Theory Driven Mobile-Based Interventions: A Scoping Review
Theory Driven Mobile-Based Interventions: A Scoping Review
Jenna Brager, PhDc, BSN-RN, MS1, Melissa Pinto, PhD2, RN, FAAN, Adam Kaplin, MD, PhD3
1Johns Hopkins University, School of Nursing, Baltimore, MD, USA
2Emory University, Nell Hodgson Woodruff School of Nursing and Rollins School of Public Health
3Johns Hopkins University, School of Medicine, Baltimore, MD, USA
Corresponding Author: Melissa.d.pinto@emory.edu
Journal MTM 6:3:48–65, 2017
Background: Mobile technology is a rapidly evolving field allowing healthcare providers to reach patients outside of a traditional face-to-face setting. Fortunately, interventions are now becoming readily available via mobile devices such as mobile phones, smart phones, and tablets, yet there has been little attention to the design of these interventions so that they are theoretically-driven (informed according to a behavioral theory or model) and ethically performed.
Objective: To provide data on theoretically-driven interventions that were empirically tested and to analyze the features and strategies used to implement these interventions.
Review Methods: This study employed a scoping review methodology according to the Joann Briggs Institute. An electronic database search yielded 20 eligible articles.
Results: The participants spanned various health domains: cardiovascular (weight control, physical activity, diabetes), cancer (pap testing), prenatal care, substance use (alcohol recovery, smoking cessation), and HIV and/or sexual risk assessment. Social Cognitive Theory, Health Belief Model, and Transtheoretical Model were applied most frequently to guide interventions.
Conclusion: Future work should focus on the application of theory and how various implementation techniques translate to the overall effectiveness of the intervention.
Keywords: mobile technology; theory; model; mhealth; mobile application; text-messaging
Theory Driven Mobile-Based Interventions: A Scoping Review
Within the last decade, there has been tremendous outgrowth of mobile technology, especially the use of tablets, smartphones, and mobile phones. The increasing use of technology presents healthcare providers with an unprecedented opportunity to support and deliver care to patients outside of the acute care setting 1. Owing to an increase in chronic health conditions, it is critical for patients to have real-time and mobile access to evidence-based health information and self-management interventions. Nearly 50% of Americans have at least one chronic disease that requires daily self-management to optimize outcomes, and the largest degree of self-management behavior occurs outside the acute care setting2. Self-management interventions that are available through mobile devices are a promising area of science for disease prevention and wellness promotion3.
Mobile technologies have extended the physical boundaries of care beyond the traditional healthcare setting through the incorporation of real-time data capture, exchange and personalization of the interventions4. Mobile interventions can be used to target key self-management behaviors like medication adherence, adversities, and barriers, which importantly reinforces the patient’s role as an active agent in management of their health5. Additionally, these interventions can be designed based on evidence-based principles shown to promote health by connecting individuals to receive social support via discussion forums and personalizing interventions to one’s individual needs through the use of tailored text messages6–9. Importantly, at a time where the cost of chronic disease is rising, mobile technologies may provide a cost-effective opportunity capable of reaching larger target populations spanning diverse health domains8,10,11.
Nearly 90% of American adults own a cell phone, and of these individuals, 64% own a smartphone 12. Since 2011, there has been a 30% increase in ownership of smartphones with nearly 62% of smartphone owners report using their cellphone to seek health information within the past year13. In 2015, there were 500 million smartphone users downloading mobile health applications14. While increased access to health information and tools for self-management are desired, the majority of these apps have not undergone rigorous trials for efficacy14. There has been little attention to the design of these interventions so that they are theoretically-driven (informed and guided by behavioral theories and/or models) and ethically perform (yield the benefit that is as they are advertised) to the level as expected by patients15.
In order for patients to have sustainable changes, consistent engagement with mobile applications over time is necessary 16. Prior research suggests the necessity of theory-driven mobile-based interventions for long-term adherence to health behavior change17,18. Mobile interventions based on theory, “ensures that the intentions and drivers in the development of the intervention are clear and replicable”18, p. 7. By building an evidence base that combines the advancements of mobile health with theory, researchers will be more equipped to understand how individuals use and benefit from these interventions9. As mobile technologies are expected to increase in scope and impact, ongoing analyses of evidence are needed to inform the development of future mobile-based interventions. To our knowledge, we know of no other review that primarily focused on theoretically-driven mobile-based interventions to promote behavior change, consistent with self-management. Therefore, the purpose of this study was to provide data on theoretically driven interventions that were empirically tested and to analyze the features and strategies used to implement these interventions.
Purpose
The study proposed to answer the following questions: (a) What theories and/or models are currently guiding mobile-based interventions? (b) What are the most common features and strategies incorporated for intervention delivery? (c) What outcomes are measured to determine effectiveness and engagement with mobile-based interventions? (d) What are the gaps in the literature on theory driven mobile-based interventions? This study employed a scoping review methodology according to the Joanna Briggs Institute (JBI) Guidelines to present the literature that has been conducted on theory-driven mobile-based interventions across diverse health domains.
Method
Scoping Review
The approach for analysis of evidence is dependent upon the state of the science 19. Systematic reviews are informative when there is larger existing body of well-developed evidence that encourages a narrowed view of the problem from a smaller lens to draw conclusions on a specific research question, for a specific condition, and in a specific population19. On the other hand, scoping reviews are used to “provide a broad overview of a topic to identify gaps in the evidence, clarify key concepts, and report types of evidence that address and inform practice in a topic area” (19, p.7). Important distinctions between systematic reviews and scoping reviews center on the development of research questions, types of evidence, study selection, and presentation of the data. A scoping review is used to understand an emerging area of scientific inquiry, where a broad view of evidence in a domain is needed19. Restrictive inclusion criteria, as present in a systematic review, would limit our ability to comprehensively understand the problem. Because this is an emerging area of science, a broader scope is needed; a scoping review provides flexibility to extract data from all sources of evidence and research methodology, rather than applying the limitations of a systematic review and focusing solely on quantitative studies (or only one study design)19. Scoping reviews are also used as hypothesis-generating technique to help develop future systematic reviews that focus on hypothesis-testing20. This scoping review was conducted in accordance with the Joanna Briggs Institute (2015) guidelines, and included the following steps: (1) Identifying the research question, (2) Identifying relevant studies, (3) Study selection, (4) Charting the data, and (5) Collating, summarizing, and reporting the results19.
Identification of Relevant Studies
This scoping review was completed on April 3, 2015. A search inquiry across four electronic databases (PubMED, PsychINFO, EMBASE, and CINAHL) was developed with the assistance of a health sciences librarian and implemented using the following terms: (“Psychological Theory”[Mesh] OR “Nursing Theory”[Mesh] OR “Models, Theoretical”[Mesh] OR theory [tiab] OR theoretical [tiab] OR model* [tiab]) AND (“Cell Phones”[Mesh] OR “cell phone” OR “cell phones” OR “cellular phone” OR “cellular phones” OR “cellular telephone” OR “cellular telephones” OR “smart phone” OR “smart phones” OR “mobile phone” OR “mobile phones”). The search terms were used in combination whenever appropriate and selected in order to acquire relevant literature available in this domain.
Study Selection
The initial query was conducted by the first and third authors. The inquiry was limited to humans, the years of publication from 2009 to 2015, and the English language, which resulted in 1,940 articles. Of these articles, 411 were duplicates and removed. As a result, 1,529 abstracts were screened for eligibility. A hand search was performed as an added measure to improve the likelihood of capturing relevant articles. The inclusion and exclusion criteria were selected to generate articles capturing the essence of our study purpose by identifying clear behavior change theories currently guiding mobile-based interventions.
The following inclusion criteria were applied: (1) interventions said by the study author to be theoretically-driven; (2) web-based and/or mobile-based intervention focused on physical/behavioral outcomes (i.e. weight loss, physical activity, blood glucose/HbA1c monitoring, tracking alcohol consumption) and/or psychological outcomes (i.e. self-efficacy/confidence, motivation, attitude, support); (3) included analysis of the results of the intervention (rationale: to understand effectiveness); and (4) reported empirical data pertaining to engagement (i.e. satisfaction, acceptability, adherence, and/or feasibility; rationale: to understand usability and delivery) of the intervention. Exclusion criteria were: (1) no description of the underlying theory or model guiding the design of the intervention (rationale: interventions based on theory ensures that the intentions and drivers in the development of the intervention are clear); (2) web-based and/or mobile-based intervention were not the sole focus and combined with other interventions (rationale: it is difficult to determine the relative contribution of these interventions when they are packaged with other interventions); (3) report of secondary, not primary data (rationale: an advantage of including studies that reported primary data is that researchers are collecting information specific to their study purpose), and (4) review articles (systematic and literature).
The application of our inclusion and exclusion criteria to abstracts yielded 338 articles eligible for text review. Of these 338 articles, 319 were excluded because of: vague application of theory and/or model (237 articles), reporting of secondary data (32 articles), lack of usage metric data (35 articles), and/or the article was a protocol or review (15 articles). Nineteen articles remained. Lastly, the reference lists of systematic reviews identified during this process were hand searched for relevant articles which yielded one additional article. A total of 20 eligible articles were included in this review (Figure 1).
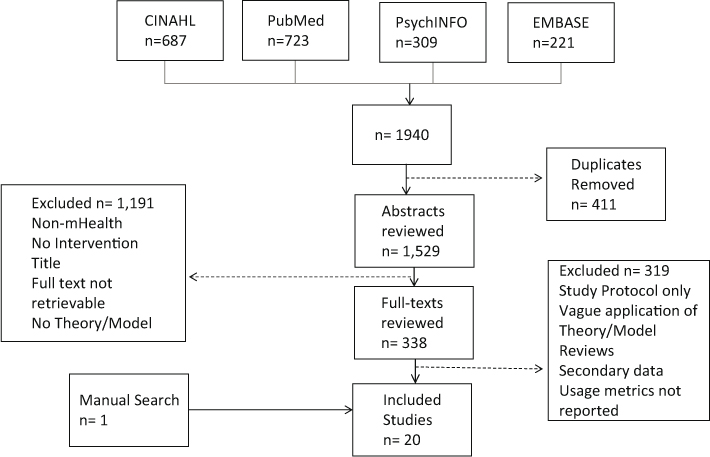
Figure 1: Flow Diagram
Charting and Collating the Data
Author, publication year, title, methods (design, theory and/or model of behavior change, intervention, and measures), study characteristics, and results were extracted from each article.
Results
A total of 20 articles were included. Although all articles focused on behavior change theories/models, the studies were heterogeneous with regard to how theories/models were employed, study designs, settings, health domains, intervention strategies, and outcome variables.
Theoretical Framework
As described in Table 1, Social Cognitive Theory (SCT) was the most commonly used theory across all types of interventions (n=8). SCT was applied across the health domains of diabetes management, smoking cessation, physical activity, and weight loss1,6,9,10,18,21–23. The Health Belief Model guided four (n=4) studies across three health domains, diabetes management, prenatal care, and sexual risk reduction9,11,22,24. The Transtheoretical Model also guided four interventions (n=4) and was most often guided interventions for weight loss and diabetes self-management6,25–27. Self Determination Theory guided two (n=2) interventions in studies focused on weight loss and alcohol relapse prevention21,28. Fog’s Behavioral Model guided two (n=2) interventions focused on preventing gestational weight gain and cervical cancer screening29,30. Theory of Planned Behavior also guided two (n=2) interventions focused on weight loss and diabetes management7,17. Sexual Script Theory, Behavioral Determinants Model, Common Sense Model, Self-Regulation Theory, Integrative Model of Behavior Intervention, and the Information Motivation Behavior Model were applied least frequently and focused on studies related to weight loss, HIV risk behavior, sexual risk reduction, and prevention of gestational weight gain1,8,22,29,31,32.
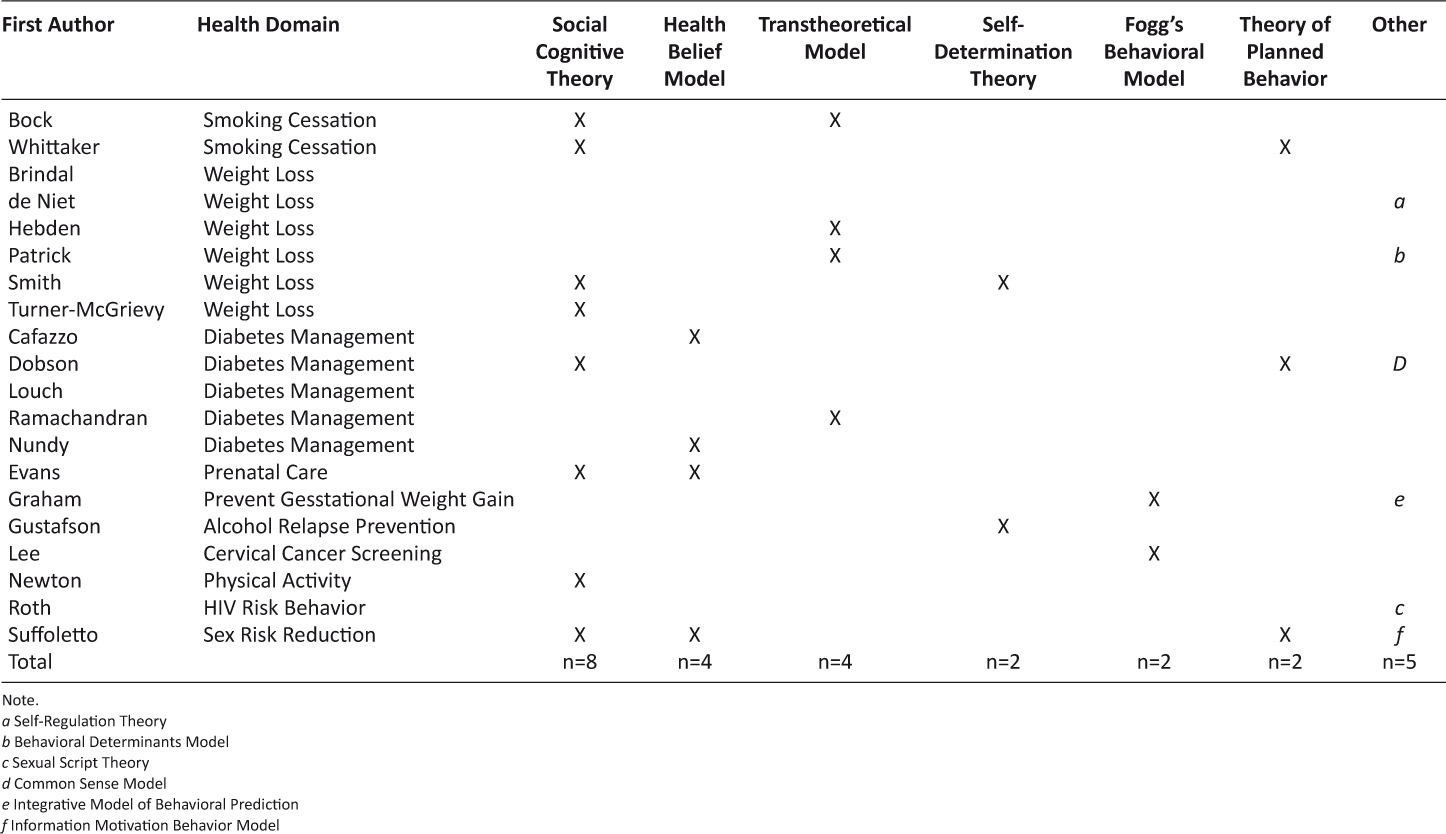
Table 1: Theoretical Framework
Theoretical Constructs
As described in Table 2, the theories and/or models were expanded upon by investigators to identify specific constructs of the theoretical frameworks that supported the development and implementation of the intervention. Of the 12 theoretical frameworks, 11 constructs were identified. Motivation (n=6) and self-efficacy (n=6) guided the majority of interventions, followed by self-control (n=3), cues to action (n=3), perceived severity/susceptibility – risk (n=2), intention (n=2), competence (n=2), knowledge/belief (n=2), barriers (n=1), self-worth/self-esteem (n=1), and self-perception of illness (n=1).
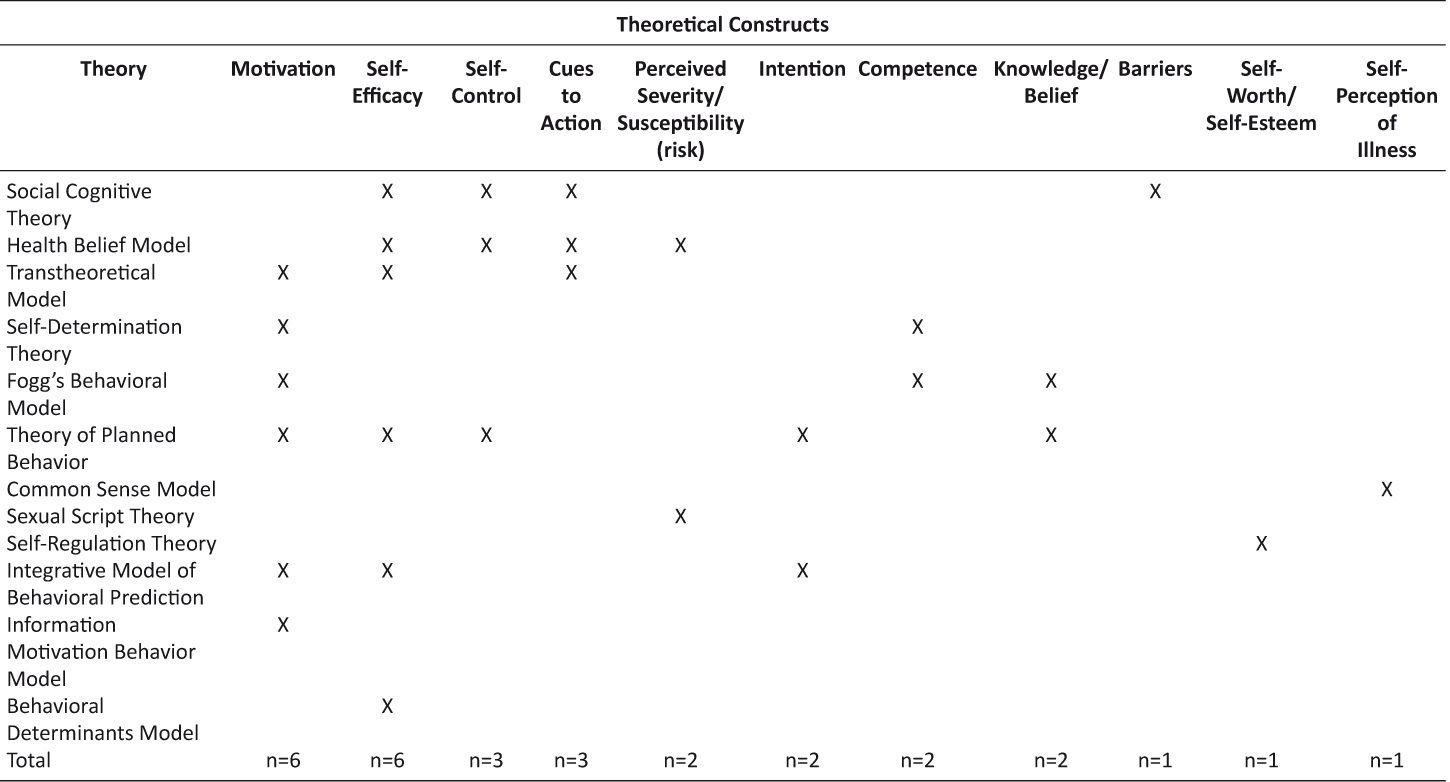
Table 2: Exploration of Theoretical Constructs
Settings and Sample
As described in Table 3, over half of studies were set in the United States6,9–11,22,23,28–32. Outside of the US, study locations included Australia (n=3)7,21,25, New Zealand (n=2)1,18, Netherlands, Canada, United Kingdom, and India8,17,24,27. Sample size and gender also varied greatly. Sample sizes ranged from as low as 2024 to 1,689 participants29. Six studies were targeted only for women7,9,22,29,30,32, whereas only one study focused solely on male participants27.
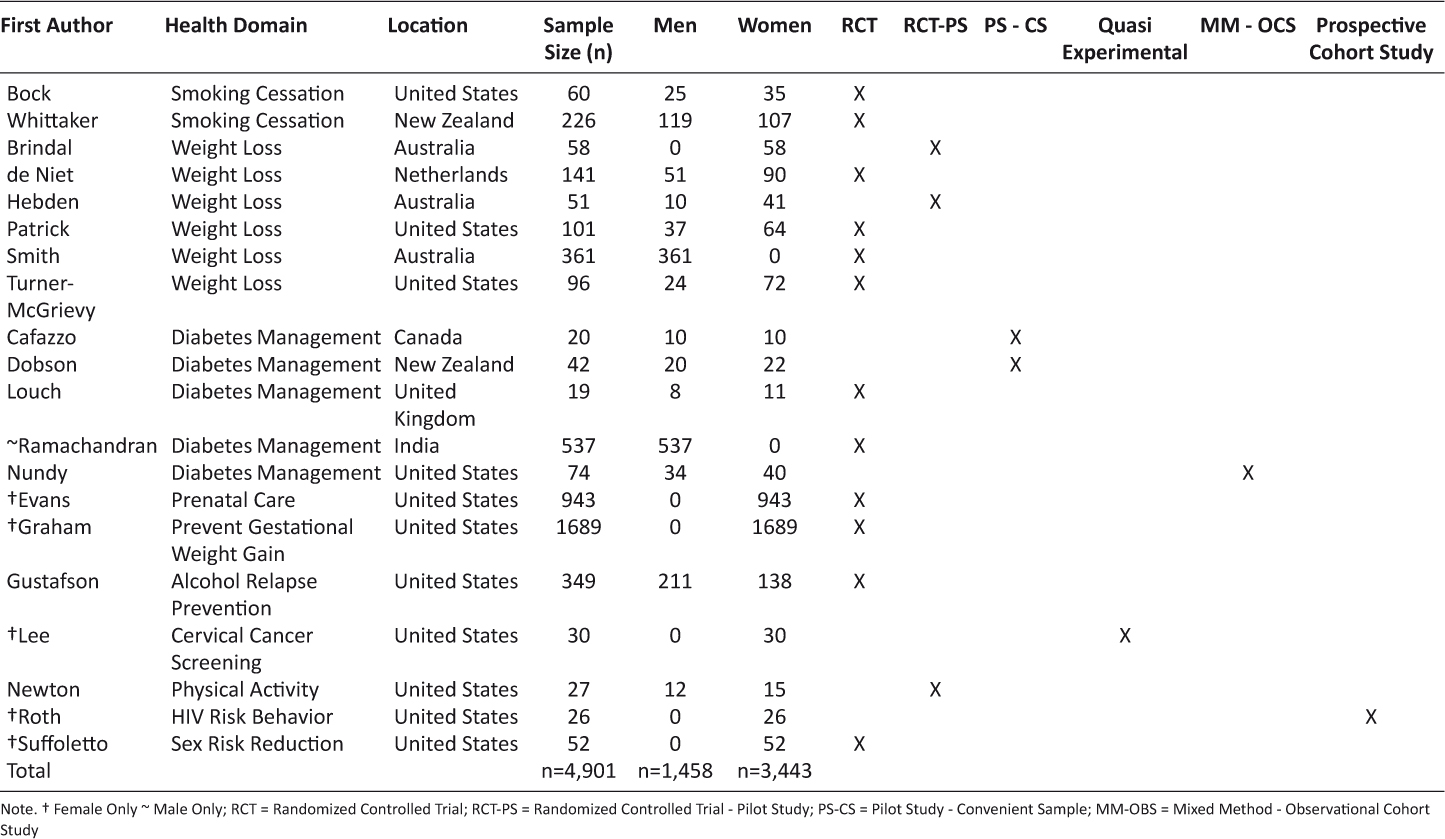
Table 3: Research Setting, Sample Size, and Design
Study Design
Also described in Table 3, the majority of the studies were randomized trials (n=12)6,8,9,17,18,21–23,27–29,31; followed by randomized controlled pilot studies (n=3)7,10,25; convenience sample pilot studies (n=2)1,24; quasi experimental (n=1)30; mixed method observation cohort study (n=1)11; and prospective cohort study (n=1)32.
Behavior Change Strategies
Described in Table 4, across all studies, the overarching health behavioral change strategy emphasized self-management, which included the following subtopics: self-monitoring, personalized feedback/tailored messages, social support and networking groups, goal setting, skill building, and health education1,6–11,17,18,21–25,27–32. Additional health behavior change strategies applied throughout the interventions emphasized reinforcement though the use of rewards and/or incentives7,8,24,31.
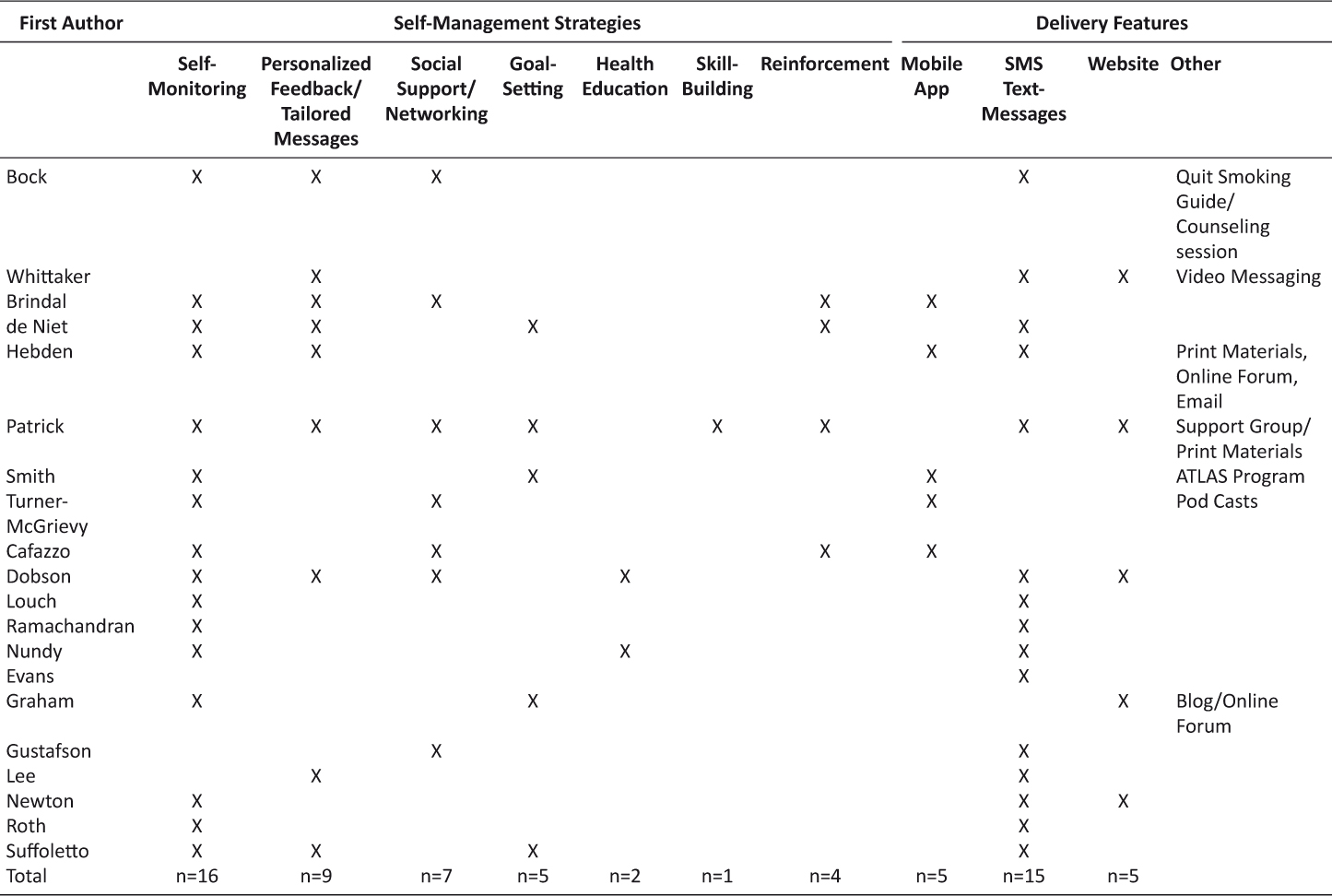
Table 4: Strategies and Features of Intervention Delivery
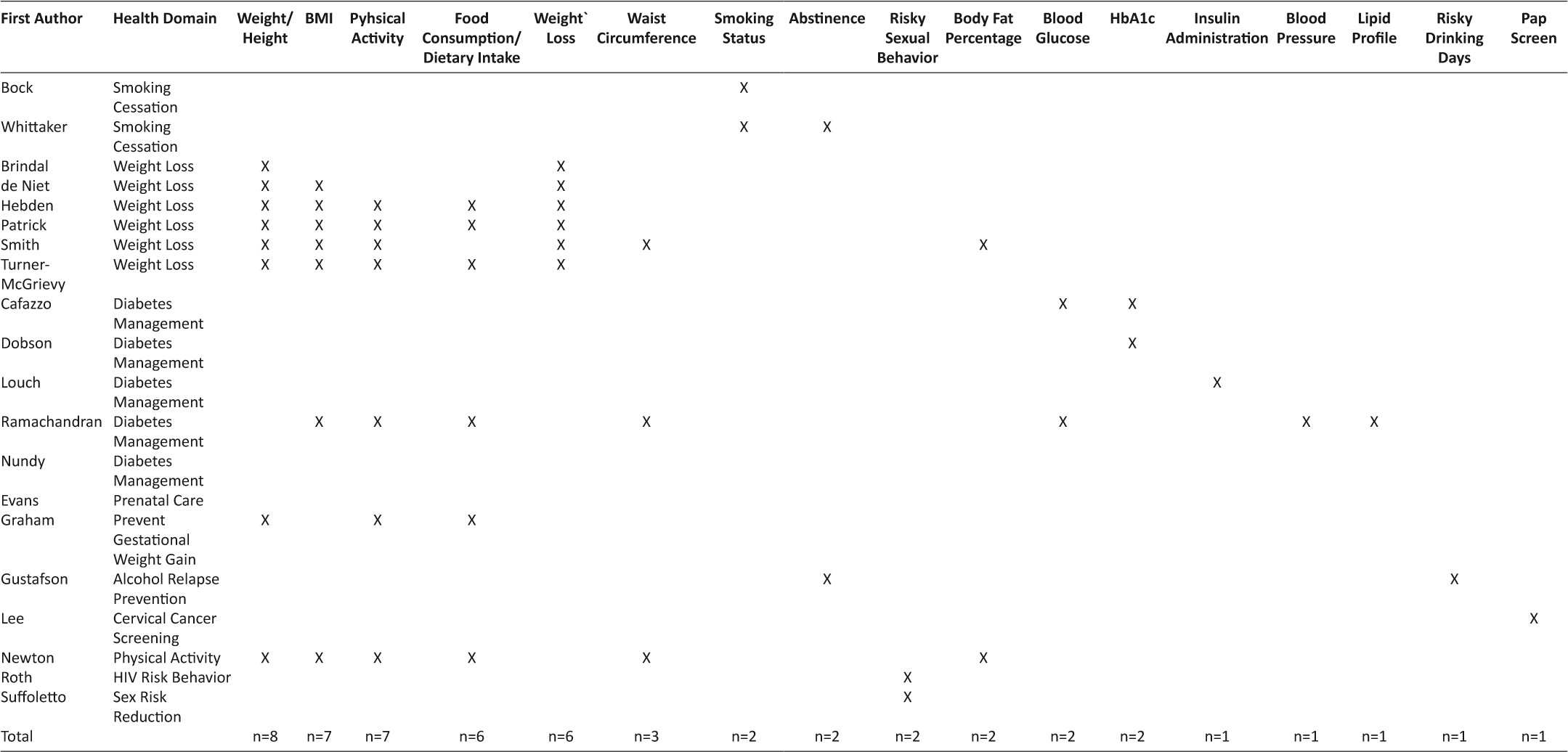
Table 5: Physical and Behavioral Measures
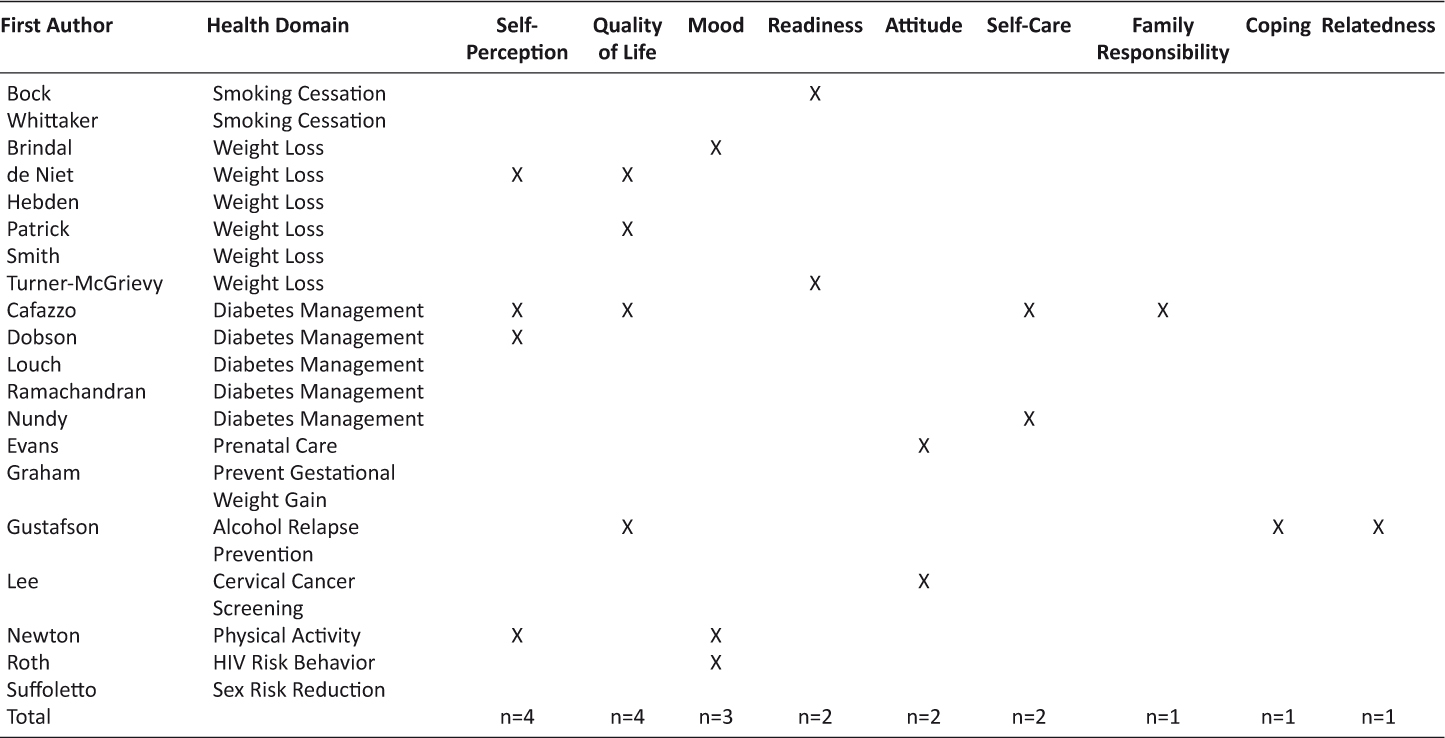
Table 6: Psychological Measures
Features of Intervention Delivery
Also described in Table 4, the studies employed various methods of delivery and behavior change strategies. SMS-text messaging and mobile applications were the most common. Fifteen studies (n=15) incorporated SMS-text messaging to either send reminders, provide education, promote medication adherence, or obtain data via survey administration1,6,8–11,17,18,22,25,27,28,30–32. Five studies (n=5) used mobile apps7,21,23–25. Four (n=4) studies included both SMS-text messaging plus a website1,10,18,31. One (n=1) study included both SMS-text messaging and a mobile app25. Professional and/or social support was also provided through additional methods of intervention delivery which included: video messaging, online forums/support groups, blogs/online forums, pod casts, print materials, and counseling6,10,18,21,23,25,29,31.
The frequency of SMS-text messages reported by investigators varied greatly and ranged from 1- 4 messages sent per day compared to weekly or monthly message schedules. Consequently, some studies did not report the frequency of messages sent or received,8,27,28,30 which is critical to understanding intervention dose. At times, the use of SMS-text messages were unidirectional (one-way and were not intended to promote participant response), resulting in the inability to capture accurate levels of engagement1. Of the studies that tracked participant responses, the response rates fluctuated from 48.8% – 57%1,25 even though 76% of participants in one study chose to receive and participate in interactive messages1.
The second most commonly used technology platform included intervention specific websites. However, websites were oftentimes used in conjunction with SMS-text messaging. Personalized/tailored SMS-text messages were favored over general SMS-text messages in promoting self-management practices. A collective critique of these interventions from study participants were that general messages were focused on broad goals such as weight loss, healthier food choices, work-out regimens, and family planning tips and not focused on the individual’s specific needs1,25.
Outcome Variables
As noted in Tables 5–6, there were a wide-range of outcomes measured by investigators. As a result, all variables were classified into two categories, physical/behavioral measures and psychological measures. Frequently measured physical/behavioral variables included: weight loss, anthropometric measurements (weight/height, waist circumference, BMI), food consumption/dietary intake, and physical activity. Additional variables of interest, cited less frequently in this category included: body fat percentage, current smoking status, abstinence, lipid profile, body fat percentage, blood glucose, HbA1c, insulin administration, risky sexual behavior, and pap screening. Psychological outcome variables included: self-perception, quality of life, and mood were measured most frequently, whereas readiness, self-care, attitude, coping, relatedness, and family responsibility were less emphasized.
The effectiveness of mobile-based interventions varied. Because the studies included in this review addressed multiple physical/behavioral and psychological variables across each health domain (i.e. weight loss, smoking cessation, diabetes management) we analyzed the effectiveness of the intervention and mode of intervention delivery grouped by health domain. The effectiveness of intervention delivery is summarized in Table 7.
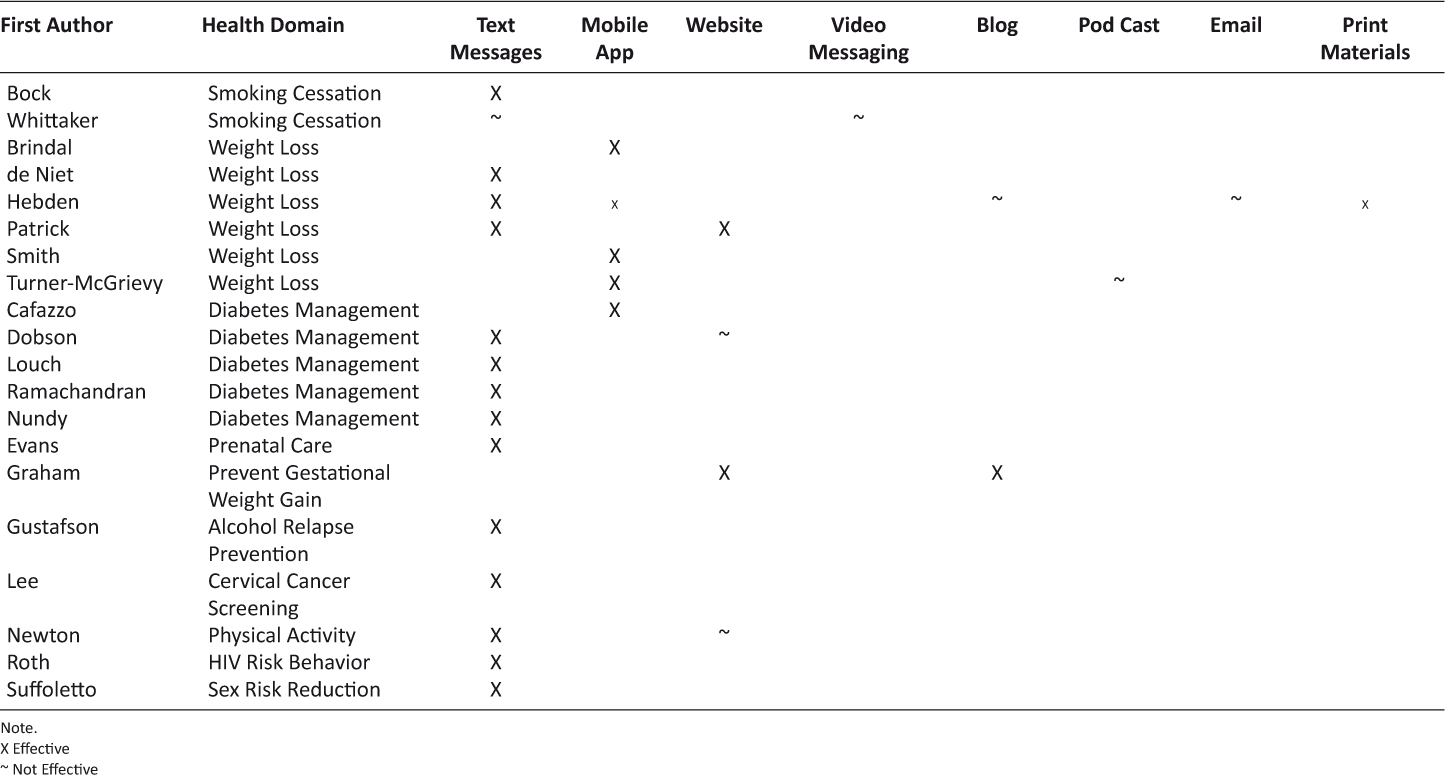
Table 7: Effectiveness of Intervention Delivery
Weight loss interventions.
The majority of studies with a primary outcome measure of weight loss reported no significant differences7,8,21,23,25,31. However, Brindal et al. and Turner-McGrievy and Tate reported that the weight lost by the participants in both groups at week eight was clinically relevant (i.e., 5% or more of total body weight loss)7,23. Additionally, there were some psychological improvements such as mood and motivation of those in the intervention group compared to the control group7. Similarly, two studies reported that although no significant differences in BMI were found between the intervention group and control group; both groups reduced their BMI by the end of the intervention period compared to their baseline measures8,25. Lastly, Patrick et al. and Smith et al. reported significant secondary outcomes (e.g., vegetable and fruit consumption, upper body muscular endurance, resistance training skill competency, and reduced sugar-sweetened beverage consumption)21,31. Overall results suggest that personalized feedback/tailored SMS-text messages were key methods of intervention delivery resulting in more positive weight loss outcomes when compared to generalized text messages7,8,31. Additionally, websites providing education material and mobile apps allowing participants to track food consumption also positively contributed to weight loss outcomes25,31.
Diabetes management interventions.
Of the five studies conducted to improve diabetes management, one study reported improvements in HbA1C1 and three studies reported improvements in secondary outcome measures such as: evening insulin administration doses, HDL cholesterol levels, blood glucose monitoring, foot care, exercise, improved eating habits, and medication adherence11,17,27. Cafazzo et al. reported that daily average frequency of blood glucose measurement increased by 50% 24; Nundy et al. reported significant improvements in each of the major self-care domains measured including medication adherence, self-monitoring of blood glucose, foot care, exercise, and nutrition, in addition to improvements in self- efficacy, social support, and health beliefs11. Louch et al. noted moderate significance in administering evening insulin injections17 p.170 whereas Ramachandran et al. found that the cumulative incidence rate of Type 2 Diabetes was lower in the intervention group compared to the control group and found a significant intervention effect on HDL cholesterol27.
All of these studies were guided by different theories and/or models, but emphasized the construct of self-efficacy. This may suggest that theories and/or models that focus on self-efficacy to promote self-management may be more beneficial in stimulating behavior change. Similar to the weight loss interventions, personalized feedback/tailored SMS-text messages resulted in better self-management of one’s HbA1C1. The inclusion of a website could not be fully evaluated because the target study population had limited Internet access resulting in only partial engagement with this feature 1.
Smoking cessation interventions.
Two studies targeted smoking cessation using personalized/tailored SMS-text messaging, yet only one reported a significance difference in the primary outcome measure, smoking abstinence, reporting increases of smoking abstinence at seven days6. Whittaker et al. also utilized video messaging, but reported no significant differences in the intention-to-treat point prevalence abstinence (no smoking at all in the past 7 days), which were recorded at 1 month, 3 months, and 6 months18.
HIV and sexual risk interventions.
Roth et al. and Suffoletto et al. investigated HIV risk and sexual risk, respectively22,32. Both studies noted positive differences in outcomes. Roth et al. found that engagement with and disclosure of sexual behaviors amongst female sex workers was positively associated with the use of electronic diaries and self-monitoring techniques32. The study enabled the identification of potential social, psychological, and physical reasons resulting in high and/or low levels of sexual risk behaviors32, p. 11. Additionally, Suffoletto et al. reported a significant increase in condom use in the intervention group over the control group from baseline to 3 months after an emergency room discharge22, p. 389. Lee et al. reported that personalized/tailored SMS-text messaging resulted in a significant increase in participants’ knowledge of cervical cancer and receipt of a Pap test30.
Multiple theories and/or models informed these interventions by focusing on not only self-efficacy, but also motivation and risk. Using personalized/tailored SMS-text messaging, researchers were able to uncover sexual risk factors, increase health knowledge, and impact health seeking behaviors across diverse populations.
Other areas (physical activity, recovery from alcoholism, and prenatal care).
The remaining studies focused on physical activity, alcohol relapse prevention and prenatal care and thus, were not grouped with the aforementioned health domains. Newton et al. found significant increases in physical activity and steps per day in both of the intervention groups with no between group differences. Secondary outcome measures included BMI, waist circumference, and body fat percentage, but did not show significant differences between or within intervention groups 10. This suggests that generalized SMS-text messages although somewhat effective may not be the most effective mode of intervention delivery to support physical activity. Similarly, Evans et al. reported that generalized SMS-text messages only improved some target beliefs and attitudes surrounding prenatal healthcare29.
However, Gustafson et al. reported a lower mean number of risky drinking days and a higher likelihood of consistent abstinence than participants in the control group28. Perhaps generalized SMS-text messages enhance motivation and are a strong factor supporting more successful behavior changes related to alcohol consumption. Lastly, Graham et al. reported that over 85% of participants consistently accessed the intervention website, which included informative articles, blog/online forums, and tools to track gestational weight gain. This suggests that a website is also an effective platform to engage study participants29.
Engagement
Described in Table 8. engagement measurements varied across all studies and was reported according to satisfaction, acceptability, feasibility, and adherence. Data were frequently captured by administering surveys and/or interviews and collecting metadata (i.e. timestamps, number of log-ins, responses to SMS-text messages or in-app messages, and interactions with app or web-based features).

Table 8: Engagement Metrics
Satisfaction with the program and mode of intervention delivery was reported by seven studies and was generally measured by administering an end of program survey, whereas one study conducted a semi-structured phone interview. Overall satisfaction with mode of intervention delivery (SMS-text messages) was positive. One study reported that 87% of participants were either satisfied or very satisfied (48/100, 48%) with program delivery6; whereas three studies reported participant satisfaction rates as high as 88%, 97% and 100%, respectively1,24,30.
Participants favored the frequency and timing of SMS-text messages18,25, but suggested that additional human contact, in-person or digitally via online social networking groups, would have been beneficial18. Additional themes such as wanting more personalized messages and possible integration with portable health devices also emerged24,25. This may suggest that not only do participants want targeted messages in order to reach their goals, but also prefer the convenience of using one integrated system to address their health needs.
Acceptance of intervention delivery was also measured by six studies. Of those studies, four described acceptance according to the intervention itself6,7,27,30, whereas two studies described acceptance as it related to digital data collection techniques22,32. Brindal et al. found that in-app message prompting supported continued engagement and a greater frequency of self-reported weigh-ins and dietary compliance7. Nundy et al. also reported that participants felt that informational SMS-text messages aided in organization and reinforcement(12, p.817), whereas, Ramachandran et al. reported that SMS text-messages were helpful with no more than 3% of study participants suggesting that the messages were disturbing them27. Additionally, Lee et al. reported that 97% of study participants would recommend the intervention to friends30. Roth et al. and Suffoletto et al. found that study participants found electronic diaries or questionnaires as an acceptable approach to collect sensitive information, such as risk assessments and track sexual risk behaviors22,32. This may suggest that these techniques increase comfortability and enhance disclosure of health information.
Feasibility of implementing mobile interventions was reported according to participant response rates. Hebden et al. reported a low SMS-text message response rate, 48.8%, even though participants reported being satisfied with frequency of messages and emails received25. Similarly, Smith et al. reported that 44% of study participants self-reported logging pedometer use sometimes, whereas only 30% self-reported logging pedometer use often21. Dobson et al. reported that although 81% of study participants agreed to receive reminder messages, on average, each participant responded to only 56% of messages received1. Understanding the relationship amid engagement metrics is complex, especially when measured differently across studies. Therefore, a key consideration may be to identify motivating factors shared amongst study participants across health domains.
Discussion
The purpose of this scoping review was to provide a thorough description of current theoretically-driven mobile-based interventions focused on improving self-management behavior. Behavioral theories and/or models were identified, features and strategies of intervention delivery were recognized, and effectiveness and engagement were described. Although all studies included at least one behavior change theory/model, specific constructs were not always clearly defined, leaving its application to the intervention obtuse. Theoretical underpinnings are essential in the evaluation of study approaches and design 33. Intervention mapping to constructs and their measures are important to determine which components contributed to the outcomes, and which did not. Because theoretical constructs are not mutually exclusive to a specific framework, we were unable to definitively state which theory and/or model may be better than the next. Studies also spanned a wide range of behavioral/physical and psychological outcome measures, which further limited our capacity to collate and generalize overall findings. Moreover, only 20 articles were included in this review. Expanding the search criteria to more than four academic search databases may have increased the number of eligible studies.
Despite this variety, a few themes pertaining to features of intervention delivery emerged. Participants preferred tailored SMS-text messages over general SMS-text messages. Participants wanted to feel as though their individual needs were the main focus of the intervention1,25, perhaps supporting concepts of the Transtheoretical Model, Social Cognitive Theory, and the Common Sense Model. The utilization of a support group or blogging feature via mobile-application or website forum emphasized by the Health Belief Model was oftentimes noted as a motivating factor that promoted continued use of the intervention. Participants enjoyed the simulated group atmosphere that was provided in the form of blogging and online discussions6,18,21,29. Survey data collection tools were acceptable, easy and convenient way of initiating and maintaining contact with study participants throughout the study period as well as a way to collect follow-up data. Participants reported that survey questionnaires were easy and convenient to complete when promoted via SMS-text messaging22,30,32.
Due to the growing number of mobile-based interventions, additional intervention research grounded in theory is needed. Beyond efficacy, there are many contextual factors that need to be considered that promote translation of an efficacious intervention into practice and sustainability of intervention engagement. Such factors geographic location, ease of use, usability, population of interest, and potential barriers to usage33. Although some investigators did capture a few contextual factors of usage and engagement, these variables may need to be explored in greater depth.
Future work should focus on the application of theory and how various implementation techniques translate to the overall effectiveness of the intervention. Because the number of mobile-based interventions guided by theories and/or models is limited, future studies are needed to clearly identify not only applicable theories/models of behavior change, but the specific constructs to determine which components are most effective and can be delivered remotely. This further emphasizes the need to streamline links between theory, intervention, and implementation.
Acknowledgements
We would like to thank Stella Seal, the academic librarian who aided in developing the search criteria that guided this review; Dr. Jacquelyn Campbell for her insight and expertise that directed the components of the review; and Dr. Harold Lehmann who helped support the development of visual aids to effectively display the theories and/or models and techniques applied per intervention.
Conflicts of Interest
The author(s) declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
References
1. Dobson R, Carter K, Cutfield R, et al. Diabetes Text-Message Self-Management Support Program (SMS4BG): A Pilot Study. JMIR mHealth uHealth. 2015;3(1):e32. ![]()
2. Ward BW, Schiller JS, Goodman RA. Multiple Chronic Conditions Among US Adults: A 2012 Update. Prev Chronic Dis. 2014;11(3):4-7. ![]()
3. Whitehead L, Seaton P. The effectiveness of self-management mobile phone and tablet apps in long-term condition management: A systematic review. J Med Internet Res. 2016;18(5). ![]()
4. Ginexi EM, Riley W, Atienza AA, Mabry PL. The promise of intensive longitudinal data capture for behavioral health research. Nicotine Tob Res. 2014;16(S2):S73-S75. ![]()
5. Holman H, Lorig K. Patient self-management: a key to effectiveness and efficiency in care of chronic disease. Public Health Rep. 2004;119(3):239–243. ![]()
6. Bock B, Heron K, Jennings E, Morrow K. A Text Message Delivered Smoking Cessation Intervention : The Initial Trial of TXT-2-Quit : Randomized Controlled Trial. J Med Internet Res. 2013;1(2):e17–e27. ![]()
7. Brindal E, Hendrie G, Freyne J, Coombe M, Berkovsky S, Noakes M. Design and pilot results of a mobile phone weight-loss application for women starting a meal replacement programme. J Telemed Telecare. 2013:166–174. ![]()
8. de Niet J, Timman R, Bauer S, et al. The effect of a short message service maintenance treatment on body mass index and psychological well-being in overweight and obese children: a randomized controlled trial. Pediatr Obes. 2012;7(3):205–219. ![]()
9. Evans WD, Bihm JW, Szekely D, et al. Initial outcomes from a 4-week follow-up study of the text4baby program in the military women’s population: Randomized controlled trial. J Med Internet Res. 2014;16(5):1–18. ![]()
10. Newton RL, Marker AM, Allen HR, et al. Parent-Targeted Mobile Phone Intervention to Increase Physical Activity in Sedentary Children: Randomized Pilot Trial. JMIR mHealth uHealth. 2014;2(4):e48. ![]()
11. Nundy S, Mishra a., Hogan P, Lee SM, Solomon MC, Peek ME. How Do Mobile Phone Diabetes Programs Drive Behavior Change?: Evidence From a Mixed Methods Observational Cohort Study. Diabetes Educ. 2014;40(6):806–819. ![]()
12. Pew Research Center. Emerging Nations Embrace Internet, Mobile Technology. Pew Res Cent. 2014: 1-10. http://www.pewglobal.org/files/2014/02/Pew-Research-Center-Global-Attitudes-Project-Technology-Report-FINAL-February-13-20147.pdf.
13. Aaron BY, Http S, Pewresearch WWW, Staff ORG. U. S . Smartphone Use in 2015.; 2015. http://www.pewinternet.org/2015/04/01/us-smartphone-use-in-2015/.
14. Olff M. Mobile mental health: A challenging research agenda. Eur J Psychotraumatol. 2015;6:1-8. ![]()
15. Pinto MD, Greenblatt AM, Hickman RL, Rice HM, Thomas TL, Clochesy JM. Assessing the Critical Parameters of eSMART-MH: A Promising Avatar-Based Digital Therapeutic Intervention to Reduce Depressive Symptoms. Perspect Psychiatr Care. 2016;52(3):157–168. ![]()
16. Glasgow RE, Christiansen SM, Kurz D, et al. Engagement in a diabetes self-management website: Usage patterns and generalizability of program use. J Med Internet Res. 2011;13(1):e9–e33. ![]()
17. Louch G, Dalkin S, Bodansky J, Conner M. An exploratory randomised controlled trial using short messaging service to facilitate insulin administration in young adults with type 1 diabetes. PsycholHealth Med. 2013;18(1465-3966 (Electronic)):166–174.
18. Whittaker R, Dorey E, Bramley D, et al. A theory-based video messaging mobile phone intervention for smoking cessation: Randomized controlled trial. J Med Internet Res. 2011;13(1):1–19. ![]()
19. Institute JB. The Joanna Briggs Institute Reviewers ’ Manual 2015 Methodology for JBI Scoping Reviews.; 2015.
20. Tricco AC, Lillie E, Zarin W, et al. A scoping review on the conduct and reporting of scoping reviews. BMC Med Res Methodol. 2016;16(15):1–10. ![]()
21. Smith JJ, Morgan PJ, Plotnikoff RC, et al. Smart-Phone Obesity Prevention Trial for Adolescent Boys in Low-Income Communities: The ATLAS RCT. Pediatrics. 2014;134(3):e723–e731. ![]()
22. Suffoletto B, Akers A, McGinnis K a., Calabria J, Wiesenfeld HC, Clark DB. A sex risk reduction text-message program for young adult females discharged from the emergency department. J Adolesc Heal. 2013;53(3):387–393. ![]()
23. Turner-McGrievy G, Tate D. Tweets, Apps, and Pods: Results of the 6-month Mobile Pounds Off Digitally (Mobile POD) randomized weight-loss intervention among adults. J Med Internet Res. 2011;13(4):1–14. ![]()
24. Cafazzo J a., Casselman M, Katzman DK, Palmert MR. Design of an mHealth App for Adolescent Type I Diabetes – A Pilot Study. J Med Internet Res. 2012;14(3):S77–S78. ![]()
25. Hebden L, Cook A, van der Ploeg HP, King L, Bauman A, Allman-Farinelli M. A mobile health intervention for weight management among young adults: a pilot randomised controlled trial. J Hum Nutr Diet. 2014;27(4):322–332. ![]()
26. Glynn LG, Hayes PS, Casey M, et al. SMART MOVE – a smartphone-based intervention to promote physical activity in primary care: study protocol for a randomized controlled trial. Trials. 2013;14:157. ![]()
27. Ramachandran A, Snehalatha C, Ram J, et al. Effectiveness of mobile phone messaging in prevention of type 2 diabetes by lifestyle modification in men in India: A prospective, parallel-group, randomised controlled trial. Lancet Diabetes Endocrinol. 2013;1(3):191–198. ![]()
28. Gustafson DH, Mctavish FM, Chih M, et al. A Smartphone Application to Support Recovery From Alcoholism : A Randomized Clinical Trial. JAMA Psychiatry. 2014;71(5):1–13. ![]()
29. Graham ML, Uesugi KH, Niederdeppe J, Gay GK, Olson CM. The Theory, Development, and Implementation of an e-Intervention to Prevent Excessive Gestational Weight Gain: e-Moms Roc. Telemed e-Health. 2014;20(12):1135–1142. ![]()
30. Lee HY, Koopmeiners JS, Rhee TG, Raveis VH, Ahluwalia JS. Mobile Phone Text Messaging Intervention for Cervical Cancer Screening: Changes in Knowledge and Behavior Pre-Post Intervention. J Med Internet Res. 2014;16(8):e196. ![]()
31. Patrick K, Norman GJ, Davila EP, et al. Outcomes of a 12-month technology-based intervention to promote weight loss in adolescents at risk for type 2 diabetes. J Diabetes Sci Technol. 2013;7(3):759–770. ![]()
32. Roth AM, Hensel DJ, Fortenberry JD. Feasibility and acceptability of cell phone diaries to measure HIV risk behavior among female sex workers. AIDS Behav. 2015;18(12):2314–2324. ![]()
33. Sutton SM, Magwood GS, Jenkins CH, Nemeth LS. A Scoping Review of Behavioral Weight Management Interventions in Overweight/Obese African American Females. West J Nurs Res. 2016;38(8):1035–1066. ![]()

