A mobile electronic record for lifestyle coaches in gestational diabetes prevention
David Simmons FRACP MD1, Tosin Daniels BSc (Hons)2, Daniel J Simmons BEng3, Mireille NM van Poppel4, Jürgen Harreiter MD5
1Western Sydney University, NSW, Australia and Cambridge University Hospitals, Cambridge, England
2Cambridge University Hospitals, Cambridge, England
3Techtonic Software, Norfolk, England
4Department of Public and Occupational Health, EMGO+-Institute for Health and Care Research, VU University Medical Centre, 1081 BT Amsterdam, the Netherlands and Institute of Sport Science, University of Graz, 8010 Graz, Austria
5Department of Medicine III, Division of Endocrinology, Gender Medicine Unit Medical University of Vienna
On behalf of the DALI core investigators group (see Appendix)
Corresponding author: da.simmons@westernsydney.edu.au
Journal MTM 8:1:37–49, 2019
Background: Lifestyle programmes require a structured approach to be effective. Maintaining fidelity of coach-based interventions is challenging. Mobile devices may assist by supporting the use of an algorithm based approach.
Aims: To describe the development and challenges associated with a mobile technology approach to supporting a coach-based lifestyle programme for the prevention of gestational diabetes mellitus (GDM) in pregnancy.
Methods: Narrative approach to system design, with a survey of 12 lifestyle coaches involved in the pan-European multicentre DALI (Randomised controlled trial for the prevention of gestational diabetes mellitus (GDM) with vitamin D And Lifestyle Intervention) study.
Results: A mobile device based programme was associated with more technical issues than a web-based approach, particularly in relation to upgrades to improve usability and utility. Even after multiple upgrades, a paper approach was preferred by some coaches, and by most for aspects of the intervention that required greater coach-participant interaction (eg goal setting). Coaches generally preferred the mobile device approach for obtaining pre-existing data, structured data entry and for intervention prompts.
Conclusion: Mobile technology can facilitate coach-delivered lifestyle interventions. However, more work is required to minimise intrusion into the behavioural intervention.
Introduction
Type 2 diabetes (T2DM) has now been shown to be preventable through weight loss, increased physical activity and appropriate dietary change (1). Successful randomised controlled trials (RCTs) for preventing T2DM included coaching interventions provided within a curriculum (2), with the major studies being ‘classroom’ or clinic based (2-3). It has been a challenge to create widespread diabetes prevention services (4) translated from such intensive interventions, applied by a small number of ‘coaches’, to RCT participants within a single country. Besides the difficulty of obtaining funding for such programmes, a major issue is the fidelity (ie the degree to which the intervention is correctly implemented) of any intervention implemented by non-research staff, outside of the rigour of an RCT. The Diabetes Prevention Program (DPP) showed that the more of the lifestyle messages that were taken up, the lower the probability of incident T2DM (2), and hence any reduction in fidelity could reduce the effectiveness of the intervention.
Elsewhere in health services, the need to improve the quality of interventions is an area that is addressed by quality assurance programmes. In diabetes, there has been a range of strategies trialled with varying effectiveness, including improvements in documentation (5). Diabetes electronic records continue to progress, but uptake has been varied (6,7). Mobile computing has been seen as one way of improving care (8,9). The potential benefits were identified as: (i) faster, real time access to and recording of health data, (ii) provision of decision support, and (iii) translation of knowledge into practice (7). However a range of challenges remain in introducing such systems into healthcare (6-9).
DALI (Randomised controlled trial for the prevention of gestational diabetes mellitus (GDM) with vitamin D And Lifestyle Intervention) included a range of lifestyle interventions for the prevention of GDM across 9 European countries (10). The lifestyle programme was based upon a series of 12 messages (7 Healthy Eating (HE) and 5 Physical Activity (PA)) delivered following Motivational Interviewing principles, and was associated with significant reductions in gestational weight gain (11,12). Rather than a curriculum based approach, a key component involved the woman prioritising interventions and working with the support of a coach to set and achieve goals. The approach was based upon prior work in New Zealand (13), where Maori Community Health Workers used a structured electronic record on a personal digital assistant (PDA) to support a lifestyle programme among adult Maori. The intervention used data collected at baseline, from self-monitoring and from prior coaching sessions. There was a need to be able to review which messages had been covered and to be able to review progress (eg. weight change) for each participant. In view of these needs, it was decided to incorporate a handheld computing device. The data collected were to be part of a process evaluation of intervention implementation in the trials. We now describe the development and usability of the DALI lifestyle coaching e-support programme, including problems encountered and how these were overcome.
Methods
DALI study design overview
Interventions to prevent gestational diabetes mellitus (GDM) remain unproven (14). DALI developed 3 lifestyle interventions: HE, PA and HE+PA (10). The 3 interventions were piloted (11), and then used in one RCT of HE, PA, HE+PA vs controls (13) and one RCT of Vitamin D tablets (VDT)+HE+PA vs VDT+no lifestyle intervention vs placebo+HE+PA vs no intervention (10). The trials invited pregnant women at risk of GDM (BMI≥29 (kg/m2) from 9 European countries to have a 75g oral glucose tolerance test before 20 weeks gestation. Those without GDM (15) were randomized to an intervention group, pre-stratified for each site. Women received 5 face-to-face, and 4 telephone coaching sessions from consent to 35 weeks, based on motivational interviewing principles, supported by a bespoke record system using a handheld electronic device (HTC HD7, HTC Corporation, Taiwan), or similarly structured paper methodology. An optimal gestational weight gain (GWG) target of <5kg was emphasized. Coaches were health workers recruited locally (eg midwives, nurses, pharmacy technician, health coaches, doctor) and attended 3 training and standardisation workshops through the trials. All coaches were required to be able to be fluent in English. Trial data (questionnaire, OGTT, measurements) were collected at baseline, 24-28 weeks, 35-37 weeks and at birth and entered directly into a bespoke database using MySQL with unique identifier and separate tabs for each time point. Data were entered by research staff who were kept separate from the coaches to maintain integrity of the randomisation.
DALI lifestyle coaching e-support programme development
The architecture was developed from experience gained with the use of a personal digital assistant (PDA) to help structure, guide and record coach-participant interactions in Te Wai o Rona: Diabetes Prevention Strategy (13). Steps taken were design of the algorithm, architecture, hardware and software choices, screen development, software development including security, navigation approaches, linkage with the server and server development. The original DALI design involved a PDA holding an electronic coach record (the application front-end), with an anonymised data back up synchronised with the DALI database after each coaching session. Data on the database was then to be used for feedback to the coach, using the study ID, and reporting progress to the wider project group (Figure 1). The server was expected to periodically create data backups stored on a separate drive.
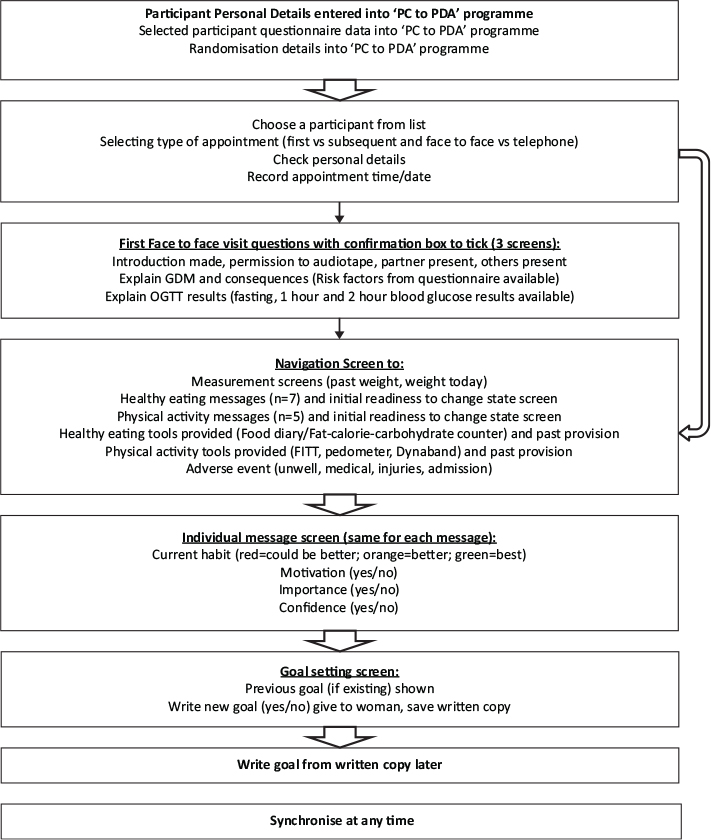
Figure 1: System Algorithm.
Key:
Physical activity interventions (n=5): “Be active every day”; “Sit less”; “Build your strength”; “Take more steps”; “Be more active at weekends”
Healthy Eating interventions (n=7): “Replace sugary drinks”; “Eat more non-starchy vegetables”; “Increase fibre consumption”; “Watch portion size”; “Eat protein”; “Reduce fat intake”; “Eat less carbohydrates”
Stages of change (1-5): Precontemplative; Contemplative; Preparation; Action; Maintenance
Advances in mobile technology allowed the upgrading of the PDA to a mobile phone, and the HTC HD7 (HTC Corporation, Taiwan) was selected for its large screen and Windows operating system (the system used in Te Wai o Rona: Diabetes Prevention Strategy). However, the newer Windows 7 operating system (Microsoft, USA) required a complete rewrite of the intervention application. Coaches had varying experience with information technology and implemented the system at varying rates. A default paper system was designed to incorporate the stages in the algorithm for times when the electronic system was not able to be used.
Screens were developed for each stage in the algorithm, designed to streamline the coach-participant interaction and ensure that each aspect of the intervention was either completed, or an active bypassing decision made (eg. for time reasons). Screens were structured for easy use, with large buttons for touchscreen completion. Writing into the programme was minimised, and completed through the on-screen keyboard. A traffic light system was used to indicate where the participant reported to the coach the uptake of a given message and whether it had progressed (green), regressed (red) or was intermediate (orange). Navigation was developed based upon the flow of the expected coaching interview. The key navigation screen provided 6 buttons to the measurements section, 7 HE messages, HE tools provided, 5 PA messages, PA tools provided and adverse events. Data saving was possible at key points through the screens.
Security features included 256 bit AES encryption and separation of any identifying information from actual research data. All coaches had their own identifier and password. Data entered into the handheld programme could be saved and used as the basis for creating appointments on the phone. Any programme updates, were downloaded from the Microsoft App store.
The original plan of linking to the DALI trial database was abandoned after the trial database was built, for security reasons, without an outward facing functionality that prevented receipt of mobile phone data. The repercussions of this were:
• The need to procure a separate server for the mobile computing with new software development
• The need for a separate office PC-based bespoke programme (called the ‘PC to PDA programme’), written in C# (Microsoft, USA), for blinded research staff to re-enter baseline questionnaire data to allow direct upload to the PDA through a cradle. Direct uploading was decided upon for security reasons. Zune client software (Microsoft, USA) was selected as the programme for linking the ‘PC to PDA programme’ with the PDA.
The server-side of this new system proved difficult to implement, and was ridged when changes needed to be made to the database (either with results or the data itself). The system on the client side had a number of minor problems mostly revolving around the international nature of the project, making debugging the application and giving support to coaches difficult through a phone application. The client application required local data to be stored on the mobile phone, which made it volatile due to the nature of the Windows Phone 7 Operating system, storing data in isolated storage (which is deleted if the application was uninstalled) and the data not being sent to the server as soon as an appointment/intervention was completed. Distance was an issue, there being no direct way of accessing data stored by the application. Storing data in a usable format on the phone was also a challenge due to the Windows phone still being in semi-early development.
The server side system was eventually replaced by a direct MYSQL approach (Oracle Corporation, USA) with all data being created and stored instantly on the main database via the use of a PC Client application which connected to the main database via the internet. During this period, the paper PDA was used by the coaches, rather than the mobile phone application itself. This meant that no data was stored locally and removed the potential for data loss or corruption either through program fault/malfunction or human error. This was soon followed by a scaled-down PDA/phone client application that acted more as a portable intervention creator that was then sent to the server and viewed through the PC client. In this way, the risk of data loss on the client side was significantly minimized to the scope of about one or two appointments.
Reporting system
The ongoing need to identify the causes of difficulties with the system (user issues, international site intranet issues, software issues, server issues) delayed the development of the reporting system which needed a foundation of a stable, operating architecture. This was not achieved until the MYSQL based system was developed and too late to be used in the trials themselves. The system commenced with 4 reports:
• Report 1: % of women receiving all 3 of introduction, GDM explanation, blood result explanation
• Report 2: % of women with no weight taken
• Report 3: % of women with weight taken whose current weight minus baseline weight is less than or equal to 5kg
• Report 4: % of messages covered for each woman in the intervention group
Training programme
Coaches were provided with the Manufacturer User Guide for the mobile device, and a manual for the coach e-support system that covered each stage in the algorithm. The manual also covered the ‘authorised user’ policy, security aspects, who to contact should problems arise and general issues relating to the phone. Coaches were required to practice on a simulation system before commencing, and to describe the positive and negative aspects of the system. Online updates were provided including a user video. Updates were provided via email. A ‘clinic’ was provided at the end of the pilot and midway through the first Lifestyle RCT.
Evaluation
The uptake of the system was continuously monitored either by email or reviewing the use of the database. At the end of the pilot study and after the migration to the PC client system, questionnaires (shown in Tables 4–6) were used as way to gather the coaches opinions on issues surrounding technology options, the usability of the PDA device and wider applicability of the PDA for delivering the DALI messages. The short questionnaire was distributed to the 12 coaches by email. A thematic analysis was used to list the issues identified. The monitoring system was not completed until after the completion of the PC client system and was not used for feedback. The DALI studies received ethics approval across all local ethics committees.
Results
Ultimately, of the 12 coaches trained in the use of the system, 3 used the system in the intervention fully. Table 1 lists the number of coaches using different components of the system. At least one survey was received from each coach within the lifestyle RCT. Table 2 describes the advantages and disadvantages reported by the coaches in using the system. Advantages related largely to accessibility of data and some design aspects. Disadvantages were largely technical, although there were unexpected difficulties due to international differences in the way punctuation is used (eg full stop (UK) vs comma (Europe) for the decimal point). Table 3 describes the technical issues encountered by the coaches. All were eventually resolved, but tool time impacted on the attitudes of the users to the new technology. Table 4 shows that the users reported that most of the features worked well. The main areas of difficulty related to connecting to the internet and the inability to correct errors. Approximately 50% of the coaches reported the training was adequate. Table 5 shows the user ratings for different aspects of the system. Overall, among users, the HTC HD7 was rated 5/10, the DALI PDA programme 4.3/10, the DALI PC to PDA programme 6/10, the PC client programme 6.9/10 and the paper PDA 7.6/10. All coaches used the PC client and Paper PDA. Table 6 shows the preferred methodologies were largely electronic for administrative items, but paper for more complex issues relating to the behavioural intervention.

Table 1: Uptake of the e-DALI system
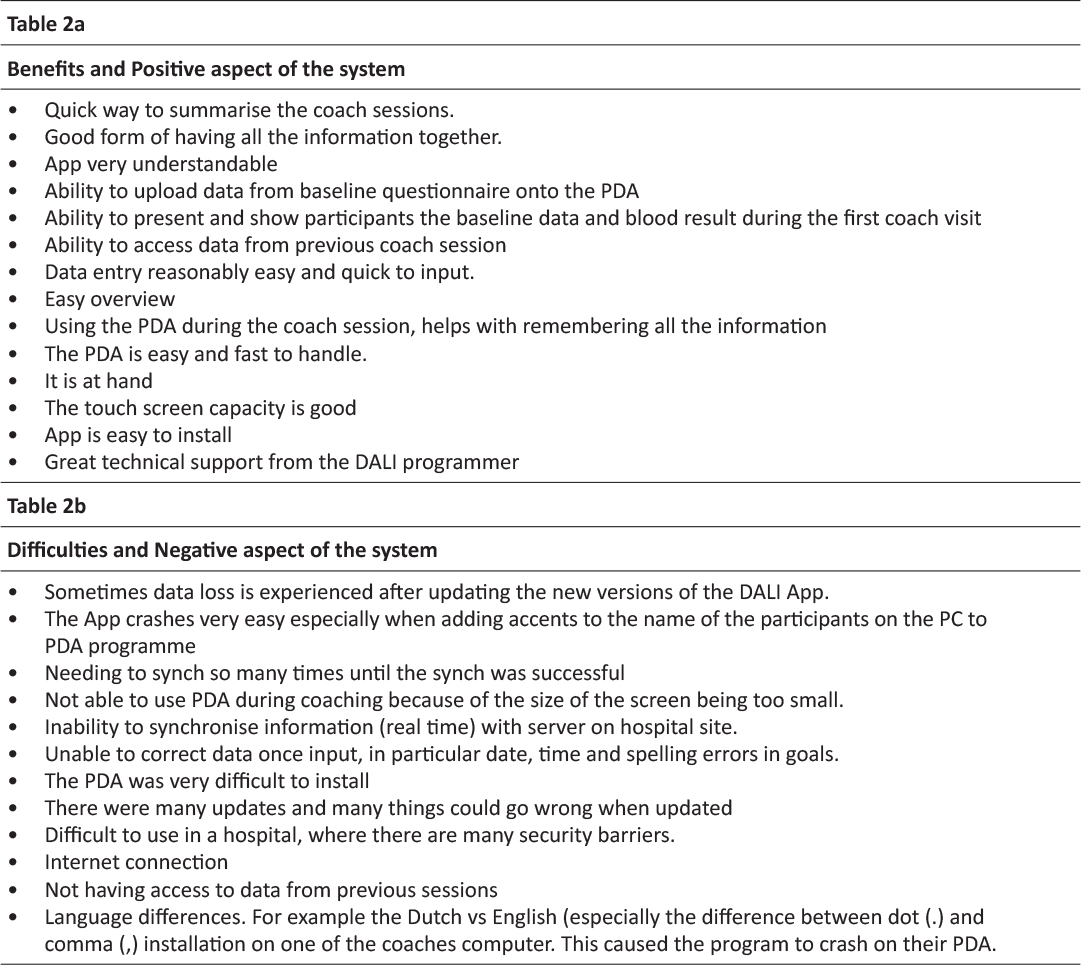
Table 2: Advantages and disadvantages of the system reported by the coaches
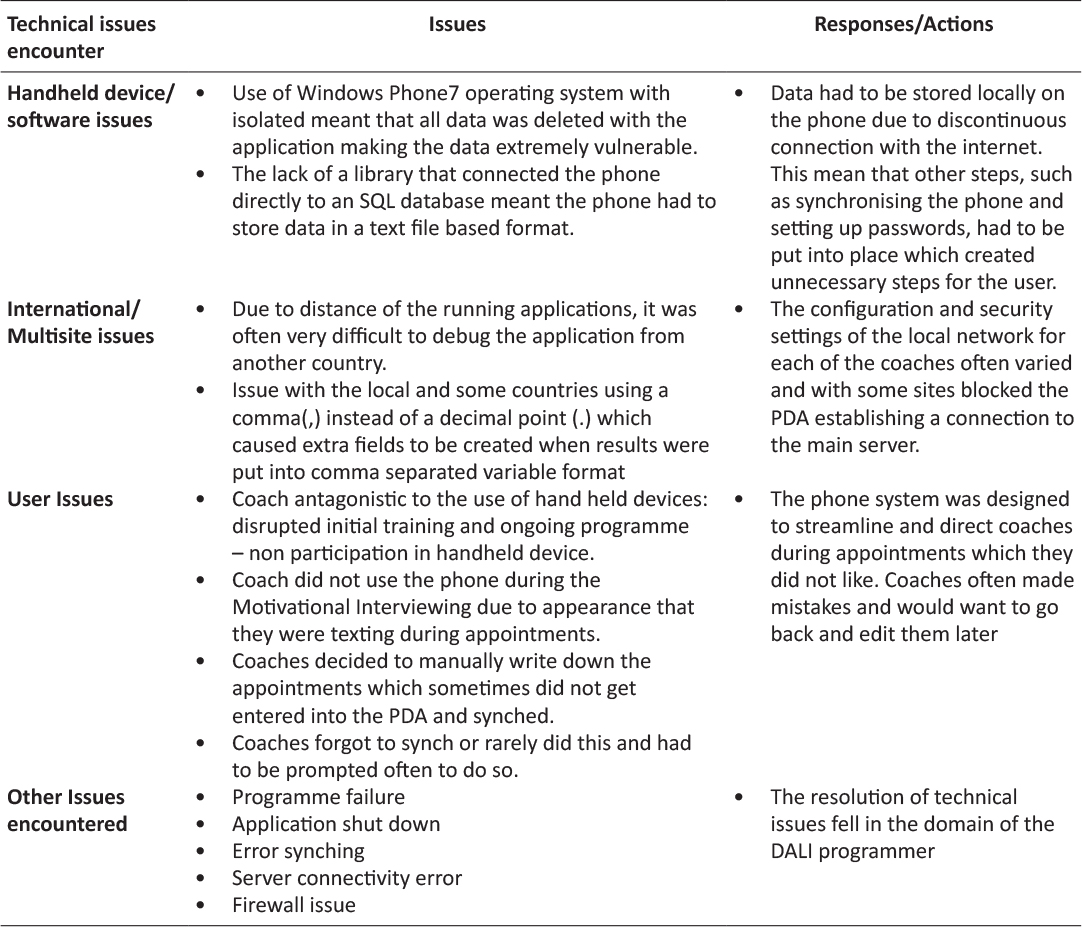
Table 3: Technical issues encountered.
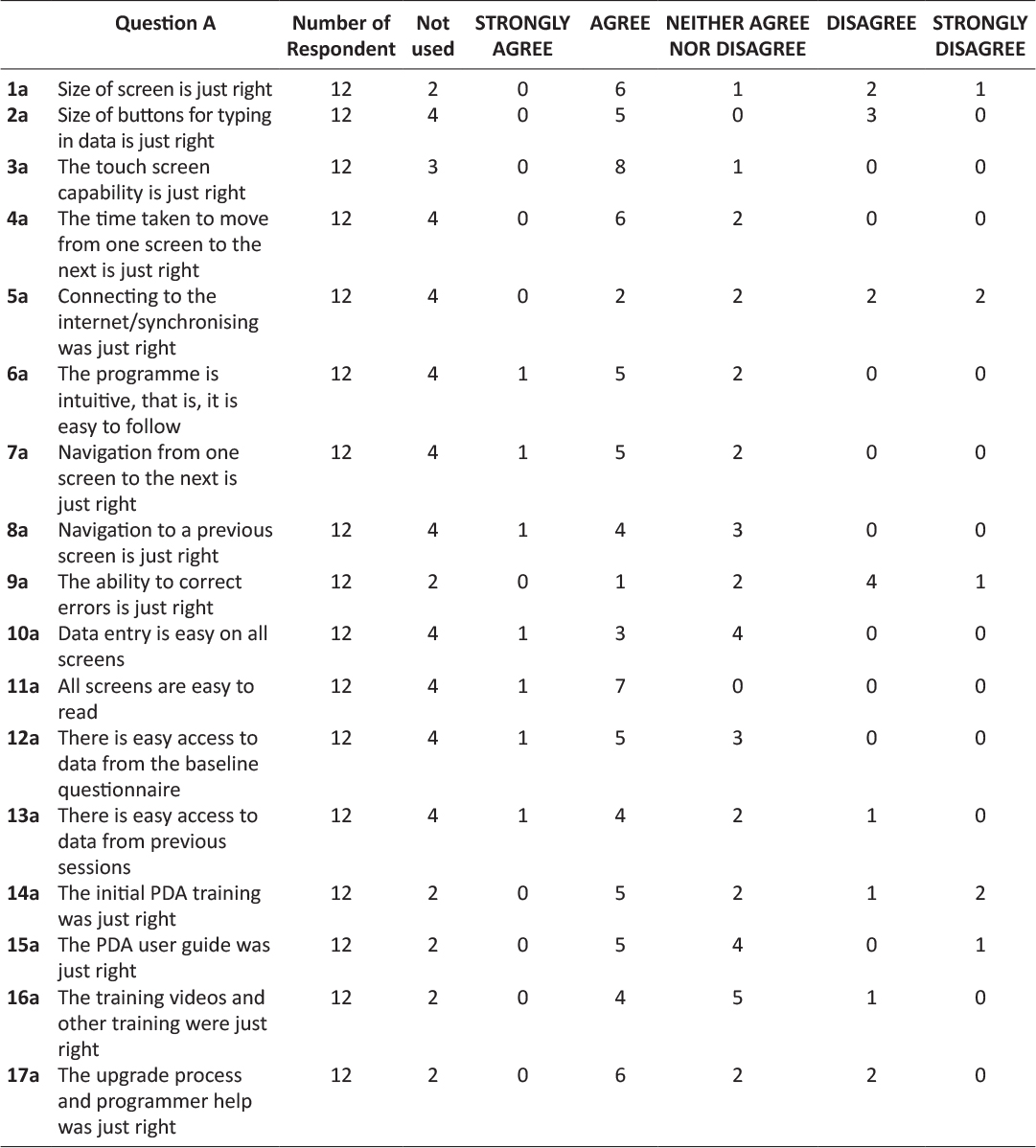
Table 4: PDA USER- EVALUATION QUESTIONNAIRE – Programme/Physical issues.
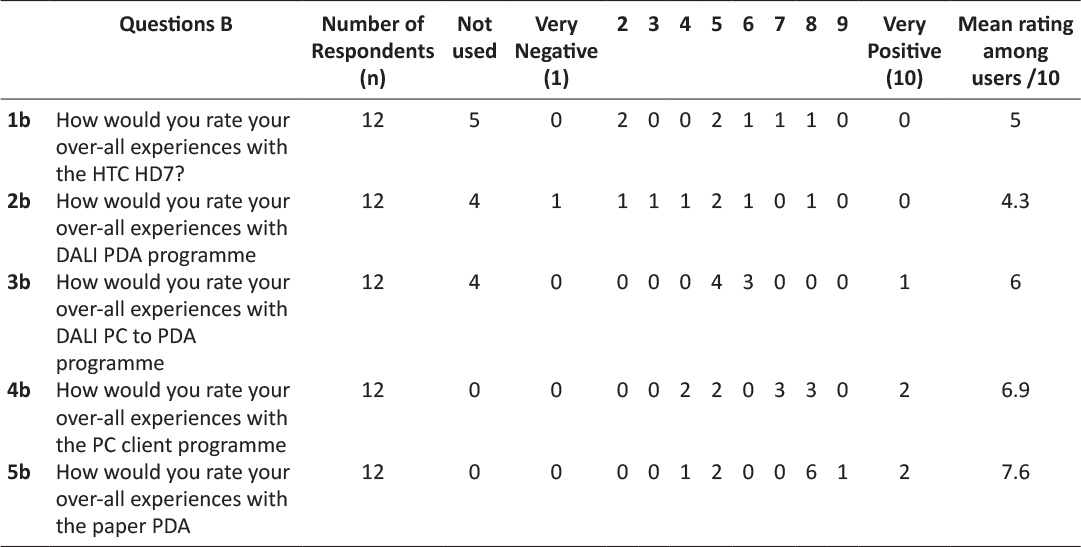
Table 5: PDA USER- EVALUATION QUESTIONNAIRE –Experience rating

Table 6: PDA USER- EVALUATION QUESTIONNAIRE –Preferred methodology
Discussion
Effectiveness
We have described the development, experience and evaluation of a mobile electronic record for lifestyle coaches involved in the prevention of GDM through lifestyle change. The experience was gained within randomised trials across 9 European countries over 3-4 years between 2010 and 2014. While many lifestyle applications now exist (16), the DALI application was tailored to the work undertaken by the DALI coaches for an intervention based upon the Health Action Process Approach (HAPA) model (10) for behavioural change, across 12 key lifestyle messages including goal setting and review. As the delivery to all trial participants was managed using the algorithm developed, either through the ‘paper’ or electronic ‘PDA’, our evaluation is unable to state whether the paper or electronic approach was more effective, just that the DALI intervention itself was effective in limiting gestational weight gain (11,12).
Preference
The electronic forms (PDA/PC client) was preferred for recording data (eg. type of appointment, measurements) and obtaining prior data (eg. personal details). Similar preference was stated between electronic forms and the paper PDA for explaining results and discussing interventions including choice of tools and recording adverse events. The paper PDA was preferred for goal setting, which requires more free text. There were occasional strong preferences for and against the use of the electronic PDA, generally based upon the ease of the technology with a capability to incorporate the technology, versus a concern over the intrusion of the technology into the flow of the coach- participant motivational interviewing.
Usability and utility
There remains evolving debate over how to define usability and utility. In his 1994 text, Nielson included a broad and deep definition to include “Efficiency (Resources expended in relation to the accuracy and completeness with which users achieve goals), Satisfaction (Freedom from discomfort, and positive attitudes towards the use of the product), Learnability (The system should be easy to learn so that the user can rapidly start getting work done with the system), Memorability (The system should be easy to remember so that the casual user is able to return to the system after some period of not having used it without having to learn everything all over again), Errors (The system should have a low error rate, so that users make few errors during the use of the system and that if they do make errors they can easily recover from them and further, catastrophic errors must not occur) and Utility (the ability of a system to meet the needs of the user).” (17 as summarised in 18). Others have narrowed this down to effectiveness, efficiency and satisfaction (18). A range of applications have been reviewed using the System Usability Scale (19), covering a range of features. Our coach survey revealed a range of issues impacting on usability, but we suspect that these were heavily influenced by the prior perspective of the coach on technology and technology use during a motivational interviewing encounter. Whether clients feel that when their coach uses a PDA or another screen based device interferes with rapport and quality counselling would be of interest to study further in other settings. One issue that was not initially expected in the programming arose from the international nature of the study with the different uses of commas, full stops and accents. This was addressed, but such events, as ‘developer errors’ reduced confidence in the system, and this itself appeared to be influenced by the pre-existing attitude to the technology. The workshops and rapid feedback, addressing issues as they arose, were used to improve confidence, but with some coaches, confidence remained low as the issues occurred on top of some of the other barriers that were outside of the control of the developers (eg the firewall issues).
Privacy and security
The electronic PDA and the PC to PDA programme held identifiable data. The former was used with the participant and had significant security as a password protected handheld device. The latter was within a password protected personal computer, within the firewall of the health service site. The server never held personal data, and was linked via a participant identifier. As a result, the personal details were protected within the limits of sensible password use.
Technical issues
This work involved a stream of technical issues from the beginning with the requirement to operate independently from the trial database, to the need to upgrade the operating system, to the difficulties with operating the PC to PDA system within the intranet of the health service site. Many of the ‘user’ requests related to the local intranet/internet administration, and not the DALI programmes. Nevertheless, each time there was a problem with the local information technology, it undermined the credibility of the DALI system. Most of the difficulties hinged on two issues (1) the underdeveloped Windows Phone 7 system which had no official support for sequel databases at the time; and (2) the lack of a live connection to the database as well as the absence of a guarantee of standard of network facilities or access to internet.
Conclusion
The DALI system through the PC client/web based approach ended up as the preferred electronic system, albeit with some caveats over longer text entry associated with goal setting. Further field trials are warranted should similar lifestyle interventions be undertaken. Besides testing the effectiveness of the approach, whether such mobile technology will improve the fidelity of interventions would be worthwhile investigating.
Funding: The project described has received funding from the European Community’s 7th Framework Programme (FP7/2007-2013) under grant agreement no 242187. In the Netherlands, additional funding was provided by the Netherlands Organisation for Health Research and Development (ZonMw) (Grant nr. 200310013). In Poland, additional funding was obtained from Polish Ministry of Science (Grant nr 2203/7. PR/2011/2). In Denmark, additional funding was provided by Odense University Free Research Fund. In the UK, The DALI team acknowledge the support received from the NIHR Clinical Research Network: Eastern, especially the local diabetes clinical & research teams based in Cambridge. In Spain, additional funding was provided by CAIBER 1527-B-226. The funders had no role in any aspect of the study beyond funding.
Conflict of interest: DJS was paid as the software and system developer for the DALI systems, but was not involved in the evaluation of the software.
References
1. Gillett M, Royle P, Snaith A, et al. Non-pharmacological interventions to reduce the risk of diabetes in people with impaired glucose regulation: A systematic review and economic evaluation. Health Technol Assess. 2012;16(33):1-236. ![]()
2. Knowler WC, Barrett-Connor E, Fowler SE, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. The New England Journal of Medicine. 2002;346(6):393-403. ![]()
3. Tuomilehto J, Lindström J, Eriksson JG, et al. Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. New England Journal of Medicine. 2001;344(18):1343-1350. ![]()
4. Dunbar JA , Hernan AL , Janus ED et al. Challenges of diabetes prevention in the real world: results and lessons from the Melbourne Diabetes Prevention Study. BMJ Open Diabetes Res Care 2015; 3: e000131 ![]()
5. Tricco A.C. et al. Effectiveness of quality improvement strategies on the management of diabetes: A systematic review and meta-analysis. The Lancet, 2012;379:2252-61 ![]()
6. Joshy G, Simmons D, Diabetes Information Systems: A Rapidly Emerging Support for Diabetes Surveillance & Care. Diabetes Technology & Therapeutics (DT&T) 2006;8:587-597. ![]()
7. Parker VER, Simmons D. Diabetes Information Technology in UK diabetes secondary care: A snapshot. British Journal of Diabetes and Vascular Disease 2013;13:150-154. ![]()
8. Wu RC, Straus SE. Evidence for handheld electronic medical records in improving care: a systematic review. BMC Med Inform Decis Mak. 2006 Jun 20;6:26. ![]()
9. Free C, Phillips G, Galli L, Watson L, Felix L, Edwards P, et al. The Effectiveness of Mobile-Health Technology-Based Health Behaviour Change or Disease Management Interventions for Health Care Consumers: A Systematic Review. PLoS Med 2013; 10(1): e1001362. doi:10.1371/journal.pmed.1001362 ![]()
10. Jelsma JG, van Poppel MN, Galjaard S, Desoye G, Corcoy R, Devlieger R, van Assche A, Timmerman D, Jans G, Harreiter J, Kautzky-Willer A, Damm P, Mathiesen ER, Jensen DM, Andersen L, Dunne F, Lapolla A, Di Cianni G, Bertolotto A, Wender-Oegowska E, Zawiejska A, Blumska K, Hill D, Rebollo P, Snoek FJ, Simmons D. DALI: Vitamin D and lifestyle intervention for gestational diabetes mellitus (GDM) prevention: an European multicentre, randomised trial –study protocol. BMC Pregnancy Childbirth 2013;13:142. ![]()
11. Simmons D, Jelsma JG, Galjaard S, van Assche A, Jans G, Corcoy R, Adelantado JM, Dunne F, Desoye G, Harreiter J, Kautzky-Willer A, Damm P, Mathiesen ER, Jensen DM, Andersen LL, Lapolla A, Dalfra M, Bertolotto A, Wender-Ozegowska E, Zawiejska A, Hill D, Rebollo P, Snoek FJ, van Poppel MN. Results From a European Multicenter Randomized Trial of Physical Activity and/or Healthy Eating to Reduce the Risk of Gestational Diabetes Mellitus: The DALI Lifestyle Pilot. Diabetes Care 2015;38:1650-6. ![]()
12. Simmons D et al. Effect of physical activity and/or healthy eating on GDM risk: The DALI Lifestyle Study. J Clin Endo Metab 2016. DOI: 10.1210/jc.2016-3455 ![]()
13. Simmons D, Rush E, Crook N. Development and piloting of a community health worker based intervention for the prevention of diabetes among New Zealand Maori in Te Wai o Rona: Diabetes Prevention Strategy. Public Health Nutr 2008;11:1318-25. ![]()
14. Simmons, D. Prevention of gestational diabetes mellitus: Where are we now? Diabetes Obes Metab 2015;17:824-34. ![]()
15. World Health Organization. Diagnostic Criteria and Classification of Hyperglycaemia First Detected in Pregnancy. WHO/NMH/MND/13.2. Geneva: World Health Organization; 2013.
16. Kao C, Liebovitz. Consumer Mobile Health Apps: Current state, barriers and future directions. PM&R 2017;9:S106-115. ![]()
17. Nielsen, J. (1994). Usability engineering. Morgan Kaufmann Publications.
18. Harrison R, Flood D, Duce D. Usability of mobile applications: literature review and rationale for a new usability model. Journal of Interaction Science 2013;1:1 ![]()
19. Kortum P, Sorber M. Measuring the Usability of Mobile Applications for Phones and Tablets. Intl. Journal of Human–Computer Interaction 2015; 31:518–529. ![]()
Appendix
The DALI core investigators group
G. Desoye4, D. Simmons3, R. Corcoy5,6, J.M. Adelantado5, R. Devlieger7, A. van Assche7, P. Damm8, E.R. Mathiesen8, D.M. Jensen9, L.L. Andersen9, A. Lapolla10, MG. Dalfrà10, A Bertolotto11,12, E. Wender-Ozegowska12, A. Zawiejska12, D. Hill13, F.J. Snoek15, M.N.M. van Poppel14, A. Kautzky-Willer2 FP. Dunne1
Gernot Desoye, PhD.4 Department of Obstetrics and Gynecology, Medizinische Universitaet Graz, Graz, Austria. E: gernot.desoye@medunigraz.at
David Simmons, MD (Cantab)3 Institute of Metabolic Science, Addenbrookes Hospital, Cambridge, England and Macarthur Clinical School, Western Sydney University, Sydney, Australia. E: Da.simmons@westernsydney.edu.au
Rosa Corcoy, PhD.4 Department of Obstetrics and Gynecology, Medizinische Universitaet Graz, Graz, Austria.5 Institut de Recerca de l´Hospital de la Santa Creu i Sant Pau, Barcelona, Spain. E: RCorcoy@santpau.cat
Juan M Adelantado, PhD5 Institut de Recerca de l´Hospital de la Santa Creu i Sant Pau, Barcelona, Spain.6 CIBER Bioengineering, Biomaterials and Nanotechnology, Instituto de Salud Carlos III, Zaragoza, Spain. E: JAdelantado@santpau.cat
Roland Devlieger, PhD7 KU Leuven Department of Development and Regeneration: Pregnancy, Fetus and Neonate. Gynaecology and Obstetrics, University Hospitals Leuven, Belgium. E: roland.devlieger@uzleuven.be
Andre van Assche, PhD7 KU Leuven Department of Development and Regeneration: Pregnancy, Fetus and Neonate. Gynaecology and Obstetrics, University Hospitals Leuven, Belgium. E: andre.vanassche@med.kuleuven.be
Peter Damm, DMsc.8 Center for Pregnant Women with Diabetes, Departments of Endocrinology and Obstetrics, Rigshospitalet, Institute of Clinical Medicine, Faculty of Health and Medical Sciences, University of Copenhagen, Copenhagen, Denmark. E: pdamm@dadlnet.dk
Elizabeth Rheinhardt Mathiesen, DMsc.8 Center for Pregnant Women with Diabetes, Departments of Endocrinology and Obstetrics, Rigshospitalet, Institute of Clinical Medicine, Faculty of Health and Medical Sciences, University of Copenhagen, Copenhagen, Denmark. E: elisabeth.reinhardt.mathiesen@regionh.dk
Dorte Moeller Jensen, PhD.9 Department of Endocrinology and Department of Gynaecology and Obstetrics, Odense University Hospital, Department of Clinical Research, Faculty of Health Science, University of Southern Denmark, Odense, Denmark. E: Dorte.Moeller.Jensen@rsyd.dk
Lise Lotte T. Anderson, MD.9 Department of Endocrinology and Department of Gynaecology and Obstetrics, Odense University Hospital, Department of Clinical Research, Faculty of Health Science, University of Southern Denmark, Odense, Denmark. E: lise.lotte.andersen@rsyd.dk
Annunziata Lapolla, MD.10 DPT Medicine, Universita Degli Studi di Padova, Padua, Italy. E: annunziata.lapolla@unipd.it
Maria G Dalfrà, MD.10 DPT Medicine, Universita Degli Studi di Padova, Padua, Italy. E: u053734@sanita.padova.it
Alessandra Bertolotto, PhD.11 Azienda Ospedaliero-Universitaria Pisana, Pisa, Italy. E: alessandrabertolotto1959@yahoo.it
Ewa Wender-Ozegowska, PhD.12 Medical Faculty I, Poznan University of Medical Sciences, Poznan, Poland. E: ewaoz@post.pl
Agnieszka Zawiejska, PhD12 Medical Faculty I, Poznan University of Medical Sciences, Poznan, Poland. E: agazaw@post.home.pl
David Hill, DPhil.4 Recherche en Santé Lawson SA, St. Gallen, Switzerland. E: davidhill473@gmail.com
Frank J Snoek, PhD.15 Department of Medical Psychology, EMGO+-Institute for Health and Care Research, VU University Medical Centre and Medical Psychology AMC, Amsterdam, the Netherlands. E: fj.snoek@vumc.nl
Mireille N.M. van Poppel, PhD.14 Department of Public and Occupational Health, EMGO+-Institute for Health and Care Research, VU University Medical Centre, Amsterdam, the Netherlands. E: mnm.vanpoppel@vumc.nl
Alexandra Kautzky-Willer, MD.2 Gender Medicine Unit, Division of Endocrinology and Metabolism, Department of Medicine III, Medical University of Vienna, Vienna, Austria. E: alexandra.kautzky-willer@meduniwien.ac.at
Fidelma Dunne, PhD.1 National University of Ireland, Galway, Ireland. E: fidelma.dunne@nuigalway.ie

