Medical Students’ Use of and Attitudes Towards Medical Applications
Dr Nicole Koehler PhD1, Dr Kaihan Yao MBBS2, Dr Olga Vujovic MBBS3,
Prof Christine McMenamin PhD1
1Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia, 2Medical Workforce Unit, Southern Health, Melbourne, Australia, 3Department of Infectious Diseases, The Alfred, Melbourne, Australia,
Corresponding Author: Nicole.Koehler@monash.edu
Journal MTM 1:4:16-21, 2012
DOI:10.7309/jmtm.73
Background/Aims: With the emergence of new technology (e.g., mobile device applications commonly known as “apps”) it is important to establish whether students have access to new technology and their attitudes towards its use prior to its implementation within a medical curriculum. The present study examined medical students’ ownership of mobile phones with application support (i.e., smartphones), and their use of and attitudes towards medical applications.
Methods: All Monash University medical students in 2011 were invited to complete an anonymous online survey regarding mobile phones and medical applications.
Results: A total of 594 medical students participated in the study. All students owned a mobile phone with 77% of them having a smartphone. Seventy-six per cent of students with smartphones used medical applications. Generally students had positive attitudes towards using medical applications. The majority of students with mobile phones without application support would be prepared to obtain such a device to enable them to access medical applications.
Conclusion: Given students’ positive attitudes toward medical applications; this study suggests that these devices could play a more significant role within medical education.
Introduction
Medical students have always relied heavily on textbooks for their education. However, with technological advances there is a shift towards medical students using electronic resources such as electronic textbooks1-3. This may change even further within the future given the relatively recent introduction of electronic devices such as smartphones.
Smartphones (e.g., Android, BlackBerry and iPhone) are powerful devices that combine the conventional functions of a mobile phone with advanced computing capabilities.4,5 Many healthcare professionals already use smartphones within their medical practice6 thus enabling them to replace multiple devices (e.g., pager, mobile phone and personal digital assistant) with one device7.
Recently there has been a meteoric rise in the popularity of smartphones, and consequently use of applications (commonly termed “apps”).4 Currently there are more than 10,000 apps within the Apple App Store’s “medical, health care & fitness” category8; with some of these being specifically designed for healthcare professionals such as medical calculators9,10 and medical reference tools11.
Medical apps can provide healthcare professionals with the ability to look up potential drug interactions7, perform medical calculations thus reducing the risk of error12, and study their patient’s radiological images13,14 without having to leave their patient’s bedside. Additionally, smartphones have enhanced communication between healthcare professionals. For example, healthcare professionals have used smartphones within the intensive care unit to inform each other in regards to the status of patients6.
The emergence of new technology, such as smartphones, is not restricted to clinical practice but has also made its way into medical courses. For example, personal digital assistants, which preceded smartphones, were owned by 65% of medical students at a Canadian university and were most commonly used to access drug references and clinical textbooks15. More recently, Wallace et al. reported that 85% of medical students at a Canadian university owned a smartphone and/or tablet, with 85% of them using the device daily for medical purposes and 77% of them regularly using at least one medical app16.
Although there is a shift towards electronic devices being used within medical education,15,16 at present little is known in regards to medical students’ smartphone ownership, use of medical apps, and their attitudes towards using these apps as part of their medical training within Australia. In other words, little is known as to whether medical students are ready for the use of medical apps to be implemented in the curriculum. Thus the aims of the present study were twofold: 1) to enumerate Monash University medical students’ mobile phone / smartphone ownership; and 2) to evaluate Monash University medical students’ attitudes towards using medical apps.
Methods
Participants
All medical students (N = 2,417) enrolled within Monash University’s five year undergraduate and four year graduate Bachelor of Medicine / Bachelor of Surgery (MBBS) degree, including those completing their Bachelor of Medical Science Honours year (an optional additional year to the MBBS), were invited to participate in the study during August 2011. Monash University is one of 18 accredited medical schools within Australia and in 2011 the total number of medical students enrolled at Monash represented 11% of all medical students within Australia during that year17.
Procedure
Ethics was obtained from Monash University’s Human Research Ethics Committee.
An anonymous online survey regarding medical students’ use and attitudes towards mobile phone apps as educational tools was created using Qualtrics (an online platform to administer surveys and collect responses). Students were alerted to the survey via a bulk email, an advertisement posted on Blackboard (a university-based online discussion board), and MBBS lecture announcements.
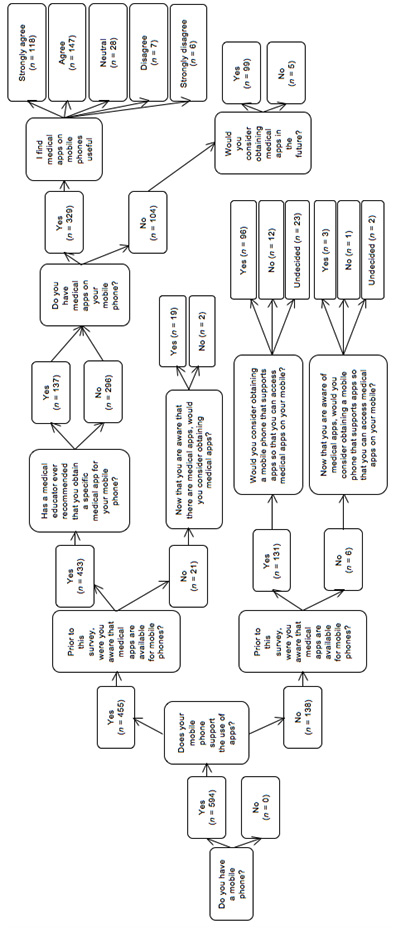
The survey comprised an algorithm such that participants were taken down a particular path depending on responses to previous questions (see figure 1). Participants were asked questions pertaining to their demographics, mobile phone ownership (including type of mobile phone), and their awareness and usage of medical apps.
Participants who owned a smartphone were presented with ten purposes for which they may use medical apps (e.g., accessing clinical handbooks). For each purpose that participants used medical apps, they were asked to rate how useful they found them for that purpose on a scale from 0 to 100 (0 = not useful; 100 = very useful). Subsequently, participants were instructed to indicate their level of agreement with nine statements pertaining to their attitudes towards the use of medical apps on a scale ranging from 0 to 100 (0 = strongly disagree; 100 = strongly agree).
Results
A total of 594 students participated in the study (i.e., a response rate of 25%). However, not all students completed all survey questions that applied to them. A total of 241 students were in their pre-clinical years, 325 were in their clinical years, and 28 students were completing their Bachelor of Medical Science (Honours) year. The mean age of the students was 22.4 years (n = 591; SD = 2.9; range = 17 – 48 years). All students owned a mobile phone.
Students with smartphones
As can be seen in figure 1, 77% of students had a mobile phone with application support (i.e., a smartphone). Ninety-five per cent of these students were aware of medical apps prior to the survey. Most students became aware of medical apps from fellow medical students (n = 362), followed by app stores (n = 317), clinicians (n = 169), websites (n = 143), other healthcare professionals (n = 63) and other sources (n = 29). Thirty-two per cent of students who were aware of medical apps indicated that a medical educator had recommended a specific medical app.
Seventy-six per cent of students who were aware of medical apps had them on their smartphone and the majority of these students found them useful (see figure 1). Most students (n = 126) used medical apps on a weekly basis, while the remaining students reported using them monthly (n = 65), daily (n = 62), more than once a day (n = 44), and yearly or less (n = 27). Medical apps were most commonly used in a self-study setting (n = 240), followed by in a clinical-based setting (n = 211), in lectures (n = 146), tutorials (n = 142), and other settings (n = 31).
Students who used medical apps were asked to rate how useful they found medical apps for various purposes on a scale from 0 (not useful) to 100 (very useful). Mean values of students’ ratings were calculated (see Table 1). Medication/drug guide apps were the most commonly used and most useful type of medical app.
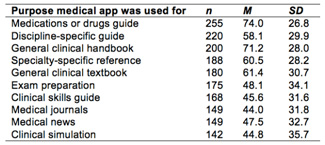
Table 1. Descriptive statistics pertaining to how useful medical students found their medical apps for various purposes on a 0-100 scale (0 = not useful; 100 = very useful). The number of students that used medical apps for the specified purpose is also indicated.
As can be seen in table 2, the most frequently used app was Medscape which is a comprehensive application for healthcare professionals containing features such as drug references, medical calculators, and professional directories to search for medical facilities. Epocrates, which is similar to Medscape in that it contains drug references, was the second most used app. Eponyms, which enables individuals to obtain a short description of medical eponyms, was the third most used app.
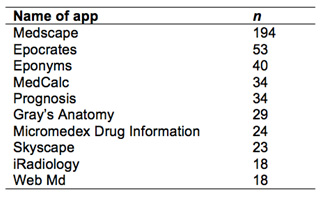
Table 2. The ten most commonly used medical apps among medical students and the number of medical students who use these apps.
Students who had medical apps were generally of the opinion that they were easy to obtain, covered a wide range of topics, had reliable content and were convenient to use in clinical settings (see Table 3). Furthermore, these students were looking to obtain more medical apps and would recommend them to fellow medical students. However, students who had medical apps generally did not rely heavily on them for their medical learning, and believed that they could not replace conventional textbooks or handbooks.
Twenty-four per cent of students who owned a smartphone and were aware of medical apps did not have them on their device. These students indicated the following reasons for not having medical apps: medical apps are unnecessary (n = 30), unsure how to obtain medical apps (n = 29), perceived medical apps too expensive (n = 15), did not trust the apps’ content (n = 4), had unfavourable experiences with medical apps (n = 4) and/or stated other reasons (n = 22). However, approximately 95% of these students indicated that they would consider acquiring medical apps in the future.
Five per cent of students who owned a smartphone were unaware that medical apps existed. Ninety per cent of these students indicated that they would consider acquiring medical apps now that they knew about them (see Figure 1).

Table 3. Medical students’ (n = 307) mean level of agreement with statements in regards to medical apps on a 0-100 scale (0 = strongly disagree; 100 = strongly agree).Students without smartphones
As can be seen in figure 1, 23% of students had a mobile phone without app support. Most (95%) of these students were aware of medical apps prior to the survey. Seventy-two per cent of students that had a mobile phone without app support, irrespective of their prior awareness of medical apps, indicated that they would consider obtaining a smartphone so that they can access medical apps.
Discussion
All medical students within our study owned a mobile phone with the majority owning a smartphone. Furthermore, our study shows that 72% of Monash University medical students with smartphones are already using medical apps, a finding which is similar to Wallace et al.’s study involving medical students in Canada16. Students without smartphones were generally prepared to obtain one so that they can use medical apps. Only 3% of students indicated that they would not consider obtaining medical apps or a smartphone so that they can use medical apps. Overall, from an access to devices perspective, these findings suggest that most medical students at Monash University are ready for medical apps to be used as part of their education or that they are prepared to obtain a smartphone so that they can access them.
Generally medical students that used medical apps indicated that apps are easy to obtain and were perceived to be reliable in terms of their content. Furthermore students indicated that they are looking to obtain more apps and would recommend them to fellow medical students. These results suggest that medical students who are already using medical apps generally have positive attitudes towards them.
However, despite medical students generally having positive attitudes towards medical apps, they still have some reservations in regards to using them compared to traditional study materials. Most students predominantly use sources other than apps (e.g., books) to study and generally felt that medical apps cannot replace the use of traditional handbooks/textbooks. This is quite surprising given that 61% and 55% of students with medical apps indicated that they use them to access clinical handbooks and clinical textbooks respectively and rated them favourably. Unlike textbooks and journals, there is no official peer review process for apps and thus students may be sceptical of the content unless being able to confirm the information with a textbook.
At first glance the findings that apps cannot replace textbooks and students accessing textbooks via apps appears to be contradictory, especially since medical apps were also most commonly reported to be used in a self-study context. However, the location where students’ self-study takes place could explain these findings. Students may access textbook/handbook apps as a quick reference tool when studying while on the public transport, when waiting between classes, or on clinical placement given that a smartphone is portable and thus readily available. On the other hand, students may prefer hardcopy textbooks/handbooks when studying at home, such as when preparing for assignments and exams, given that mobile phone screens are relatively small. Another plausible explanation for these seemingly contradictory findings is that the current generation of medical students is at the beginning of the emergence of technological advances such as medical apps. Thus these students may be retaining traditional study means (e.g., hardcopies of books) while utilising new technologies (e.g., medical apps) to study. In addition, these students will be influenced by their medical educators in regards to what sources they recommend for study. Perhaps a change in this trend will emerge within the next decade of medical students as medical apps become more popular, especially if curricular changes encourage their use. Further research would be needed to fully explore medical students’ uses of medical apps and textbooks for study purposes.
Limitations
Unfortunately only 25% of Monash University medical students participated in our study. Our low response rate could be attributed to: 1) our study being conducted just prior to the end of year examination period and students having many assessments due at that time; and 2) medical students generally being over surveyed and consequently suffering from survey fatigue. Furthermore, it is possible that students without a mobile phone thought that the study was not applicable to them and thus did not participate. However, we anticipate that only a small percentage of students, if any, would fall into this category given the anecdotal evidence of a high prevalence of mobile phone ownership amongst teenagers and those in their twenties.
Conclusion
Our findings show that Monash University medical students appear to be ready for and accepting of medical apps to be used during their medical education. Thus medical schools should consider incorporating the use of medical apps within their curriculum.
References
- Ducut, E., & Fontelo, P. (2008). Mobile devices in health education: Current use and practice. Journal of Computing in Higher Education, 20, 59-68.

- Peterson, M. W., Rowat, J., Kreiter, C., & Mandel, J. (2004). Medical students’ use of information resources: Is the digital age dawning? Academic Medicine, 79, 89-95.

- Schlenker, M., & Park, J. (2008). Are printed textbooks obsolete in medical education? University of Toronto Medical Journal, 86, 27-29.
- Boulos, M. N. K., Wheeler, S., Tavares, C., & Jones, R. (2011). How smartphones are changing the face of mobile and participatory healthcare : An overview, with example from eCAALYX. Biomedical Engineering Online, 10, 24.

- Phillippi, J. C., & Wyatt, T. H. (2011). Smartphones in nursing education. Computers, Informatics, Nursing, 29, 449-454.

- Savel, R. H., & Munro, C. L. (2011). Scalpel, stethoscope, iPad: The future is now in the intensive care unit. American Journal of Critical Care, 20, 275-277.

- Burdette, S. D., Herchline, T. E., & Oehler, R. (2008). Practicing medicine in a technological age: Using smartphones in clinical practice. Clinical Infectious Diseases, 47, 117-122.

- Havelka, S. (2011). Mobile resources for nursing students and nursing faculty. Journal of Electronic Resources in Medical Libraries, 8, 194-199.

- Dasari, K. B., White, S. M., & Pateman, J. (2011). Survey of iPhone usage among anaesthetists in England. Anaesthesia, 66, 620–631.
- Franko, O. I., & Tirrell, T. F. (2011). Smartphone app use among medical providers in ACGME training programs. Journal of Medical Systems [Online]. Available: http://www.springerlink.com/content/p6t82ph541835u75/
- Franko, O. I. (2011). Smartphone apps for orthopaedic surgeons. Clinical Orthopaedics and Related Research, 469, 2042–2048.
- Flannigan, C., & McAloon, J. (2011). Students prescribing emergency drug infusions utilising smartphones outperform consultants using BNFCs. Resuscitation, 82, 1424-1427.

- Baumgart, D. C. (2011). Smartphones in clinical practice, medical education, and research. Archives of Internal Medicine, 171, 1294-1296.

- Fried, J. J. (2012). Images at your fingertips. Community Oncology, 9, 141-142.

- Chatterley, T., & Chojecki, D. (2010). Personal digital assistant usage among undergraduate medical students: exploring trends, barriers, and the advent of smartphones. Journal of the Medical Library Association, 98, 157-160.

- Wallace, S., Clark, M., & White, J. (2012). ‘It’s on my iPhone’: attitudes to the use of mobile computing devices in medical education, a mixed-methods study. British Medical Journal, 2, e001099.

- Medical Deans Australia and New Zealand (2011). 2011 Medical Students Statistics, viewed 27th November 2012,http://www.medicaldeans.org.au/wp-content/uploads/Table-2-Website-Stats-2011.pdf

