lack of physician awareness of national screening recommendations.3,4,5 Screening and early detection are critical to improving health outcomes for HIV and HCV, so strategies to increase routine screening in healthcare are necessary.6,7 While improving physician awareness of screening recommendations could be one approach, a patient-focused strategy may be to use mobile health (mHealth) technology to provide targeted health information directly to patients. Mobile phones, specifically, could educate patients about screening recommendations and “nudge” them to actively engage in their healthcare.8 In the case of health, “nudging” involves using interventions to help people overcome the barriers that may be limiting their ability to obtain optimal healthcare.9 We developed text message campaigns in which we educated patients about HIV and HCV and “nudged” them to discuss screening with their physicians. The purpose of this pilot study is to describe patients’ attitudes towards these HIV and HCV text messages.
Methods
In 2016 and 2017, patients in primary care clinics in Houston, Texas were recruited to participate in mHealth text message studies promoting HIV and HCV screening. During the consent process, patients were informed that they would receive a message either about HIV, HCV, or a different health topic. Patients who participated had mobile phones, used text messaging, and provided informed consent. Participants in the HIV study were sent an HIV text message or a control text message, and participants in the HCV study were sent an HCV text message or a control text message. Each message included a one-sentence fact about HIV or HCV and a prompt encouraging participants to talk to their physicians about screening. The messages were sent within the hour prior to their individual primary care appointments. After the appointment, research staff called the participants and conducted evaluation surveys to determine whether they enjoyed receiving health-related text messages and to elicit their opinions about the specific content of the messages. The Baylor College of Medicine Institutional Review Board approved these studies.
Results
For both our HIV and HCV campaigns, we found that the majority of participants enjoyed receiving text messages with health information. Our post-text evaluation surveys provided insight into why our participants did or did not enjoy receiving health-related messages before their appointments with their physicians.
Out of our 12 HIV text message recipients, 11 (92%) enjoyed receiving a health-related text message, while one (8%) did not. Those who enjoyed receiving the message cited the following reasons: seven (64%) appreciated a health reminder, two (18%) felt that the message provided valuable information relevant to their health, and one (9%) believed that texting was more effective than calling as a communication method. A participant who benefitted from the reminder about HIV testing stated, “I liked it because it reminded me to ask my doctor about the HIV test.” Another acknowledged that the text instructed her “to do something that [she] otherwise wouldn’t have asked.” One of the participants who valued the information he received said the message “[kept him] on point” and let him know that he could get an HIV test “without setting a special appointment.” Another participant expressed her belief that “[HIV] is a disease that everyone should be on top of.” Finally, there were several participants who found the text message useful but still confessed that it was “alarming” or “a little disturbing” because people do not normally “send a text message out of the blue about something like [HIV].” On the other hand, the single participant who did not enjoy receiving our HIV text message was concerned that her confidentiality could be breached if a friend saw her phone: “It was a personal message but it was to my phone. I’m okay with it… but it could be a problem… someone snooping could cause a problem.”
Out of the 25 participants who received text messages about HCV, 22 (88%) enjoyed receiving a health-related text message, while two (8%) did not and one (4%) felt neutral. Those who enjoyed receiving the message cited the following reasons: 14 (64%) felt that the message provided valuable information relevant to their health, seven (32%) appreciated a health reminder, and one (5%) believed that receiving the text message was easy and convenient. One participant who was grateful that the text message prompted her to discuss HCV with her physician stated: “At appointments, it’s hard to remember what you want to bring up with your doctor. This text can function as a jumping off point for initial discussion.” Two other participants felt that the text message provided valuable information about their health; one said the message “pertained to an issue most people don’t know about,” and another said he “never thought about a hepatitis C test at [his] age.” One participant who did not enjoy receiving the text message said he “didn’t understand the purpose” of the text message.
Discussion
In this pilot study, we encouraged participants to discuss HIV and HCV screening with their physicians by sending them informative text messages with cues to action prior to their appointments. We learned that participants appreciated our text messages because they provided valuable health information and prompted them to discuss HIV and HCV screening with their physicians. However, despite the consent process, we also found that one patient had concerns about receiving health information on her cell phone that she considered alarming and another patient did not understand the purpose of the text message campaign.
The limitations of this study include a small sample size, which may hinder generalizability. However, this pilot study provides proof of concept for using text messages as an intervention to promote HIV and HCV screening. Another potential limitation is social desirability bias, or participants’ tendency to give responses that will satisfy the research staff. We attempted to mitigate this limitation by emphasizing before participants completed the evaluation survey that there were no correct answers and that their participation would not impact their medical care.
People face many barriers that may negatively impact their ability to make decisions that are good for their health. Examples of these barriers include limited awareness of medical topics, difficulty remembering to ask their providers certain questions, or fear of receiving an unwanted diagnosis, particularly in the case of chronic infections such as HIV and HCV. A “nudge” is a policy change or intervention that helps people overcome these barriers, thereby making it easier for people to act in their own best interest and make healthy decisions. Our study demonstrates that the majority of patients enjoyed receiving a text message-based “nudge” because it helped them overcome two of their most significant barriers: lack of information about screening recommendations and difficulty remembering health information. These findings are important because they can improve screening rates for asymptomatic yet treatable diseases such as HIV and HCV in primary care. Larger studies are needed to confirm our findings and determine the impact on screening rates.
Acknowledgements
The authors would like to thank John Benjamin Kellogg, Jessica Lee, Sharon Joy, and Stephen Manning for their contributions to data collection. The HIV-related work was supported by the National Institute of Mental Health of the National Institutes of Health under Award Number K23MH094235 (Principal Investigator: Arya). This work was also supported in part by the Center for Innovations in Quality, Effectiveness and Safety (#CIN 13-413) of the Michael E. DeBakey Veterans Affairs Medical Center in Houston. The views expressed in this article are those of the authors and do not necessarily represent the views of the National Institutes of Health or of the US Department of Veterans Affairs.
References
1. Dailey AF, Hoots BE, Hall HI, Song R, Hayes D, Fulton Jr P, Prejean J, Hernandez AL, Koenig LJ, Valleroy LA. Vital Signs: Human Immunodeficiency Virus Testing and Diagnosis Delays—United States. Morbidity and Mortality Weekly Report. 2017 Dec 1;66(47):1300–1306. 
2. Smith BD, Morgan RL, Beckett GA, Falck-Ytter Y, Holtzman D, Teo CG, Jewett A, Baack B, Rein DB, Patel N, Alter M. Recommendations for the Identification of Chronic Hepatitis C Virus Infection Among Persons Born During 1945–1965. Morbidity and Mortality Weekly Report: Recommendations and Reports. 2012 Aug 17;61(4):1–32. 
3. Zheng MY, Suneja A, Chou AL, Arya M. Physician Barriers to Successful Implementation of US Preventive Services Task Force Routine HIV Testing Recommendations. Journal of the International Association of Providers of AIDS Care. 2014 May;13(3):200–205.
4. Falade-Nwulia O, McAdams-Mahmoud A, Irvin R, Niculescu A, Page KR, Mix M, Thomas DL, Sulkowski MS, Mehta SH. Primary Care Providers Knowledge, Attitude and Practices Related to Hepatitis C Screening and Treatment in the Oral Direct Acting Antiviral Agents Era. Journal of Community Medicine & Health Education. 2016 Oct;6(5).
5. Thomson M, Konerman MA, Choxi H, Lok AS. Primary Care Physician Perspectives on Hepatitis C Management in the Era of Direct-Acting Antiviral Therapy. Digestive Diseases and Sciences. 2016 Dec 1;61(12):3460–3468. 
6. Moyer VA. Screening for HIV: US Preventive Services Task Force Recommendation Statement. Annals of Internal Medicine. 2013 Jul 2;159(1):51–60. 
7. Younossi Z, Blissett D, Blissett R, Henry L, Younossi Y, Beckerman R, Hunt S. In an Era of Highly Effective Treatment, Hepatitis C Screening of the General Population of the United States for Hepatitis C Should be Considered. Liver International. 2017 Jul 18:38(2):258–265. 
8. Arya M, Kumar D, Patel S, Street Jr RL, Giordano TP, Viswanath K. Mitigating HIV Health Disparities: The Promise of Mobile Health for a Patient-Initiated Solution. American Journal of Public Health. 2014 Dec;104(12):2251–2255. 
9. Thaler RH, Sunstein CR. Nudge: Improving Decisions about Health, Wealth, and Happiness. New Haven, CT. Yale University Press; 1999.
Posted on Dec 4, 2018 in Original Article |
The Role of Text Messages in Patient-Physician Communication about the Influenza Vaccine
Disha Kumar1, BS, BA, Vagish Hemmige2,3, MD, MS, Michael A. Kallen4, PhD, MPH, Richard L. Street Jr.2,5,6, PhD, Thomas P. Giordano2,5, MD, MPH, Monisha Arya2,5, MD, MPH
1School of Medicine, Baylor College of Medicine, One Baylor Plaza, Houston, TX 77030, U.S.A.; 2Department of Medicine, Baylor College of Medicine, Houston, TX, U.S.A.; 3Division of Infectious Diseases, Department of Medicine, Montefiore Medical Center, 3411 Wayne Avenue, Suite 4H, Bronx, NY 10467, U.S.A.; 4Department of Medical Social Sciences, Northwestern University Feinberg School of Medicine, 303 E Chicago Ave, Chicago, IL 60611 U.S.A.; 5Center for Innovations in Quality, Effectiveness and Safety, Michael E. DeBakey VA Medical Center, 2002 Holcombe Blvd (Mailstop 152), Houston, TX 77030, U.S.A.; 6Department of Communication, Texas A&M University, 4234 TAMU, College Station, TX 77843, U.S.A.
Corresponding author: disha.kumar@bcm.edu
Journal MTM 7:2:55–59, 2018
doi:10.7309/jmtm.7.2.8
Background: Racial and ethnic minorities face disparities in receiving the influenza vaccination. A text message intervention could deliver personalized and timely messages to counsel patients on asking their physician for the vaccination.
Aims: We assessed whether patients would be receptive to influenza vaccination text messages.
Methods: Participants were recruited from a sample of low-income, racial and ethnic minority primary care patients. Participants completed a self-administered survey. Descriptive statistics were used to analyze the data.
Results: There were 274 patients who participated and answered the questions of interest, of whom 70% were racial and ethnic minorities and 85% owned a cell phone. Thirty-six percent reported they had never received an influenza vaccination recommendation from their physician. However, 84% would be comfortable asking their physician for the influenza vaccination. Of cell phone-owning participants who would be comfortable asking their physician about the influenza vaccination, 80% would also be comfortable receiving a text message reminder.
Conclusion: Text messages may be an acceptable channel to prompt patients to discuss the annual influenza vaccination with their physicians. Text messaging is a feasible tool to engage patients in their health and improve annual influenza vaccination rates among low-income, racial and ethnic minority patients.
Key words: minority health, healthcare disparities, telemedicine, mHealth, text messaging, influenza vaccination, health communication
Introduction
Text messages may be an effective solution for improving unacceptably low influenza vaccination rates.1 In the U.S. 2017 early-influenza season, only 38% of adults received the influenza vaccine, with 36% of Hispanic adults, 40% of non-Hispanic Black adults, and 38% of non-Hispanic White adults receiving the vaccine.2 In comparison, 41% of adults received the influenza vaccine during the 2016 early-influenza season.2 As recommended by the U.S. Advisory Committee on Immunization Practices, all adults should receive annual influenza vaccination3 to prevent against the life-threatening effects of influenza. The low vaccination rate during the 2017 early-influenza season may in part have led to the relatively high incidence of influenza illness. During the recent 2017-2018 influenza season (1 Oct 2017 to 03 Feb 2018), the weekly percentage of outpatients visits for influenza-like illness ranged from 1.3% to 7.7%, well above the 2.2% national baseline for the prior three seasons.4
The push-pull capacity model5,6 could be adapted to improve influenza vaccination communication between patients and physicians. In this context, an intervention “pushing” the patient to ask their physician about the influenza vaccination may then “pull” the physician into talking about or recommending the vaccine. Arya et al. have illustrated how the push-pull model using text messages could improve communication about and demand for preventive health services.7 As racial and ethnic minorities are more likely to have poorer communication with their physicians,8 adapting the push-pull model using text messages may help improve this communication especially among these groups. Text messaging-based health campaigns have been successful at engaging patients in preventive health behaviors.9 Despite this success, text messages are underutilized in pushing health information to patients to engage them in managing their own health and in particular, improving patient-physician communication. Due to the ubiquity of text messaging, a text message campaign could help reduce the digital divide, which has left certain groups – such as racial and ethnic minorities – with less access to health information.10
Studies have demonstrated that text messages can help improve influenza vaccination rates; however, these studies have focused on improving childhood vaccination (by texting parents) or improving vaccination among pregnant women.11,12 To date, there has been limited research among low-income racial and ethnic minority adults on using text messages to improve patient-physician communication about vaccination. The purpose of this study was to determine if racial and ethnic minority adult patients who had not received an influenza vaccination recommendation would be comfortable 1) receiving a cell phone text message reminder about the vaccination and 2) asking their physicians for the vaccination.
Methods
This study was conducted June 2014 – February 2015 in a primary care clinic that serves low-income, mostly uninsured racial and ethnic minority patients. We recruited a convenience sample of patients to participate in a self-administered survey developed by the research team. Before study initiation, 38 patients pilot-tested the questions to ensure survey comprehensibility. In addition to survey questions on demographics and cell phone ownership, the primary questions were: 1) “Has your doctor at this clinic ever recommended that you get a flu shot?” 2) “How comfortable would you be asking your doctor for the flu shot?” and 3) “Would you be comfortable receiving a text message reminder about the flu shot?” Participants were given a $10 gift card for participating. The Baylor College of Medicine Institutional Review Board approved the study.
Descriptive statistics were used for data analysis. The responses “no” and “did not remember” for question one were combined into the single response category “no.” The responses “comfortable” and “very comfortable” for question two were combined into the single response category “comfortable.” Similarly, the responses “somewhat comfortable” and “not at all comfortable” for question two were combined into the single response category “not comfortable.”
Results
We report data from the 274 participants who answered all three primary questions. Not all 274 participants answered all demographic questions. Of those who answered, the majority were female, had less than a college education, were racial and ethnic minorities, had an income under $20,000/year, and owned a cell phone. Of the 272 participants who responded to age, the median age was 54 years old (Interquartile range: 46-59 years old). See Table 1 for demographic characteristics of study participants.

Table 1: Demographic characteristics of the study population (N=274)
Overall, 98 (36%) had never received an influenza vaccination recommendation from their physician, 230 (84%) would be comfortable asking their physician for the vaccination, and 176 of 234 (75%) cell-phone owning participants would be comfortable receiving a vaccination text message reminder. See Table 2. Of the 98 (36%) participants who indicated they had never received an influenza vaccination recommendation, 77 (79%) would be comfortable asking their physician for the vaccination. Of these 77 participants, 64 (83%) owned a cell phone. Fifty-one (80%) of these 64 participants would be comfortable receiving an influenza vaccination text message reminder. Thus, overall 51 of 98 (52%) participants who had never received an influenza vaccination recommendation would be comfortable asking their physician for the vaccination and may be prompted by a text message to do so. See Figure 1.

Table 2: Results of survey questions pertaining to receiving the influenza vaccination (N=274)
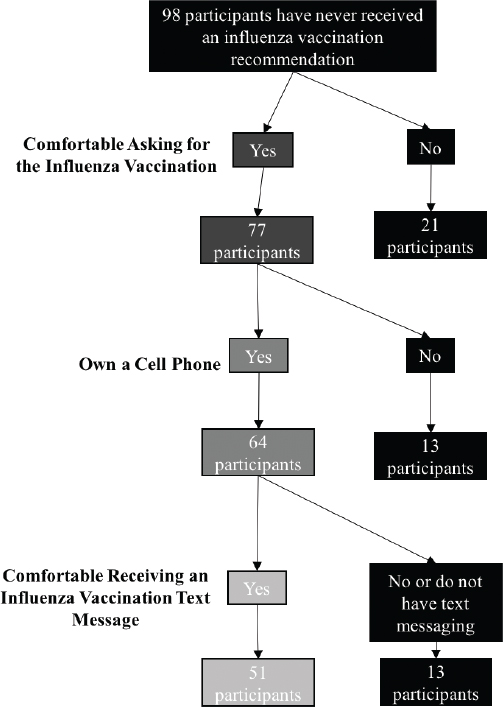
Figure 1: Acceptability of an influenza vaccination text message among participants who have never received a vaccination recommendation from their physician.
Discussion
Interventions are needed to improve vaccination rates, particularly among racial and ethnic minority populations who are traditionally underserved in healthcare. In our study of mostly racial and ethnic minority adults, over one-third of patients did not receive or did not remember receiving an influenza vaccination recommendation from their physician. This highlights the need for strategies to improve vaccination communication between these patients and their physicians. Notably, over three-fourths of patients who had never received an influenza vaccination recommendation from their physician and would be comfortable asking their physician for the vaccination, would also be comfortable receiving the corresponding text message reminder.
Text messages may be particularly suitable for delivering vaccine information in healthcare settings. Texts can be tailored and delivered at a highly pertinent time, such as immediately before a patient enters the examination room. An example of a personalized text message could be: “John, even healthy adults can get the flu and spread it to loved ones. Remind Dr. Jones at your appointment today to talk to you about your yearly flu shot.” This personalized and timely campaign may be more influential at prompting patients to ask for the influenza vaccination than static and non-personalized campaigns. Static campaigns, epitomized by posters in a clinic, may simply go unnoticed among a sea of signs, may not be relatable to the specific patient, or may fail to convince patients who have not already received their annual influenza vaccination. Another benefit of a text message campaign is that it can be integrated into the existing electronic medical record (EMR). Many EMR systems have the capability to send text messages. EMRs are able to extract patient name, physician name, appointment date and time, patient phone number, and lack of receipt of influenza vaccination – all of which can be used to personalize the text message. Thus, the EMR could both personalize and automate text message delivery to patients before a scheduled appointment. For healthcare systems that already use the EMR for appointment reminders, an influenza vaccination campaign could complement the existing reminder. In sum, text messages offer significant opportunity to cost-effectively improve influenza vaccination rates.
While this study offers insight into a strategy to improve influenza vaccination, there are limitations to our findings. Limitations to this study include a relatively small sample size consisting of predominately racial and ethnic minorities and collection of data from one study site. Thus our findings may not be generalizable to other populations. However, our findings may be salient for improving influenza vaccination rates among racial and ethnic adults. An additional limitation is our method of convenience sampling. This may have resulted in a response bias from participants already more inclined to engage in their health; our study sample may therefore be overrepresented by participants willing to talk to their physicians and to receive text message reminders. Our proposed intervention of using text messaging to encourage patient-physician communication about vaccination may therefore be most useful for patients who already actively participate in their health.
Conclusion
Our findings suggest a text message could “push” patients to “pull” their physicians into an influenza vaccination discussion, a step needed to improve vaccination rates among adults. This type of text message campaign could help achieve Healthy People 2020 goals of increased patient-physician communication, greater use of health communication technologies, and increased influenza immunization rates.13 Research is still needed to determine the optimal text message content to best persuade patients about their need for annual influenza vaccination and cue them to engage in an influenza vaccination conversation with their physicians. Physician ordering of the vaccination after a patient prompt would also need to be assessed to provide empirical evidence supporting the push-pull model for influenza vaccination.
Acknowledgements
The authors would like to thank Alexandra Trenary, Sajani Patel, and Ashley Phillips for their contributions to data collection. We would also like to thank Haley Marek for her thoughtful contributions to the manuscript draft.
D. Kumar contributed to literature reviews, study design, data collection and analysis, and the writing of all sections. V. Hemmige contributed to data analysis and the writing of the methods and results sections. M.A. Kallen and R.L. Street contributed to study design. T.P. Giordano contributed to study design and data analysis. M. Arya planned the thematic content and study design, and contributed to data analysis and the writing and editing of all sections. All authors contributed to draft versions of the manuscript and provided editorial suggestions for important intellectual content. All authors read and approved the final version of the manuscript.
Some of the results presented in this manuscript were presented in a poster at the March 10, 2016 Henry J.N. Taub/James K. Alexander Medical Student Research Symposium at the Baylor College of Medicine.
Funding: This work was supported by the National Institute of Mental Health of the National Institutes of Health under Award Number K23MH094235 (PI: Arya). This work was supported in part by the Center for Innovations in Quality, Effectiveness and Safety (#CIN 13-413).
The views expressed in this article are those of the authors and do not necessarily represent the views of the Department of Veterans Affairs, the National Institutes of Health, or Baylor College of Medicine.
Financial Disclosures: No financial disclosures were reported by the authors of this paper.
Research Involving Human Participants: This study was conducted under approval of Baylor College of Medicine Institutional Review Board Protocol H-30232. The study was performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
References
1. Phillips AL, Kumar D, Patel S, Arya M. Using text messages to improve patient–doctor communication among racial and ethnic minority adults: An innovative solution to increase influenza vaccinations. Prev Med. 2014;69:117–119. doi:10.1016/j.ypmed.2014.09.009 
2. U.S. Centers for Disease Control and Prevention. National Early-Season Flu Vaccination Coverage, United States, November 2017. https://www.cdc.gov/flu/fluvaxview/nifs-estimates-nov2017.htm. Accessed March 17, 2017.
3. U.S. Centers for Disease Control and Prevention. Prevention and Control of Seasonal Influenza with Vaccines: Recommendations of the Advisory Committee on Immunization Practices — United States, 2017–18 Influenza Season.; 2017:1–20. https://www.cdc.gov/mmwr/volumes/66/rr/rr6602a1.htm. Accessed March 17, 2018.
4. U.S. Centers for Disease Control and Prevention. Update: Influenza Activity — United States, October 1, 2017–February 3, 2018.; 2018:169–179. https://www.cdc.gov/mmwr/volumes/67/wr/mm6706a1.htm?s_cid=mm6706a1_w. Accessed March 17, 2018.
5. Curry SJ. Organizational interventions to encourage guideline implementation. Chest. 2000;118(2 Suppl):40S-46S. 
6. Orleans CT. Increasing the demand for and use of effective smoking-cessation treatments reaping the full health benefits of tobacco-control science and policy gains–in our lifetime. Am J Prev Med. 2007;33(6 Suppl):S340–348. doi:10.1016/j.amepre.2007.09.003 
7. Arya, M., Kumar, D., Patel, S., Street, R.L., Giordano, T.P., Viswanath, K. Mitigating HIV Health Disparities: The Promise of Mobile Health for a Patient-Initiated Solution. Am J Public Health. 2014;104(12):2251–2255. doi:10.2105/AJPH.2014.302120 
8. Ashton CM, Haidet P, Paterniti DA, et al. Racial and ethnic disparities in the use of health services: bias, preferences, or poor communication? J Gen Intern Med. 2003;18(2):146–152. 
9. Fjeldsoe BS, Marshall AL, Miller YD. Behavior change interventions delivered by mobile telephone short-message service. Am J Prev Med. 2009;36(2):165–173. doi:10.1016/j.amepre.2008.09.040 
10. Chang BL, Bakken S, Brown SS, et al. Bridging the digital divide: reaching vulnerable populations. J Am Med Inform Assoc. 2004;11(6):448–457. doi:10.1197/jamia.M1535 
11. Hofstetter AM, Vargas CY, Camargo S, et al. Impacting delayed pediatric influenza vaccination: a randomized controlled trial of text message reminders. Am J Prev Med. 2015;48(4):392–401. doi:10.1016/j.amepre.2014.10.023 
12. Stockwell MS, Westhoff C, Kharbanda EO, et al. Influenza vaccine text message reminders for urban, low-income pregnant women: a randomized controlled trial. Am J Public Health. 2014;104 Suppl 1:e7–12. doi:10.2105/AJPH.2013.301620 
13. U.S. Department of Health and Human Services. Healthy People 2020 Topics and Objectives. http://www.healthypeople.gov/2020/topicsobjectives2020/default. Accessed March 17, 2018.
Posted on Dec 4, 2018 in Perspective Pieces |
Recharging Smiles: Strategies for Using Mobile Phones in Dental Public Health
Dr. Aditi Hegde1, Dr. Gopikrishna V2, Dr. Smitha B Kulkarni3, Dr. Nithin N Bhaskar3, Dr. Sourabha K Gangadharappa4, Dr. Jeswin Jacob4
1BDS, Postgraduate student, Department of Public Health Dentistry, Dayananda Sagar College of Dental Sciences; 2MDS, Professor and Head of the Department, Department of Public Health Dentistry, Dayananda Sagar College of Dental Sciences; 3MDS, Reader, Department of Public Health Dentistry, Dayananda Sagar College of Dental Sciences; 4MDS, Senior Lecturer, Department of Public Health Dentistry, Dayananda Sagar College of Dental Sciences
Corresponding Author: hegde.aditi.91@gmail.com
Journal MTM 7:2:60–65, 2018
doi:10.7309/jmtm.7.2.9
Abstract: Through the advent of smartphones, the previously elusive internet is now available to each person right in their hands, with lightning fast speeds available at rather nominal charges. Mobile phones offer numerous solutions to dentists and health workers alike and can be applied in a variety of ways in a public health setting. This paper discusses the application of mobile phones in primary, as well as secondary and tertiary levels of intervention from a dental public health perspective. Indeed, the described strategies can be employed by professionals, alone or combined with other interventions, to enhance the oral health of their patients.
Keywords: cell phones, dental public health, health promotion, oral health, prevention.
Introduction
The role of communication in the human health care sector is inescapable. It helps to convey the patient’s own experiences, values and preferences to the health care professional, all of which greatly influences a patient’s perception of the service, can create motivation for change, as well as augment subsequent compliance and adherence.1 This has led health care providers to constantly seek new, effective ways to reach “consumers” and promote their health through education, ultimately helping them manage their ailments. Overall, mobile phones have revolutionized the face of communication, and there is great potential for their use in health sectors. Patients and providers can now communicate from anywhere in order to follow-up on test results, ask questions, collect information, schedule appointments, send reminders and renew prescriptions.
Previously, text-messaging based health education campaigns have been used by administrations to control infectious diseases, to educate people regarding health policies, care of the pregnant and the elderly, and to dispel rumors.2 In scarcely resourced countries, mobile technologies can be used in a three-fold manner – to educate health workers, to establish a surveillance system, and to provide information to the general public.3
Dental Public Health has been defined as “the science and art of preventing and controlling dental diseases and promoting dental health through organized community efforts. It is that form of dental practice that serves the community as a patient rather than the individual. It is concerned with the dental health education of the public, with applied dental research, and with the administration of group dental care programs, as well as the prevention and control of dental diseases on a community basis.”4 In this new, complex world, dental public health is seen as a means to address the disparities in oral health outcomes that exist both within and between nations.5
In a country like India, where the dentist population ratio is so skewed in favor of urban areas, many remote villages and localities severely lack dental health services.6 The absence of private dentists can only be countered by providing adequate oral health services at a primary health center or community health center. Deprofessionalization of dentistry has been regarded as a necessary evolution to combat the burgeoning morbidity due to oral diseases in rural areas, a problem that is only magnified by the ever-increasing population.7 Developing a system to remotely educate and aid health extension workers will greatly improve the quality of oral health care. Where other conventional delivery mechanisms fall short, mHealth is already being used to provide underserved populations with access to information and services.
Mobile devices can easily be applied in a dental health setting to enhance patient outcomes.8 As practitioners of dental public health in a developing nation where there is both lack of oral health awareness and lack of services, the authors realized the need for alternative methods of oral health care delivery. It was observed that most patients possessed a mobile phone with internet capabilities, and were also interested in innovative technologies that could enhance their health. This inspired a search for mobile phone interventions in dental public health. A comprehensive knowledge of the purposes for which mobile phones have been used in healthcare in the past and an idea about their future utilization is necessary. Understanding the ‘Why?’, ‘What?’ and ‘How?’ of these interventions will enable public health workers to incorporate mHealth, an essential tool in this technology-oriented era, into dental public health practice.
Applying Mobile Phones In Dental Public Health
Researchers from all fields of science have attempted to incorporate the myriad features and technologies of mobile phones into health-care interventions. In the field of oral health, such interventions can be used in a variety of ways to enhance health outcomes. Dentists too are getting involved in this technological revolution. In a descriptive study by Jasti et el.,9 approximately 68% of the surveyed dentists from Khammam, Andhra Pradesh reported using healthcare apps on their smartphones for either personal knowledge or patient education purposes. In a Dental Public Health setting, mobile phones can be used for primordial, primary, secondary, as well as tertiary prevention.
In primordial prevention
One way to help patients is by giving them the information about how to avoid dental problems by means of text messaging or apps. A mass oral health education campaign can be carried out using text messages and multimedia messages (MMS) even before the appearance of risk factors in the population. For example, text messages discussing the importance of avoiding tobacco can be sent to all cell phone users, irrespective of their usage status. The reach of such a campaign will be massive because even in a developing country like India, there are approximately 74 mobile subscriptions per 100 people.10
An attempt can also be made to bolster the oral health of the community by taking advantage of the Digital India Initiative by the Government of India. ‘Kilkari’ is one such scheme for information regarding maternal and child health, where pregnant women receive voice calls on a range of relevant topics.11 Integrating oral health education into this scheme will not just expand the latitude of the existing programme, but will also allow access to a key target population.
In primary prevention
Using SMS and mobile phone applications, oral health education can be provided at an individual and community level. When selecting apps for oral health education, it is necessary to select one that dispenses accurate information based on evidence. Software developed for this purpose usually allows patients learn about their disease, its prevention and necessary treatment, however, requires active participation.
Smartphones can also utilize entertainment to dispense health education, such as Molarcropolis, a mobile persuasive to raise oral health and dental hygiene awareness for adolescents and young adults. Soler et al.12 evaluated the game and found that most of the participants found the game to be both entertaining and informative. Mobile social media platforms such as Facebook and Twitter can also be used to leverage social influence and bring attention to the importance of oral health.
Schluter et al.13 successfully utilized motivational text messaging to promote brushing among young adults receiving Work and Income support in New Zealand. By making use of the communication capabilities of mobile phones, a discernible improvement in oral hygiene was obtained. Researchers have also reported that sharing anonymous photographs (“selfies”) in a WhatsApp or other such chat-room leads to significant improvements in oral hygiene of participants.14,15
The Brush DJ app was developed to motivate patients to adopt an evidence-based oral hygiene behavior by playing music of the user’s choice. The app also reminds the user to spit and not rinse after brushing in order to maintain optimum local fluoride levels. Its competence was demonstrated by Underwood et al.16 who reported that 88% of app users were motivated to brush longer.
Dental caries is another common dental disease, closely associated with diet, as has been proven by innumerable researchers.17,18 Tracking a patient’s diet is a commonly used method for caries risk assessment and also for assessing one’s general health behavior in routine practice. Although unexplored, this pivotal step of diet history can be simplified by making use of journaling applications such as Wellness Diary, Calorific, My Food Diary, Nutritionist etc. This comprehensive overview of the patient’s diet history can be shared with the dentist who can then formulate an appropriate treatment plan.
To help patients quit harmful habits, public health dentists and primary care workers can provide habit counselling using mobile phones. An example of this is The Real E Quit Mobile smoking cessation application that helps people quit smoking with the aid of supportive audio clips and documents. Users can also make their own lists on reasons for quitting, benefits, and plans for challenging situations. Buller et al.19 found that 75% of users evaluated REQ-mobile to be user-friendly, and concluded that it was a feasible method for delivering cessation support to help people quit smoking.
In secondary prevention
Oral cancer screening is based on the rationale that self-examination or oral check-up by a professional reduces the mortality due to this disease, and also leads to recognition in earlier stages. Birur et al.20 describe the use of Oncogrid, a mobile phone based remote oral cancer surveillance tool, connecting primary care dental professionals with frontline health workers (FHW). This telemedicine program found that oral cancer screening and surveillance via mobile phones was feasible even in remote areas and low-resource settings. The authors suggest that such interventions can cause a paradigm shift in the practice of public health.
MySmileBuddy was developed by Levine et al.21 to reduce early childhood caries prevalence and its consequences amongst a high risk population. It allows community health workers or lay workers to conduct preliminary dietary screening assessment for high risk children and their mothers. After collecting information on the caries risk, the parents are informed of suitable behavior goals they can choose from so that the caries risk is diminished. The associated community health worker also follows up on the family to assess the progress towards behavior goals. With further research and adaptation, the use of mobile technology for dietary assessment may be applicable for widespread use in a variety of sites and programs that address the health needs of young children. The highly-advanced cameras available in current mobile phones also allow for remote screening for dental caries by mid-level dental providers, as demonstrated by Estai et al.22 They found that this method has a sensitivity ranging from 60-68%, and a specificity between 97-98%. This can help tackle some of the problems caused by the lack of dental services available to rural populations in countries like India.
Another problem created by inequitable distribution is the unavailability of emergency dental treatment. Oral and maxillofacial surgery (OMFS) is a particularly challenging field as it requires impeccable knowledge of both medicine and dentistry.23 There is potential for gaps in clinical knowledge when an untrained health worker has to manage acute OMFS cases. Mobile devices can be a means to access electronic educational resources during clinical activities and also improve clinical decision-making.24
Additionally, it is now possible to advise even those who are furthest from dental treatment during an emergency. Stein et al.25 developed an extremely useful application for the purpose of triaging dental emergency. Their study demonstrated that patients can use their smartphones to transmit relevant clinical data to their dentists, all within 4 minutes. The authors suggested using mobile applications to enhance routine and emergency dental care.
In Tertiary Prevention
In primary and community health centers, dentists are often posted on a rotational basis due to the paucity of professionals. Therefore, a dentist may not always be available for post-surgery consultation. In the case of full-mouth rehabilitation cases, it takes quite some time for patients to get used to their new appearance and occlusion. To help patients rehabilitate, dental professionals and health workers can consult and counsel via mobile phones. For instance, myDentist is an app through which patients may explain their problems to the oral health care provider by sending text, diagrams or photos. The dentist can respond to these messages with appropriate instructions to manage the problem, and can also arrange an appointment for the future.
Dental phobia is a crippling disorder causing an individual to avoid dental treatment because of an irrational fear, even if they are in pain. In the process of avoiding the dentist, the disease progresses and may lead to severe disability. To limit this disability caused by dental diseases, elimination of dental phobia is necessary, after which patients can utilize the services available to them. Applications like Dental Phobia claim to reduce a patient’s anxiety towards dental treatment through hypnosis. Such means of handling dental phobia must be critically reviewed before wider application; research must be conducted in this field in the future.
Shortcomings of Mobile Phone Health Care Interventions
One of the primary restraints of mHealth is that not all interventions can be readily applied to the myriad segments of the population. It must be kept in mind that the ability to read the information may be lacking in many mobile phone users due to low literacy rates; approximately 15% of the adult population was considered to be illiterate in 2010. Moreover, as per World Bank estimates, at least thirteen developing nations have a literacy rate of less than 50%.26 In such conditions, a text-based intervention may fail, while image-based interventions can succeed. Complicated and cumbersome technology may hinder, rather than assist the user, especially if the procedure involves too many steps.
Another limitation is that the cost-effectiveness of internet-based mobile phone interventions has not been established. Depending on the network carrier and data usage, charges can vary from user to user. One more feature that varies with network carrier is the range. Although there has been staggering growth, there are certain areas that are still untouched by this technology.

Table 1: Mobile phone interventions in Dental Public Health
Additionally, Tatum et al.27 have proposed that cortical processing in the human brain is uniquely activated by the use of personal electronic devices such as mobile phones. However, the practical and real-world implications are yet to be studied.
Finally, it is worth mentioning that there is a paucity of comparative studies regarding mobile phone interventions in dentistry. Therefore, it is not possible at this time to conclude on the relative value of each intervention. It is necessary to conduct rigorous investigation to assess the same.
Conclusion
Like fire and the wheel, the invention of mobile phones changed the lives of humans worldwide, and like most inventions, they are in a process of constant improvement. Healthcare professionals have recognized the impact this has had on the lives of their patients, and have adopted cellphones in a variety of ways. Oral health care providers can implement mHealth interventions in public health practice at all levels of prevention. Indeed, one, or a combination of these strategies can be employed by health workers to enhance the oral health of their patients. Moreover, mobile phones are an accessible, affordable, appropriate technology for interventions in a public health setting.
By focusing on prevention and involving the community in these programs, dental professionals can give a much-needed boost to the oral health status of people. There are unparalleled advantages to using mobile devices that cannot be matched by other technological media. However, the potential complications should be kept in mind. Dentists should take initiative and be involved in the planning of guidelines for these interventions.
Sources of support
Nil
Acknowledgements
Nil
Declaration: The matter presented in this paper or any part of it is has not been submitted elsewhere simultaneously. The authors certify that they have no potential conflict of interest, financial or otherwise, pertaining to the information discussed in this paper. All the matter presented in this paper has been read and approved by all the authors.
Criteria for inclusion in author’s list: Dr. Aditi Hegde was involved in the conception, literature review, compilation and writing of the paper. Dr. Gopikrishna V took part in the conception of the study and writing of the paper. Dr. Smitha B Kulkarni took part in writing the paper. Dr. Nithin N Bhaskar supervised the literature review, and took part in the writing of the paper. Dr. Sourabha K G participated in literature review and paper writing. Dr. Jeswin Jacob participated in the study conception and writing of the paper. All authors have provided valuable inputs to the manuscript, agree with its contents, and have approved the final manuscript.
References
The literature search was performed using an electronic database search of peer-reviewed bibliographic and non-bibliographic databases, as well as a review of websites of reliable institutions. Medical Subject Headings (MeSH terms) were used wherever possible to ensure a uniform search strategy. Each term was used as a single item or in combination by employing the Boolean operators “AND” and “OR”. The following terms were used: teledentistry, mHealth, mobile phone, mobile health, cell phone, texting, message, text message, mobile application, SMS, dentistry, dental health, dental public health, public health dentistry, oral health.
The studies that were not directed towards oral or dental health were excluded. All included studies focused on the prevention and control of oral diseases, collection and transmission of oral disease information, and training of health workers.
1. Ang WC, Swain N, Gale C. Evaluating communication in healthcare: Systematic review and analysis of suitable communication scales. J Commun Healthc 2013;6(4):216–22. 
2. Ni Z, Wu B, Samples C, et al. Mobile Technology for Health Care in Rural China. Int J Nurs Sci 2014;1(3):323–4. 
3. Deribe K, Roda AA. The potential of mobile phone technology for public health practice in Ethiopia. Ethiop J Health Dev 2012;25(3):233–4.
4. Beltran E. The American Board of Dental Public Health Informational Brochure [Internet]. American Association of Public Health Dentistry; 2015 [cited 1 August 2017]. Available from: http://www.aaphd.org/assets/ABDPH/abdph-informational-brochure-2016-fin.pdf
5. Petersen PE. The World Oral Health Report 2003: continuous improvement of oral health in the 21st century–the approach of the WHO Global Oral Health Programme. Community Dent Oral Epidemiol 2003;31(S1):3–24. 
6. Yadav S, Rawal G. The current status of dental graduates in India. Pan Afr Med J 2016;23:22. doi:10.11604/pamj.2016.23.22.7381. 
7. Reddy KV, Moon NJ, Reddy KE, et al. Time to implement national oral health policy in India. Indian J Public Health 2014;58:267–9. 
8. Mustaza TA, Lim TW, Ghani A, et al. Mobile applications at the dentist. International Journal on E-Learning and Higher Education 2016;4:16–28.
9. Jasti D, Pratap KVNR, Padma MT, et al. Health care apps- will they be a facelift for today’s medical/dental practice? J Mob Technol Med 2015;4(1):8–14. 
10. Telecom Regulatory Authority of India. Highlights of Telecom Subscription Data as on 30th June, 2015. Press Release no. 47/2015. New Delhi: Telecom Regulatory Authority of India; 2015.
11. Ministry of Health and Family Welfare. Kilkari Messages – Mother and Child Tracking: Govt. Of India [Internet]. Nrhm-mcts.nic.in. 2016 [cited 17 December 2016]. Available from: http://nrhm-mcts.nic.in/KKMSG.aspx
12. Soler C, Zacarías A, Lucero A. Molarcropolis: a mobile persuasive game to raise oral health and dental hygiene awareness. International Conference on Advances in Computer Entertainment Technology. New York: The Association for Computing Machinery; 2009. p. 388–91. 
13. Schluter P, Lee M, Hamilton G, et al. Keep on brushing: a longitudinal study of motivational text messaging in young adults aged 18–24 years receiving Work and Income Support. J Public Health Dent 2015;75:118–25. 
14. Zotti F, Dalessandri D, Salgarello S, et al. Usefulness of an app in improving oral hygiene compliance in adolescent orthodontic patients. Angle Orthod 2015;86(1):101–7. 
15. Li X, Xu ZR, Tang N, et al. Effect of intervention using a messaging app on compliance and duration of treatment in orthodontic patients. Clin Oral Investig 2016;20(8):1849–59. 
16. Underwood B, Birdsall J, Kay E. The use of a mobile app to motivate evidence-based oral hygiene behaviour. Br Dent J 2015;219(4):E2. doi: 10.1038/sj.bdj.2015.660. 
17. Nikiforuk G. Understanding Dental Caries. Vol. 1: Etiology and Mechanisms. Basel: Karger; 1985.
18. Hujoel PP, Lingström P. Nutrition, dental caries and periodontal disease: a narrative review. J Clin Periodontol 2017;44(S18):S79–S84. 
19. Buller DB, Borland R, Bettinghaus EP, et al. Randomized trial of a smartphone mobile application compared to text messaging to support smoking cessation. Telemed J E-Health 2014;20(3):206–14. 
20. Birur PN, Sunny SP, Jena S, et al. Mobile health application for remote oral cancer surveillance. J Am Dent Assoc 2015;146(12):886–94. 
21. Levine J, Wolf R, Chin C, et al. MySmileBuddy: An iPad-based interactive program to assess dietary risk for early childhood caries. J Acad Nutr Diet 2012;112(10):1539–42. 
22. Estai M, Kanagasingam Y, Huang B, et al. The efficacy of remote screening for dental caries by mid-level dental providers using a mobile teledentistry model. Community Dent Oral Epidemiol 2016;44(5):435–41. 
23. Aziz SR, Ziccardi VB. Telemedicine Using Smartphones for Oral and Maxillofacial Surgery Consultation, Communication, and Treatment Planning. J Oral Maxillofac Surg 2009;67:2505–9. 
24. Payne KF, Goodson AM, Ahmed N, et al. Developing a smartphone application to improve access to quick-reference educational resources: the oral and maxillofacial surgery experience. Bulletin of the Royal College of Surgeons of England 2013;95(2):62–79. 
25. Stein CD, Xiao X, Levine S, et al. A prototype mobile application for triaging dental emergencies J Am Dent Assoc 2016;147(10):782–791.e1. doi: 10.1016/j.adaj.2016.03.021. 
26. World Bank. Literacy rate, adult total (% of people ages 15 and above) | Data [Internet]. Data.worldbank.org. [cited 1 August 2017]. Available from: http://data.worldbank.org/indicator/SE.ADT.LITR.ZS?year_high_desc=false
27. Tatum WO, Di Ciaccio B, Yelvington KH. Cortical processing during smartphone text messaging. Epilepsy Behav 2016;59:117–21. 
Posted on Dec 4, 2018 in Letter to the Editor |
Computer Literacy in the Elderly: A Survey Examining Real World Usability of Medical Software
Rasiah, S
Whitchurch, M
Journal MTM 7:2:66–67, 2018
doi:10.7309/jmtm.7.2.10
There is widespread evidence of an association between reduced health literacy and an increased risk of poor medical outcome. Patients with poor medical education experience significantly higher emergency room costs1 and up to double the hospital admission rates compared to patients with sufficient medical education.2–6 Lack of medical literacy is particularly important in the ageing population, due to increased burden of chronic illness and the increasingly complex management of progressive chronic conditions. To address this, various smartphone and tablet medical applications have been developed to improve patient health literacy and monitor chronic illnesses. We propose the need to examine the technological literacy of elderly patients, who are most likely to benefit from these applications.
The efficacy of self-monitoring medical applications hinges on a patient’s ability to access and use technology to track health progress. We suspect that computer literacy in elderly patients will not be adequate for effective technological monitoring of chronic illness at this time. It has been shown that amongst doctors there is often low familiarity with basic computer applications.7
We have designed a study to determine the technological literacy of patients who present to a large specialist Ophthalmology hospital. This population is one of the least likely to adequately operate advanced technology due to deteriorating vision and advanced age. There has also been recent development of patient health-monitoring applications for illnesses in this field. These include applications to monitor glaucoma and macular degeneration, which have significant correlation with clinical assessment in experimental settings.8,9
We will survey Ophthalmology patients and compare their ability to perform simple tasks on their smartphones and tablets as a screening measure for operating more advanced medical software for the purposes of health monitoring. The designed survey will enquire about the ability of patients to install, open and operate applications on a smartphone or tablet. The survey will also obtain information about the type of devices patients own and frequently use. Finally, the survey asks whether a patient has any previous experience with medical applications.
With the results of this research we aim to assess the computer literacy of an ageing patient population, and extrapolate from this data the reliability of personal medical software to accurately monitor chronic disease in this demographic. Due to potential limitations in patient language comprehension, participants will be limited to those fluent in English. While there are also potential study limitations due to visual or technological difficulties, these problems will reflect the issues in implementing personal medical applications in practice.
These findings will act as a benchmark to guide the feasibility of implementation of technology-based disease monitoring in the near future. We would expect, with time, that subsequent generations’ computer literacy will only improve from this benchmark.
References
1. Howard DH, Gazmararian J, Parker RM. The impact of low health literacy on the medical costs of Medicare managed care enrollees. The American journal of medicine [Internet]. 2005;118(4):371–7. Available from: http://www.ncbi.nlm.nih.gov/pubmed/15808134 
2. Baker DW, Parker RM, Williams M V., Clark WS. Health literacy and the risk of hospital admission. Journal of General Internal Medicine. 1998;13(12):791–8. 
3. Levin-Zamir D, Peterburg Y. Health literacy in health systems: Perspectives on patient self-management in Israel. Vol. 16, Health Promotion International. 2001. p. 87–94. 
4. Dewalt DA, Berkman ND, Sheridan S, Lohr KN, Pignone MP. Literacy and health outcomes: a systematic review of the literature. Journal of general internal medicine. United States; 2004 Dec;19(12):1228–39.
5. Williams M V, Baker DW, Parker RM, Nurss JR. Relationship of functional health literacy to patients’ knowledge of their chronic disease. A study of patients with hypertension and diabetes. Archives of internal medicine. United States; 1998 Jan;158(2):166–72.
6. Schillinger D, Grumbach K, Piette J, Wang F, Osmond D, Daher C, et al. Association of health literacy with diabetes outcomes. JAMA. United States; 2002 Jul;288(4):475–82.
7. Debehnke DJ, Valley VT. Assessment of the current computer literacy and future computer needs of emergency medicine residents and faculty. American Journal of Emergency Medicine. 1993;11(4):371–3. 
8. Anderson A, Bedggood A, Kong Y, Martin K, Vingrys A. Can Home Monitoring Allow Earlier Detection of Rapid Visual Field Progression in Glaucoma? American Academy of Ophthalmology. 2017;124(12):1735–42. 
9. Winther C, Frisen L. Self-Testing of Vision in Age-Related Macula Degeneration: A Longitudinal Pilot Study Using a Smartphone-Based Rarebit Test. Journal of Opthalmology. 2015;2015:285463. 
Posted on Dec 4, 2018 in Featured |

The Editorial Board at the Journal of Mobile Technology in Medicine is proud to present Volume 7, Issue 2. Mobile technology in Medicine is a rapidly developing area, and we hope to continue accelerating research in the field. We look forward to your submissions for Issue 2.
Posted on May 1, 2018 in News |
WITHOUT SOURCES
Feburary 2018 saw the release of the exciting research paper ‘Prediction of cardiovascular risk factor from retinal fundus photographs via deep learning’ in Nature Biomedical Engineering. The Google Team had developed a new artificial intelligence technology using deep convolutional neural networks to assess both individual cardiovascular risk factors and the risk of a cardiac event through retinal fundus imaging.
The algorithm assesses individual risk factors (including smoking, blood pressure) by generating a heat map so the algorithm assesses the anatomical regions most relevant to the particular cardiovascular risk factor. It is particularly impressive that many of the risk factors which the algorithm predicted were risk factors previous not believed to be present in retinal images, including age, gender, smoking status and systolic blood pressure. Alongside assessing individual risk factors the team also developed a model to predict major adverse cardiovascular event onset within 5 years.
Current means of cardiovascular disease risk calculation include the Framingham CVD Risk Prediction Score, Pooled Cohort Equations, and Systematic Coronary Risk Evaluation. There are continued efforts to improve the quality of the risk prediction calculators, as there are limitations associated with some of them. For example the Framingham CVD Risk Prediction Score, which is the most commonly used risk estimation system worldwide, has been found to overestimate risk for women and has been less effective in predicting risk for elderly people.
This development has exciting implications in improving identification of individuals at risk for cardiovascular disease. Cardiovascular disease poses a significant global burden as the leading global cause of death. In 2015 Cardiovascular disease represented 31% of all global deaths of which three quarters occurred in low and middle income countries.
The algorithm not only has the ability to improve outcomes of patients at risk for developing cardiovascular disease through early identification, but also other diseases as the individual risk factors identified (including blood pressure, age, smoking, gender, race) can potentially be used to calculate risk for other diseases such as Chronic Kidney Disease and Diabetes.
WITH SOURCES
Feburary 2018 saw the release of the exciting research paper ‘Prediction of cardiovascular risk factor from retinal fundus photographs via deep learning’ in Nature Biomedical Engineering. The Google Team had developed a new artificial intelligence technology using deep convolutional neural networks to assess both individual cardiovascular risk factors and the risk of a cardiac event through retinal fundus imaging.
The algorithm assesses individual risk factors (including smoking, blood pressure) by generating a heat map so the algorithm assesses the anatomical regions most relevant to the particular cardiovascular risk factor. It is particularly impressive that many of the risk factors which the algorithm predicted were risk factors previous not believed to be present in retinal images, including age, gender, smoking status and systolic blood pressure. Alongside assessing individual risk factors the team also developed a model to predict major adverse cardiovascular event onset within 5 years.
(1).
Current means of cardiovascular disease risk calculation include the Framingham CVD Risk Prediction Score, Pooled Cohort Equations, and Systematic Coronary Risk Evaluation. There are continued efforts to improve the quality of the risk prediction calculators, as there are limitations associated with some of them. For example the Framingham CVD Risk Prediction Score, which is the most commonly used risk estimation system worldwide, has been found to overestimate risk for women(2) and has been less effective in predicting risk for elderly people (3).
This development has exciting implications in improving identification of individuals at risk for cardiovascular disease. Cardiovascular disease poses a significant global burden as the leading global cause of death. In 2015 Cardiovascular disease represented 31% of all global deaths of which three quarters occurred in low and middle income countries (4).
The algorithm not only has the ability to improve outcomes of patients at risk for developing cardiovascular disease through early identification, but also other diseases as the individual risk factors identified (including blood pressure, age, smoking, gender, race) can potentially be used to calculate risk for other diseases such as Chronic Kidney Disease and Diabetes.
Sources
1. Prediction of cardiovascular risk factors form retinal fundus photographs via deep learning. Nature biomedical engineering. https://www.nature.com/articles/s41551-018-0195-0
2. Validation of the Framingham general cardiovascular risk score in a multiethnic Asian population: Retrospective cohort study http://bmjopen.bmj.com/content/5/5/e007324?utm_source=trendmd&utm_medium=cpc&utm_campaign=bmjopen&trendmd-shared=1&utm_content=Journalcontent&utm_term=TrendMDPhase4
3. Value and limitations of existing scores for the Assessment of Cardiovascular Risk: A Review for Clinicians. Journal of the American College of Cardiology. https://www.sciencedirect.com/science/article/pii/S0735109709025029
4. WHO Cardiovascular Diseases Fact Sheet May 2017 http://www.who.int/mediacentre/factsheets/fs317/en/
![]()
![]()
![]()
![]()
![]()
![]()














