Cell phone access among persons who inject drugs in Tijuana, BC, Mexico.
Kelly M. Collins1,2, Daniela Abramovitz1, Meredith C. Meacham1,2, Patricia E. Gonzalez-Zuniga1, Kevin Patrick3,4, Richard S. Garfein1
1Division of Global Public Health, Department of Medicine, School of Medicine, University of California, San Diego, La Jolla, CA, USA; 2Graduate School of Public Health, San Diego State University, San Diego, CA, USA; 3Department of Family and Preventive Medicine, University of California, San Diego, La Jolla, CA, USA; 4CALIT2, University of California, San Diego, La Jolla, CA, USA
Corresponding author: rgarfein@ucsd.edu
Journal MTM 4:3:13–19, 2015
Background: Persons who inject drugs (PWID) are at high risk for hepatitis C virus (HCV) and human immunodeficiency virus (HIV) infection, particularly in Tijuana, Baja California, Mexico, where HCV prevalence among PWID is above 95%. PWID also demonstrate low access and use of health services. mHealth intervention tools may prove effective for reducing disease risk and increasing access to health services for PWID. However, knowledge of cell phone access within this population is needed before designing such interventions.
Methods: We aimed to determine the prevalence and correlates of cell phone access among PWID enrolled in the ‘El Cuete’ cohort study in Tijuana. Participants were asked for detailed contact information at baseline—including a cell phone number if available—to facilitate retention. Interviews obtained socio-demographic data, health information, and lifetime/recent drug and sexual risk behaviors. Logistic regression was used to assess factors independently associated with providing a cell phone number.
Results: Of 735 participants enrolled, 16% of participants had access to a cell phone at baseline. Mean age was 37 years old, ranging from 18–63. Sixty two percent of participants were male, 96% were Hispanic, and 27% reported recent homelessness. Higher education and a monthly income≥2500 pesos were associated with higher odds of cell phone access. Inversely, homelessness, daily injection drug use, and older age were associated with lower odds of cell phone access.
Conclusions: Cell phone access among PWID in Tijuana is low and should be considered in the design of mHealth interventions targeting this population.
Introduction
Risky injection practices, such as sharing of needles and injection paraphernalia, put persons who inject drugs (PWID) at high risk for hepatitis C virus (HCV) and human immunodeficiency virus (HIV) infection.1 In a 2008 cross-sectional study of 1056 PWID in Tijuana, Baja California, Mexico, 59% of participants reported lifetime receptive needle sharing.2 Similarly, a 2010 cross-sectional study of 510 PWID in San Diego, CA, found that 49% of participants receptively shared needles and 68% shared injection paraphernalia.3 In addition to engaging in risky behaviors, PWID are at high risk for loss-to-follow-up for treatment adherence4 and demonstrate low access to and use of health care services.5
Tijuana is thought to have approximately 10,000 injection drug users, with a high prevalence of heavy drug use in the Zona Norte colonia, or neighborhood, close to the U.S.—Mexico Border.6 The Zona Norte is home to the largest red-light district (e.g., zona roja) in North America, known for its brothels, street prostitution, and illicit drug sales.7 In addition, HIV and HCV rates among PWID living in Tijuana are approximately 4% and 95% respectively.2,8 Successful treatment and prevention approaches for HIV and HCV require strict adherence to medication regimens and continuity in care, as well as significant reductions in risk behaviors to prevent the spread of infection to others.
mHealth—the use of mobile and wireless devices to improve health outcomes, health care services, and health research9—may offer some promise for reducing risk and increasing engagement in health care for PWID. mHealth intervention strategies have proved effective in non-substance using populations to improve self-management of diabetes,10 increase physical activity,11 improve medication adherence,12 and decrease smoking.13 These strategies have also been used successfully in research among vulnerable populations, including providing support for those participating in addictions treatment,14 reducing sexually transmitted infection (STI) among female sex workers,15 and improving HIV anti-retroviral therapy (ART) adherence among non-injection substance users.12,16
To assess technology access and use among high-risk individuals, one study of substance users enrolled in drug treatment in Baltimore reported that 91% of participants had access to a cell phone and 79% to text messaging.17 Another study among homeless youth in Los Angeles, of which 55% used a substance in the past 30 days, reported 62% of respondents owning a cell phone.18 However, less is known about mHealth strategies to improve health outcomes among PWID specifically. One small study assessing ART adherence among HIV-positive PWID in China suggests that although participants found mHealth tools acceptable, privacy and confidentiality were of the utmost concern.19 Another study among PWID in Sweden, found that mobile phones were a successful tool for communication and prospective follow-up among PWID who owned a mobile device.20
To successfully implement mHealth interventions among PWID, it is first necessary to know what proportion are already using cell phones in this population. Thus, we assessed the prevalence and correlates of cell phone access among PWID enrolled in a longitudinal cohort study of HIV risk behaviors in Tijuana. The results of this analysis will be valuable for informing the development and implementation of mHealth interventions among PWID.
Methods
Study Population and Eligibility
“Proyecto El Cuete IV” is a prospective longitudinal cohort study of 735 PWID in Tijuana; detailed study methods are described elsewhere.21 At baseline, participants completed a behavioral risk assessment interview and serologic testing for HIV. Baseline enrollment was completed from 2011 to 2012; semi-annual follow-up visits are ongoing. Baseline quantitative study instruments assessed lifetime and recent drug use and risk behaviors.21 Eligibility criteria included the following: 1) being at least 18 years of age, 2) having evidence of injecting illicit drugs within the past month confirmed by observation of track marks or other physical evidence of injecting, 3) being able to converse in English or Spanish, 4) currently residing in Tijuana with no plans to move away within 24 months from enrollment date, and 5) not currently participating in any intervention studies. Individuals with severe cognitive deficiencies who were unable, or those who were unwilling to provide informed consent were excluded. Individuals who were too intoxicated or sleepy to provide consent and complete the study procedures were asked to return at a later date. The Human Research Protections Program of the University of California San Diego and the Institutional Review Board at the Colegio de la Frontera Norte (COLEF) approved all study procedures.
Recruitment
Recruitment involved targeted street-based outreach. Outreach teams established temporary mobile recruitment sites (such as vans and tents) in ten different colonias around Tijuana. Recruitment was also conducted out of the El Cuete field office located in the Zona Norte.
Data Collection
After participants were screened for eligibility and provided informed consent, trained bilingual research assistants conducted behavioral risk as-sessment interviews in English or Spanish in a confidential setting. Interviews were administered using computer-assisted personal interviewing (CAPI) technology, which has been used previously for studies in Mexico and the United States.21 Instruments at baseline assessed lifetime and recent experiences and behaviors. To facilitate study retention, detailed locator information, including cell phone number if available, was collected at baseline and updated at subsequent visits. Since the validity of findings from this longitudinal study depended on achieving high retention rates, interviewers made every effort to obtain all possible forms of contact, including cell phone numbers.
Measures
Socio-demographic measures included race/ethnicity, place of birth, education, language proficiency, citizenship and immigration status, marital status, living situation, incarceration, and reporting a landline phone number when asked for contact information. Drug use behaviors included lifetime and recent use of specific drugs, including drug of choice and frequency of injection, and sharing of syringes and/or other drug-related paraphernalia. Drug treatment and harm reduction measures included lifetime and recent experiences with voluntary and court-mandated drug treatment (e.g., methadone, outpatient vs. residential drug treatment, self-help groups), syringe exchange program (SEP) use, and obtaining syringes from a pharmacy or another safe source. Sexual risk behaviors included exchanging sex for money or other material goods. Other measures included history of prior HIV diagnosis and study retention at six months.
Data Analysis
The outcome measure for this analysis was whether or not the participant had access to a cell phone, which was assessed by whether or not s/he provided a cell phone number at baseline (yes/no). Descriptive statistics of the socio-demographic and risk behavior variables were calculated for each of the two cell phone groups. Frequencies were calculated for the binary variables, whereas means and standard deviations were calculated for continuous variables. A bivariate analysis was conducted to assess unadjusted associations with our outcome. Variables with a p≤ 0.10 in bivariate analysis were considered for inclusion multivariable models. Manual stepwise logistic regression was used to build these models, and variables with p≤ 0.05 were retained in the final model to determine odds ratios and 95% confidence limits for correlates of cell phone access. Confounding was assessed by determining significant changes (>10%) in crude associations, and maintaining confounding variables in the final model. Multi-collinearity was assessed using variance inflation factors (VIF), and models were compared using likelihood ratio tests. All analyses were performed with SAS version 9.3 (SAS, Cary, NC).
Results
Sample Characteristics
All participants who were enrolled in El Cuete IV (n = 735) were included in this analysis. One hundred and seventeen participants (16%) had access to a cell phone at baseline (Table 1). Overall, the mean age was 37 years old, ranging from 18–63. Sixty two percent of participants were male and 96% were Hispanic. Twenty-seven percent reported being mostly homeless in the past six months; 59% reported ever having lived in the United States, 49% had an average monthly income above 2500 Pesos (~$200 USD), and participants reported a mean of eight years of education. Twenty-six participants (3.5%) tested HIV-positive at baseline.
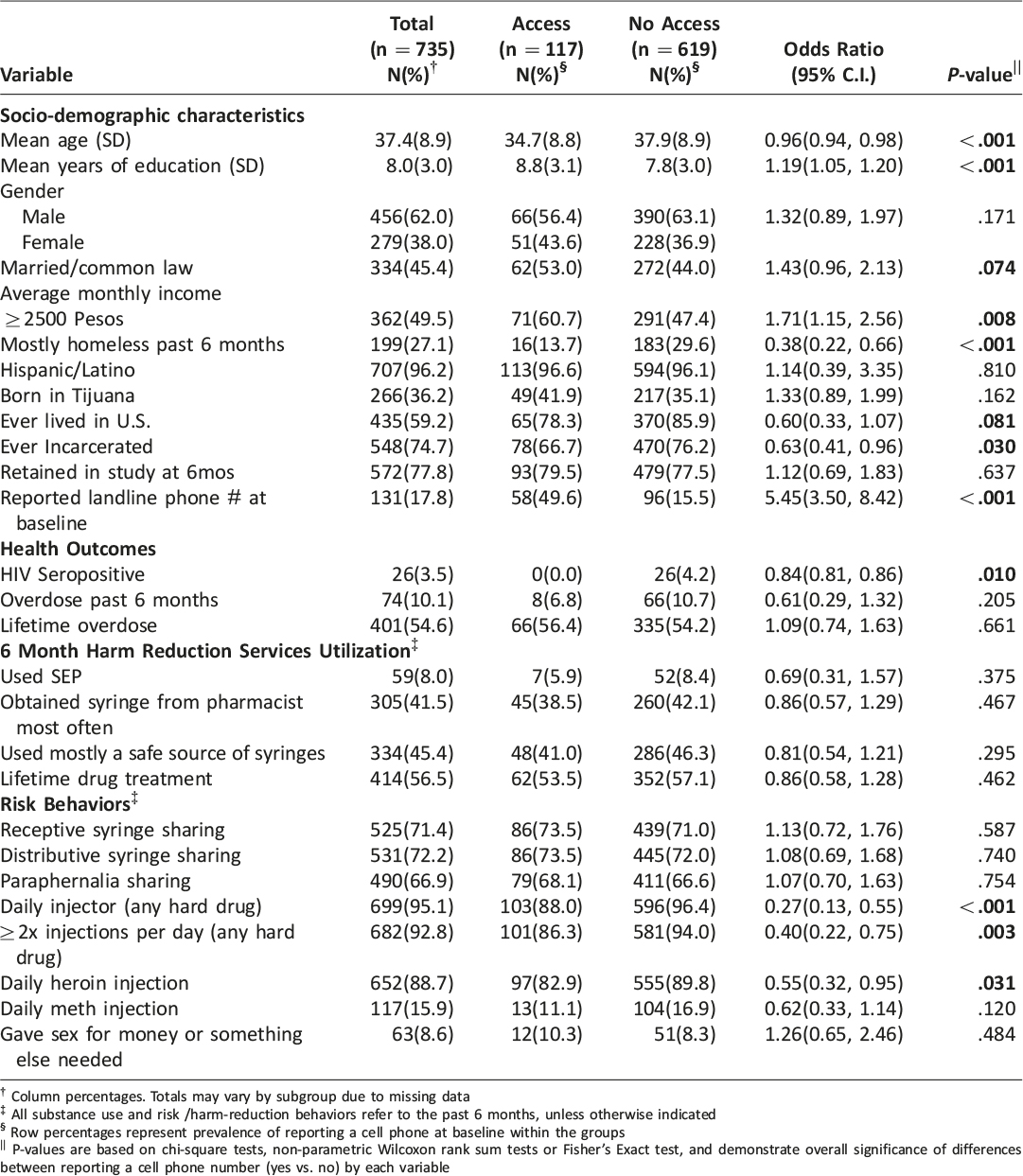
Table 1: Bivariate analysis of socio-demographic characteristics, health outcomes and substance risk and harm reduction behaviors by cell phone access among people who inject drugs, Tijuana, BC, Mexico, 2011–2012.
Prevalence and Correlates of Cell Phone Access
In bivariate analysis, (Table 1) cell phone access was positively associated with more years of education, having an average monthly income ≥2500 Pesos, and reporting a landline phone number. Self-reported homelessness in the past 6 months, lifetime incarceration, HIV seropositivity, daily heroin injection, daily injection of any hard drug, and injecting more than once per day with any hard drug were inversely associated with cell phone access. Lastly, for every ten-year increase in age there was a 40% decrease in the likelihood of cell phone access (i.e., 4% per year). All p-values for significant differences were less than 0.05.
While self reported homelessness and reporting a landline phone number were both significant in bivariate analyses, these variables were highly co-linear and could not be retained in the same multivariable model. Thus, the authors elected to retain homelessness in this analysis due to its importance as a risk factor among PWID. In the final multivariable model (Table 2), homelessness (Adjusted Odds Ratio [AOR]= 0.44, 95% Confidence Interval [CI]= 0.25, 0.77), daily injection drug use (AOR= 0.34, 95% CI= 0.16, 0.71) and age (AOR= 0.96 per year, 95% CI= 0.93, 0.98) were independently associated with lower odds of cell phone access; whereas years of education (AOR= 1.11 per year, 95% CI= 1.02, 1.18), and having average monthly income ≥2500 pesos (AOR= 1.51, 95% CI= 0.99, 2.31) were associated with higher odds of cell phone access.
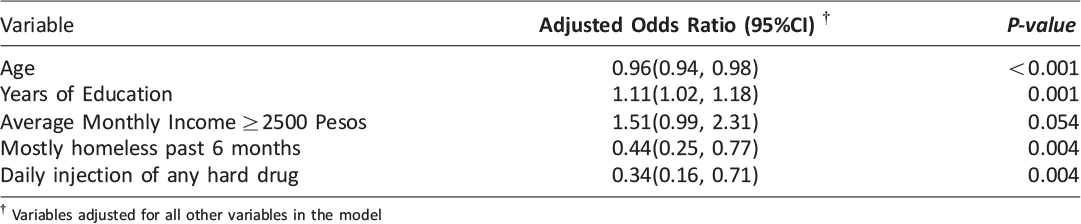
Table 2: Multivariable logistic regression analysis of factors associated with cell phone access among people who inject drugs, Tijuana, BC, Mexico, 2011–2012.
Discussion
Overall, a low percentage (16%) of this cohort of PWID living in Tijuana had access to a cell phone. In comparison, the Mexican National Census estimated that two-thirds (67%) of Mexicans owned a cell phone in 2010.22 Cell phone use throughout Mexico has since risen, with 87% of Mexicans estimated to have access to a cell phone in 2013.23 However, Tijuana is thought to have a higher percentage of PWID than any Mexican state—PWID in Tijuana are generally lower SES and more likely to be socially marginalized individuals.2 This could partially account for the low cell phone coverage among the El Cuete study population.
Younger age was associated with cell phone access in this study, which is consistent with trends in the general Mexican population.24,25 Additionally, participants with higher SES (e.g., more education and higher monthly income) were more likely to have access to a cell phone, consistent with international polling about the growing use of technology in global emerging economies including Mexico.24,25 Marginalized participants, including individuals who were poorer, homeless, and those engaging in daily injection practices, were significantly less likely to have access to a cell phone. Given their marginalized status, these participants may also have less access to the resources required for owning and maintaining a cell phone, and thus less likely to report cell phone access to study staff. Researchers will need to consider cell phone coverage when developing mHealth intervention studies among PWID in Tijuana, because a high percentage of this population will be similarly resource-deprived.2
It was notable that none of the HIV seropositive participants reported a cell phone number to study staff. However, the low HIV prevalence in the study population may have precluded a significant finding for this variable in the final model. Landline use in Mexico has fallen below 50% in recent years22 and access to a phone, whether it’s a landline or a cell phone, is important for a population such as this to stay in contact with health care providers. These individuals may have elected not to share this type of contact information due to stigmatization or privacy concerns related to cell phone use and/or their HIV status. More research is needed to understand how HIV-positive PWID in Tijuana access appointments, communicate with their provider, and manage HIV treatment.
Some limitations should be considered when interpreting these findings. This study did not specifically ask participants if they owned or had access to a cell phone in the risk assessment interview. Instead, participants were asked to provide a cell phone number, if they had one, when providing locator information at the baseline and subsequent study visits. Participants may have owned or had access to a communal cell phone, but elected not to provide the number to study staff due to privacy concerns. This could potentially underestimate the proportion of participants who had access to a cell phone. Nonetheless, from the perspective of conducting research, willingness to provide a cell phone number to study staff is critical to implementing mHealth interventions. In addition, the baseline cross-sectional data used in this analysis do not permit temporal correlations between reporting a cell phone number and the other study variables. All risk behaviors were self-reported, which is subject to problems with recall. However, since the cell phone access variable was obtained from the participant contact form and was unrelated to the original study objectives, any problems with recall would be non-differential with regards to cell phone access and would tend to bias the results toward null findings.
Recall and social desirability bias may have resulted in an under-reporting of risk behaviors, and thus biased the associations between cell phone number reporting and correlates towards the null. However, a short recall period (six months for substance abuse and injection behavior questions) was used here to minimize bias. To minimize socially desirable responses, interviews were conducted in private settings with trained interviewers. Due to the convenience sampling used to recruit study participants for El Cuete Phase IV, these data might not be generalizable across all PWID in Tijuana. However, sampling and recruitment were designed to reach a variety of PWID across varying backgrounds and socioeconomic status. Despite these limitations, this research yields novel information regarding cell phone access among PWID, and identifies potential barriers to implementing mHealth research and interventions among PWID in the future.
Conclusions
mHealth interventions designed for PWID will need to consider levels of cell phone coverage for this low income, marginalized population. Only a small percentage of PWID in Tijuana provided a cell phone number when asked—the majority of participants either did not have access to a phone or were unwilling to share this information with El Cuete study staff. However, due to rapidly changing economic and societal norms, access to mobile technology is becoming ubiquitous across all levels of socioeconomic status, even in resource poor areas like Tijuana. More research may be needed among HIV-positive PWID to understand cell phone coverage among this population and determine how these individuals stay connected with care and any intervention research project staff. Future research should also assess smartphone ownership and/or mobile technology use in this population to better understand how mHealth tools may be utilized to implement interventions among PWID.
Acknowledgements
The authors would like to thank the field staff and all of the participants in Tijuana for making this research possible. The authors also acknowledge the thoughtful contributions of Dr. Tom Novotny, Dr. Camille Nebeker and Dr. Hector Lemus. This research was funded by the National Institutes of Health, grant numbers R37DA019829 and 2T32DA023356.
References
1. Strathdee SA, Hallett TB, Bobrova N, et al. HIV and risk environment for injecting drug users: the past, present, and future. Lancet. 2010;376:268–84. ![]()
2. Strathdee SA, Lozada R, Pollini RA, et al. Individual, social, and environmental influences associated with HIV infection among injection drug users in Tijuana, Mexico. J Acquir Immune Defic Syndr. 2008;47(3):369–76. ![]()
3. Garfein RS, Rondinelli A, Barnes RF, et al. HCV infection prevalence lower than expected among 18–40-year-old injection drug users in San Diego, CA. J Urban Health. 2013;90(3):516–28. ![]()
4. Arnsten JH, Xuan L, Mizuno Y, et al. Factors Associated With Anti retroviral Therapy Adherence and Medication Errors Among HIV-Infected Injection Drug Users. J Acquir Immune Defic Syndr. 2007;46(S2):S64–71. ![]()
5. Drumm RD, McBride DC, Metsch L, et al. ‘The Rock Always Comes First’: Drug Users’ Accounts About Using Formal Health Care. J Psychoactive Drugs. 2003;35(4):461–9. ![]()
6. Strathdee SA, Fraga WD, Case P, et al. Vivo para consumirla y la consumo papa vivir” [“I live to inject and inject to live”]: High Risk Injection Behaviors in Tijuana, Mexico. J Urban Health. 2005;82(4 Suppl):iv58–73.
7. Strathdee SA, Magis-Rodriguez C. Mexico’s evolving HIV epidemic. JAMA. 2008;300(5):571–3. ![]()
8. White EF, Garfein RS, Brouwer KC, et al. Prevalance of hematitic C virus and HIV infection among injection drug users in two Mexican cities bordering the U.S. Salud Publica Mex. 2007;49(2):165–72.
9. United States Department of Health and Human Services. 2010 [cited 2014 April 25]. Available from: http://www.hrsa.gov/healthit/mhealth.html.
10. Ribu L, Holmen H, Torbjornsen A, et al. Low-intensity self-management intervention for persons with type 2 diabetes using a mobile phone-based diabetes diary, with and without health counseling and motivational interviewing: protocol for a randomized controlled trial. JMIR Res Protoc. 2013;2(2):34. ![]()
11. Chomutare T, Fernandez-Luque L, Arsand E, et al. Features of mobile diabetes applications: review of the literature and analysis of current applications compared against evidence-based guidelines. J Med Internet Res. 2011;13(3):65. ![]()
12. Moore DJ, Montoya JL, Blackstone K, et al. Preliminary Evidence for Feasibility, Use, and Acceptability of Individualized Texting for Adherence Building for Antiretroviral Adherence and Substance Use Assessment among HIV-Infected Methamphetamine Users. AIDS Res Treat. 2013;2013:1–11. ![]()
13. Whittaker R, Maddison R, McRobbie H, et al. A multimedia mobile phone-based youth smoking cessation intervention: findings from content development and piloting studies. J Med Internet Res. 2008;10(5):49. ![]()
14. Epstein DH, Willner-Reid J, Vahabzadeh M, et al. Real-Time Electronic Diary Reports of Cue Exposure and Mood in the Hours Before Cocaine and Heroin Craving and Use. Arch Gen Psychiatry. 2009;66(1):88–94. ![]()
15. Roth AM, Hensel DJ, Fortenberry JD, et al. Feasibility and Acceptability of Cell Phone Diaries to Measure HIV Risk Behavior Among Female Sex Workers. Aids Behav. 2014;18(12):2314–24. ![]()
16. Ingersoll K, Dillingham R, Reynolds G, et al. Development of a personalized bidirectional text messaging tool for HIV adherence assessment and intervention among substance abusers. J Subst Abuse Treat. 2014;46(1):66–73. ![]()
17. McClure EA, Acquavita SP, Harding E, et al. Utilization of communication technology by patients enrolled in substance abuse treatment. Drug Alcohol Depend. 2013;129(1–2):145–50. ![]()
18. Rice E, Lee A, Taitt S. Cell phone use among homeless youth: potential for new health interventions and research. J Urban Health. 2011;88(6):1175–82. ![]()
19. Bachman Desilva M, Gifford AL, Keyi X, et al. Feasibility and Acceptability of a Real-Time Adherence Device among HIV-Positive IDU Patients in China. AIDS Res Treat. 2013;2013:1–6. ![]()
20. Hakansson A, Isendahl P, Wallin C, et al. Efficacy of mobile telephone contact for follow-up in injecting heroin users. Am J Drug Alcohol Abuse. 2011;37(2):89–92. ![]()
21. Robertson AM, Garfein RS, Wagner KD, et al. Evaluating the impact of Mexico’s drug policy reforms on people who inject drugs in Tijuana, B.C. Mexico, and San Diego, CA, United States: a binational mixed methods research agenda. Harm Reduct J. 2014;11(4):1–14.
22. T.W.J. Mexico’s census: TVs outnumber fridges. The Economist. 2011 April 28:2.
23. Lonergan K. Mexico telecoms sector expands 10% in Q2 2013. Available from: http://www.bnamericas.com/news/telecommunications/mexico-telecoms-sector-expands-10-in-q2.
24. Pew Global Attitudes Project. Global Digital Communication: Texting, Social Networking Popular Worldwide. 2011:1–30. http://www.pewglobal.org/2011/12/20/global-digital-communication-texting-social-networking-popular-worldwide/.
25. Pew Global Attitudes Project. Emerging Nations Embrace Internet, Mobile Technology; Cell Phones Nearly Ubiquitous in Many Countries. 2014.

