Google Glass Indirect Ophthalmoscopy
Aaron Wang, MD, PhD1, Alex Christoff, CO, COT1, David L. Guyton, MD1, Michael X. Repka, MD1, Mahsa Rezaei, MS1, Allen O. Eghrari, MD1
1Department of Ophthalmology, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA
Corresponding Author: allen@jhmi.edu
Journal MTM 4:1:15–19, 2015
Background: Google Glass is a wearable, head-mounted computer with display, photographic and videographic imaging capability, and connectivity to other devices through Wi-Fi and Bluetooth signaling.
Aims: To describe for the first time the use of Google Glass for use in indirect ophthalmoscopy and modification techniques to assist with its use.
Methods: A lightweight, portable light source was installed above the Glass aperture, a small tissue paper used to diffuse the light, and the arm of the headset was taped to the examiner’s glasses in order to bring the display into the right eye’s central visual field.
Results: Using a slightly modified Glass headset, the examiner documented the central and peripheral retina in a young male with ease.
Conclusion: We demonstrate for the first time that Glass, with minor modifications, can be used as a simple and effective method to perform and record a fundus examination.
Introduction
In April 2013, Google released a beta version of the Google Glass for developers for $1500, termed the Explorer version. Glass is a wearable headset weighing 50 grams with a prismatic heads-up color display in the superior visual field of the right eye. It includes a built-in 5 megapixel camera with 1280 x 720 pixel HD video at 30 frames per second ambient light sensor, Wi-fi and Bluetooth connectivity, a capacitive touchpad on the temple frame, 16GB of flash memory, and is powered by a 2.1 Watt-hour lithium polymer battery. Among the earliest adopters of this wearable technology were physicians, who quickly integrated this tool into medical and surgical practice.1
In health care, the application of the Glass has largely centered on the ability to access patient-specific medical records in a convenient manner. Reports of its use to display radiographic images by the bedside or intraoperatively,2 allergy information in an emergency medicine setting,3 or medical records by facial recognition,4 demonstrate the unique utility of this commercially available head-mounted tool to present physicians with needed information quickly and effectively. Patient privacy has been addressed by customization of the Glass to shut off social media sharing.5
The use of imaging through Glass for health delivery has been particularly relevant for surgery. Advantages include its head mounted, hands-free use6 and the ability to allow other physicians and observers to view surgical techniques from the visual perspective of the surgeon.7,8
To our understanding, however, the use of Glass for imaging of fine details or microscopy in vivo has not been explored. This may be due in part to the lack of manual controls in image acquisition and the inability to zoom, as well as the superiorly displaced display over the right eye visual field, which may cause symptoms of strain9 for the user and prevent comfortable real-time imaging. In contrast to most current-generation smartphones, the Glass also does not have an illuminating light source, and therefore no flash photography.
Here, we describe for the first time the use of the Glass to acquire images of the retina. Through simple, affordable modifications of the commercially available headset, “Glass indirect ophthalmoscopy” can assist with disease management and education.
Methods
Minimal modification of Glass is necessary for use in indirect ophthalmoscopy, as the headset already includes an onboard camera and display. We affixed an external light source, small enough to be attached securely to the device, on top of the aperture, as the standard indirect binocular ophthalmoscopes with which ophthalmologists are accustomed include a light source above the viewing optics. The orientation of the light with respect to the viewing optics, or in this case, the Glass’s camera aperture, affects the character of the glare and reflections for the condensing lens and cornea. Affixing the light source above the aperture preserves the familiar movements of the user’s head and tilting of the condensing lens to optimize fundus viewing and minimize glare and reflections. The light itself needs to be bright enough to view the fundus, but not too bright that it overwhelms the autoexposure capability of the Glass. It should be battery operated to prevent the need for additional power or obtrusive wiring.
After utilizing several portable LED lights of various shapes and sizes, we identified a small keychain LED light from http://meritline.com (SKU 600-773-001) to be particularly useful, as its switch allows the light to be continually powered. To create a soft diffuse light, we attached a small piece of tissue paper in front of the LED. The light was then affixed to the Glass with Velcro. This allows the position of the light to be easily adjusted to ensure that the direction of the light is the same as that of the aperture. This apparatus is demonstrated in Figure 1.

Figure 1: Google Glass with LED lighting apparatus fixed directly superior to aperture. During use, tissue paper is placed in front of the light for diffusion.
The exam of the fundus is performed by viewing the onboard display only, while the Glass is viewing the aerial image of the condensing lens. This technique ensures that what is seen is what is captured. In its current form, the user starts video capture, taps the Glass arm to extend the length of the video, and taps to stop the recording after the exam. Although the default assembly of the Glass requires the examiner to direct gaze superotemporally, for Glass Indirect ophthalmoscopy the user should position the display centrally, to be in primary gaze for extended comfortable viewing with the Glass for the duration of the exam. This is accomplished by unscrewing the Google Glass frame from the main unit and taping it to the frame of the user’s own glasses (see Figure 2), or a blank pair.

Figure 2: The Google Glass unit is attached to the user’s own glasses with tape around the arm, allowing the display to be positioned directly in the center of the user’s field of view.
To perform the exam, the light is toggled on and the video capture is started. The exam is then performed in the same manner as with the traditional binocular indirect ophthalmoscope (BIO) by holding the condensing lens in one hand. Since the camera application for the Glass currently is wide angle and zooming options are not currently present, the fundus will appear small in the display. To address this issue, the examiner should position his or her head about 25cm (rather than arm’s length) from the patient’s eye so that the fundus can fill the field of view of the Glass camera. This represents the only change in examination technique that differs from use of the traditional BIO, and is demonstrated in Figure 3.
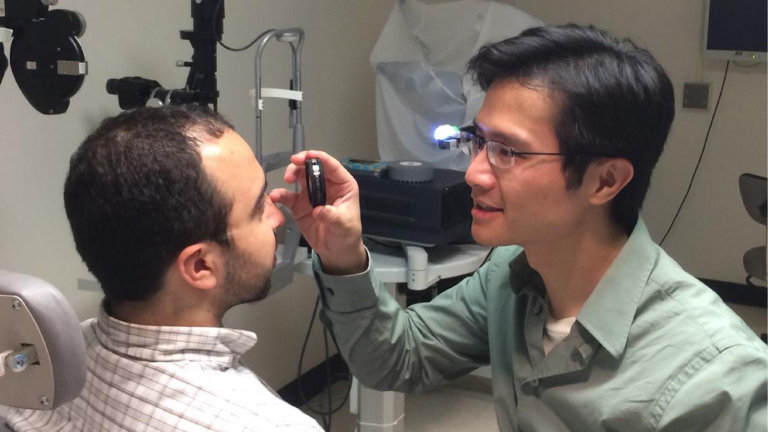
Figure 3: The examiner uses Glass on a subject for fundoscopy at a relatively close distance, positioned between the typical near (direct ophthalmoscopy) and far (indirect ophthalmoscopy) locations encountered with standard techniques.
After discussion of risks and benefits, a 31-year-old male volunteer provided informed consent to proceed with Glass indirect ophthalmoscopy and recording, as part of a study of head-mounted digital camera indirect ophthalmoscopy for which Institutional Research Board approval was obtained. The participant’s right eye was dilated with 2.5% phenylephrine and 1% tropicamide.
All authors have completed the Unified Competing Interest form at www.icmje.org/coi_disclosure.pdf and declare: no support from any organisation for the submitted work; no financial relationships with any organisations that might have an interest in the submitted work in the previous 3 years; no other relationships or activities that could appear to have influenced the submitted work.
Results
With the appropriate external light fixated in the manner described above, and the shorter examination distance, the user can obtain fundus examination and video recording using the Google Glass. The learning time to use such an apparatus is minimal. Video 1 demonstrates the ease of examination, and simplicity of marching around the periphery of the fundus. Still photographs from the center and periphery are demonstrated in Figure 4.

Figure 4: Still photographs from Video 1 reveal an image of the disc, macula, choroidal vasculature and vitreoretinal interface centrally (left). Glass may also be oriented to acquire images of the retinal periphery; details of a single peripheral retinal vessel are appreciated inferiorly (right). We expect resolution of Glass imaging to improve in future iterations.
The quality of viewing is based on the resolution of the display, and the quality of the video capture is based on the camera; both of which will only improve with time. Currently, the resolution of the display and camera are sufficient to obtain a good fundus exam. Auto-exposure and autofocusing was rapid enough to not hinder the speed of the exam.

Video 1: Video of Glass reveals ease of fundoscopy. Details of the optic nerve, macula, vessels, and peripheral pigmentary changes are all recognized through this view.
Discussion
The use of mobile technology in daily ophthalmic practice is widespread, and the vast majority of ophthalmologists have integrated the use of smartphones into their professional responsibilities.9
To date, portable digital fundoscopy has been largely smartphone-based. This includes the iExaminer (WelchAllyn, Skaneateles Falls, NY, USA) which pairs with a panoptic ophthalmoscope, and PEEK (Peek Vision). In contrast to these options, Glass indirect ophthalmoscopy allows the practitioner to maneuver the photographic unit with the head, utilizing the familiar technique of indirect ophthalmoscopy, and providing a view of the peripheral retina.
Although the resolution of cameras associated with popular commercially available mobile devices is often less than slit-lamp mounted digital SLR cameras, image quality is adequate for documentation of gross and, with proper magnification, fine features of the retina. A direct head-to-head diagnostic comparison of images from digital SLR vs. smartphone photography in a dermatological setting demonstrated that a difference in resolution, although noticeable, does not necessarily translate to clinical utility.11 For instance, the RetCam (Clarity Medical Systems, Pleasanton, California, USA), widely used for retinal imaging under anesthesia, produces 640 x 480 images; our institution has found it useful clinically despite the fact that alternative fundus imaging systems Panoramic 200 (Optos, Fife, Scotland) and Optooret-1000 (Medibell Medical VIsion Technologies, Haifa, Israel) have higher resolutions (2000 x 2000 and 1024 x 1024, respectively). In comparison, the Glass demonstrates relatively high resolution, increased portability, and a price two orders of magnitude less.
This balance of portability and digital video or photographic documentation may open new avenues for clinical care and education. A physician, for instance, may find it helpful to document examination findings seen through Glass for integration into electronic medical records. Similar to operating rooms in which medical students may view surgery on a screen through the perspective of the operating microscope, students learning the details of indirect ophthalmoscopy may find it beneficial to view the retina from the perspective of the examiner. In rural settings or in developing countries, a portable battery could be used to charge the Glass through its USB connection and the LED-powered light source is independent in its battery life from the Glass itself. An additional advantage in such settings is the ability to record audio narration while examining patients, and the possibility of geotagging photographs based on GPS/spatial and temporal coordinates during rural camps. Further development of the Glass device, its operating system, storage, and imaging capabilities will facilitate its use in a variety of settings.
The indirect ophthalmoscopic exam method is preserved except for the examination distance. Although a telephoto lens in front of the aperture may preserve the examination distance, adapting to a closer viewing distance is not impractical, as it requires the head to be positioned between what would be generally utilized for direct and indirect ophthalmoscopy. Also, as applications on the Glass develop, it is likely that a zoom feature will be incorporated into the video application to allow for traditional arm’s length working distance, enabling the Glass to be used through smaller pupils. Applications could be developed for the Glass to enhance video ophthalmoscopy and its use in medicine.
Conclusion
In summary, we describe the use of Google’s Glass device for indirect ophthalmoscopy and documentation of the optic nerve, macula and peripheral retina. Its portability, affordability relative to other retinal imaging techniques, and ease of use allows it to be applied in a variety of clinical and research settings.
Acknowledgements
The authors wish to thank Jessica Chang and Sonya Thomas for photographic support.
References
1. Eng, J. British doctor livestreams cancer surgery using google glass. NBC News May 23 2014. http://www.nbcnews.com/science/science-news/british-doctor-livestreams-cancer-surgery-using-google-glass-n113596 (Accessed on June 15, 2014).
2. Kim, L. Google glasss delivers new insight during surgery. UCSF October 13 2013. http://www.ucsf.edu/news/2013/10/109526/surgeon-improves-safety-efficiency-operating-room-google-glass (Accessed on June 15, 2014).
3. Borchers, C. Google glass embraced at Beth Israel Deaconess. Boston Globe April 4 2014. http://www.bostonglobe.com/business/2014/04/08/beth-israel-use-google-glass-throughout-emergency-room/WhIXcVzkpn7MOCAhKuRJZL/story.html (Accessed on June 15, 2014)
4. MedRef : https://medrefglass.appspot.com (Accessed on June 15, 2014).
5. Pai, A. At least four startups are now focused on Google Glass apps for doctors. Mobihealthnews April 17 2014. http://mobihealthnews.com/32170/at-least-four-startups-are-now-focused-on-google-glass-apps-for-doctors/ (Accessed June 15, 2014).
6. Muensterer OJ, Lacher M, Zoeller C, Bronstein M, Kubler J. Google glass in pediatric surgery: an exploratory study. Int J Surg. 2014; 12(4): 281–289.
7. O’Conner, A. Google glass enters the operating room. The New York Times June 1 2014. http://mobile.nytimes.com/blogs/well/2014/06/01/google-glass-enters-the-operating-room Accessed on June 15, 2014).
8. Lutz B, Kwan N. Chicago Surgeon to use google glass in operating room. NBC Chicago Dec 26 2013. http://www.nbcchicago.com/news/tech/google-glass-surgery-237305531.html (Accessed on June 15, 2014).
9. Smith, J. Google’s eye doctor admits glass can cause pain. Betabeat May 19 2014 http://betabeat.com/2014/05/googles-eye-doctor-admits-glass-can-cause-pain/ (Accessed on June 15, 2014).
10. Davis EA, Hovanesian JA, Katz JA, Kraff MC, Trattler WB. Professional Life and the Smartphone. Cataract Refract Surg Today. 2010 Sep 21–2.
11. Asaid R, Boyce G, Padmasekara G. Use of smartphone for monitoring dermatological lesions compared to clinical phothography. Journal of Mobile Technology in Medicine. 2012; 1(1) 016–8.

